Understanding Achilles Tendinitis
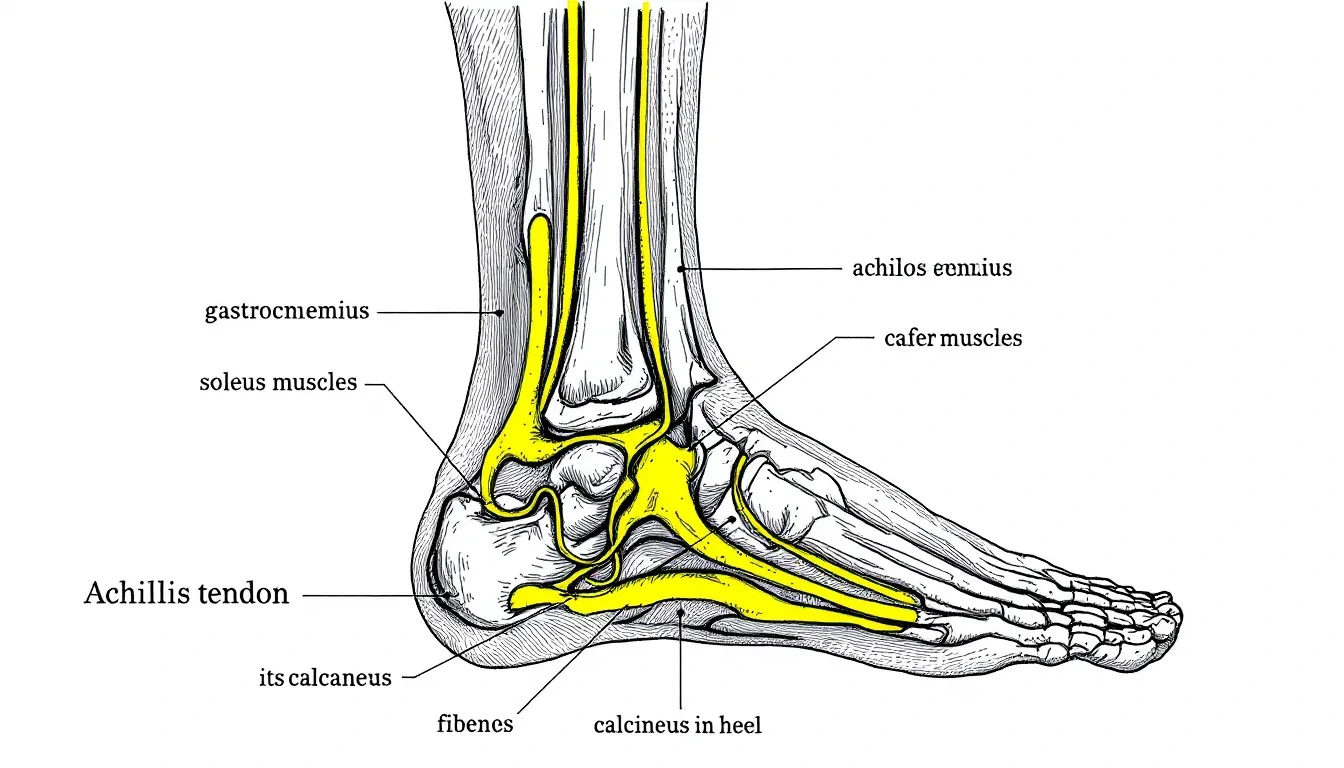
The achilles tendon is a remarkable piece of anatomy—a thick, fibrous cord that connects your calf muscles to your heel bone, enabling you to walk, run, jump, and rise up on your tiptoes. This essential structure can withstand enormous forces, experiencing loads up to 12.5 times your body weight during high-impact activities like running and jumping.
Importance of Routine Diabetic Foot Exams
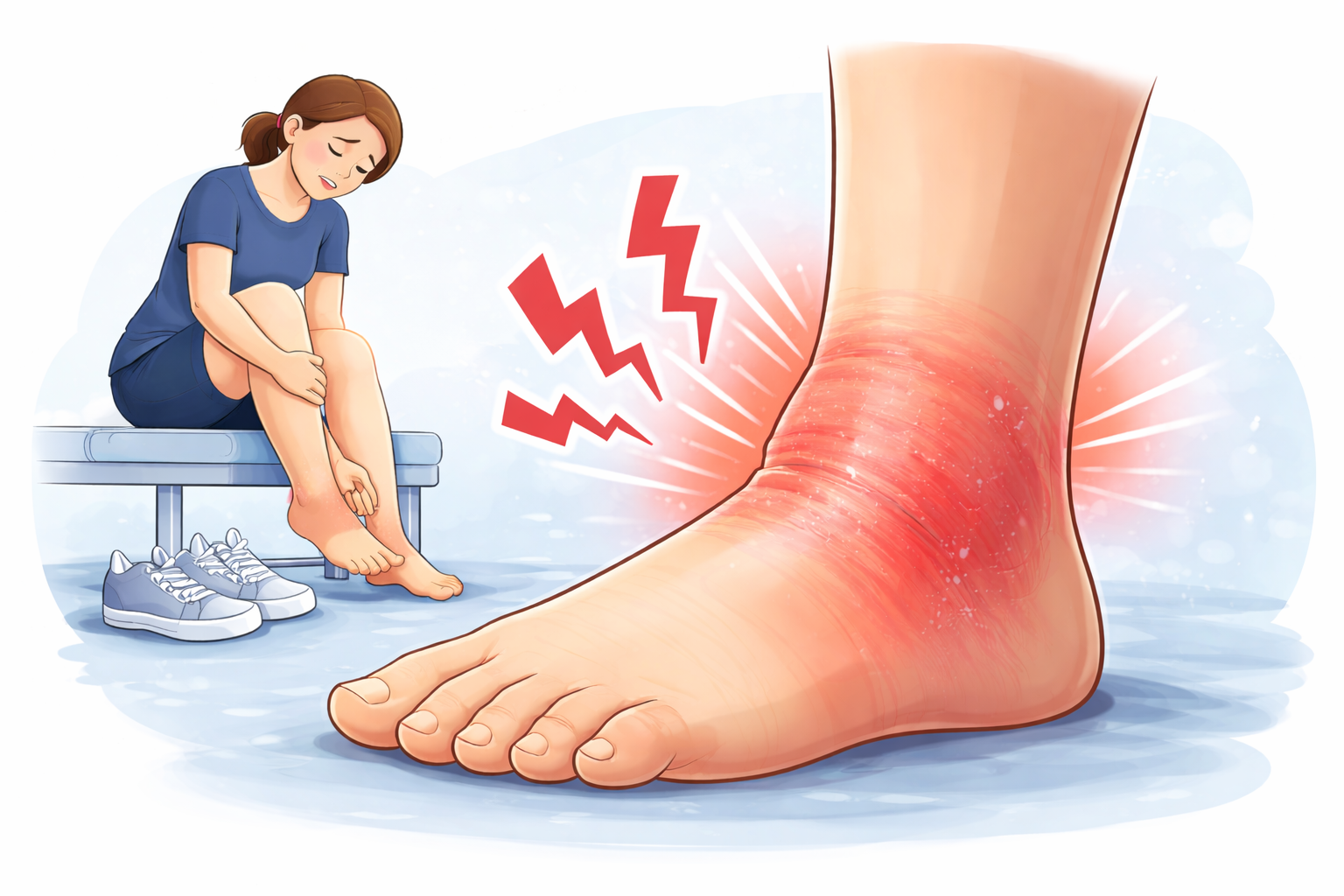
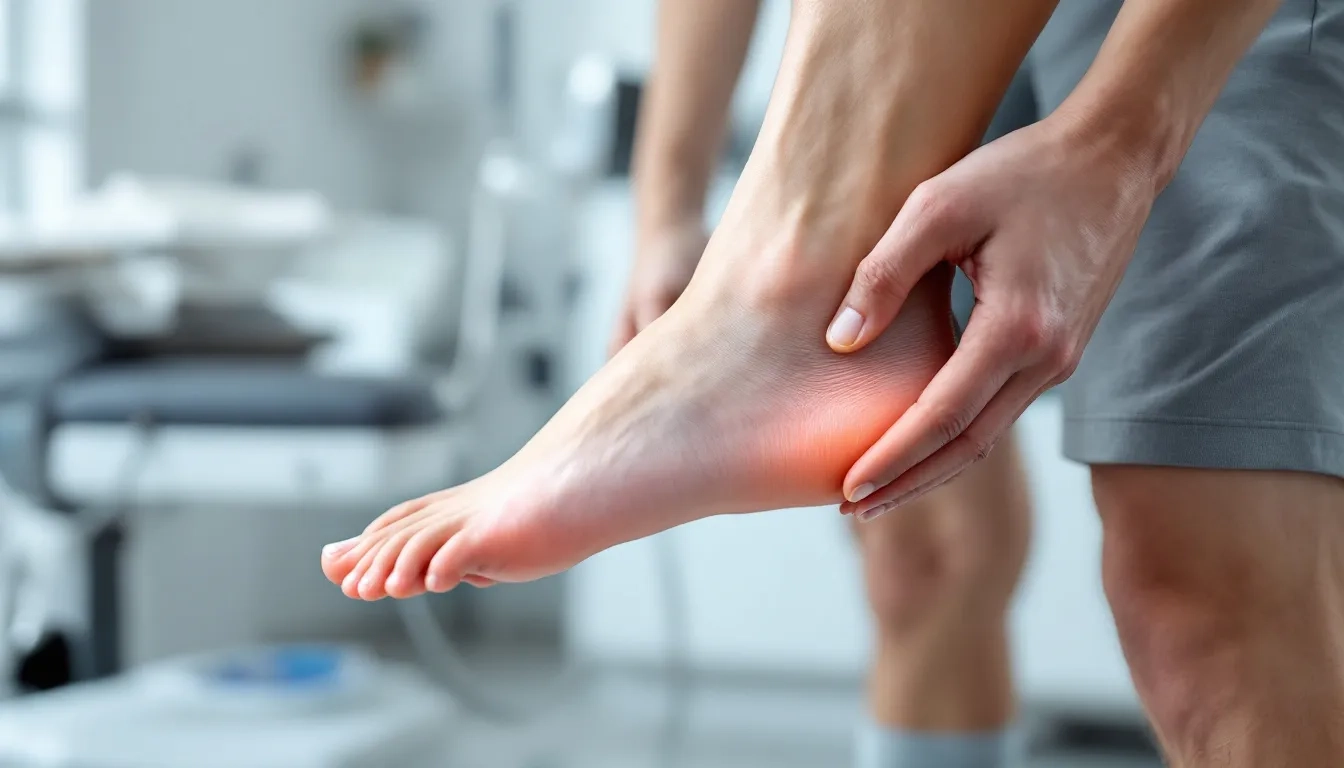
When this crucial tendon becomes overloaded or subjected to repetitive stress, it can develop microscopic tears and inflammation, leading to the condition we know as achilles tendinitis. The affected area becomes painful, swollen, and tender to the touch, making normal physical activity uncomfortable or even impossible.
This condition primarily affects active individuals between 30 and 50 years old, though it can occur in younger athletes and older adults as well. Men are more commonly affected than women, and the incidence rate jumps significantly among runners and athletes compared to the general population. Understanding who’s at risk helps both in prevention and early recognition of symptoms.
What Is Achilles Tendinitis?
Medically speaking, achilles tendinitis refers to irritation, inflammation, or degeneration of the achilles tendon—the large, strong fibrous cord connecting your calf muscles (specifically the gastrocnemius and soleus muscles) to the heel bone (calcaneus). This vital connection allows your calf muscle to generate the power needed for walking, running, and jumping.
It’s important to understand the distinction between tendinitis and tendinopathy, terms often used interchangeably but with subtle differences. Tendinitis implies active inflammation of the tendon, while tendinopathy encompasses a broader range of tendon problems, including degenerative changes that occur over time.
Modern research shows that chronic achilles tendon pain often involves tendinopathy—a failed healing response characterized by tissue degeneration rather than classic inflammation.
The condition develops gradually as repetitive motion and mechanical stress exceed the tendon’s ability to repair itself. Instead of healthy, organized collagen fibers, the injured tissue develops areas of degeneration with fragmented fibers, increased ground substance, and abnormal blood vessel growth.
This process explains why achilles tendinitis can be particularly stubborn to treat and why proper diagnosis and treatment are essential for full recovery.
Types of Achilles Tendinitis

Healthcare professionals recognize two distinct types of achilles tendinitis, each with unique characteristics and treatment considerations:
1. Noninsertional Achilles Tendinitis
Noninsertional achilles tendinitis affects the middle portion of the tendon, typically occurring 2-6 centimeters above where the tendon attaches to the heel bone. This type accounts for approximately 75% of all achilles tendinitis cases and primarily involves degenerative changes in the tendon tissue.
This form of the condition typically affects younger, more active individuals and athletes who subject their tendons to high mechanical loads. The noninsertional achilles tendinitis responds better to conservative treatments, particularly eccentric exercise programs, compared to its insertional counterpart.
2. Insertional Achilles Tendinitis
Insertional achilles tendinitis occurs at the achilles tendon insertion point where the tendon attaches directly to the heel bone. This type often involves not just tendon degeneration but also bone spurs, calcification, and inflammation of the nearby retrocalcaneal bursa.
The insertional type typically affects older, less active individuals and tends to be more challenging to treat conservatively. Patients with insertional achilles tendinitis often require longer recovery periods and may be more likely to need surgical intervention if nonsurgical treatments fail.
Understanding which type affects you is crucial because treatment approaches can vary significantly. Your physical therapist or orthopaedic surgeons can determine the specific type through physical exam and imaging tests when necessary.
Common Symptoms of Achilles Tendinitis and Warning Signs
Recognizing the symptoms of achilles tendinitis early can prevent a minor issue from becoming a chronic, debilitating problem. The condition typically develops gradually, with symptoms worsening over time if left untreated.
The hallmark symptom is pain along the achilles tendon, particularly noticeable during the first steps in the morning or after periods of rest. This pain often improves with gentle movement but worsens with increased activity. Many patients describe it initially as a mild ache that progresses to more severe tendon pain if ignored.
Key warning signs include:
Morning stiffness and pain that gradually improve with movement
Activity pain that worsens during or after exercise
Tendon swelling and thickening you can feel when touching the affected area
Heel pain that radiates up the back of the lower leg
Reduced flexibility in the affected foot and ankle
Crackling sensation (crepitus) when moving the ankle
The pain pattern is particularly telling—it typically starts as discomfort at the beginning of activity, may improve during exercise as the tendon warms up, then returns with greater intensity after activity ends. This characteristic pattern helps distinguish achilles tendinitis from other tendon injuries.
More serious warning signs that require immediate medical attention include sudden, severe pain that might indicate an achilles tendon rupture, inability to bear weight on the affected foot, or a complete loss of strength when trying to push off with your toes.
Advanced Treatments for Diabetic Foot Complications
What Causes Achilles Tendinitis?
Understanding the underlying causes of achilles tendinitis helps both in treatment and prevention. The condition typically results from a combination of factors rather than a single cause.
Overuse and Repetitive Stress
The most common cause is repetitive stress that exceeds the tendon’s capacity to heal and adapt. This repetitive motion gradually breaks down the tendon’s collagen structure, leading to microscopic tears and eventually pain and dysfunction.
Activities that involve repeated heel lifting, such as running, jumping, or dancing, are particularly problematic.
Sudden Activity Increases
Weekend warriors are particularly susceptible when they dramatically increase their physical activity after periods of inactivity. The “too much, too soon” approach overwhelms the tendon’s ability to adapt, leading to injury.
Even experienced athletes can develop problems when they suddenly increase training intensity, duration, or frequency without proper progression.
Age-Related Changes
As we age, our tendons naturally become less elastic and more prone to injury. The achilles tendon’s blood supply decreases with age, reducing its ability to heal from minor damage.
This explains why achilles tendinitis becomes more common in middle-aged adults, even those who have been active their entire lives.
Biomechanical Factors
Several biomechanical issues can predispose individuals to achilles tendinitis:
Tight calf muscles that increase tension on the tendon
Weak calf muscles that cannot properly support the demands placed on the tendon
Poor foot biomechanics, including overpronation or high arches
Improper footwear that doesn’t provide adequate support or heel cushioning
Medical Conditions
Certain health conditions increase the risk of developing achilles tendinitis. Diabetes can impair healing and increase susceptibility to tendon problems. High blood pressure, obesity, and high cholesterol also contribute to increased risk.
Additionally, some medications, particularly fluoroquinolone antibiotics and corticosteroids, can weaken tendons and predispose them to injury.
Environmental factors like exercising in cold weather or on hard surfaces can also contribute to tendon problems, as can sudden changes in training surfaces or footwear.
Diagnosis and Medical Evaluation
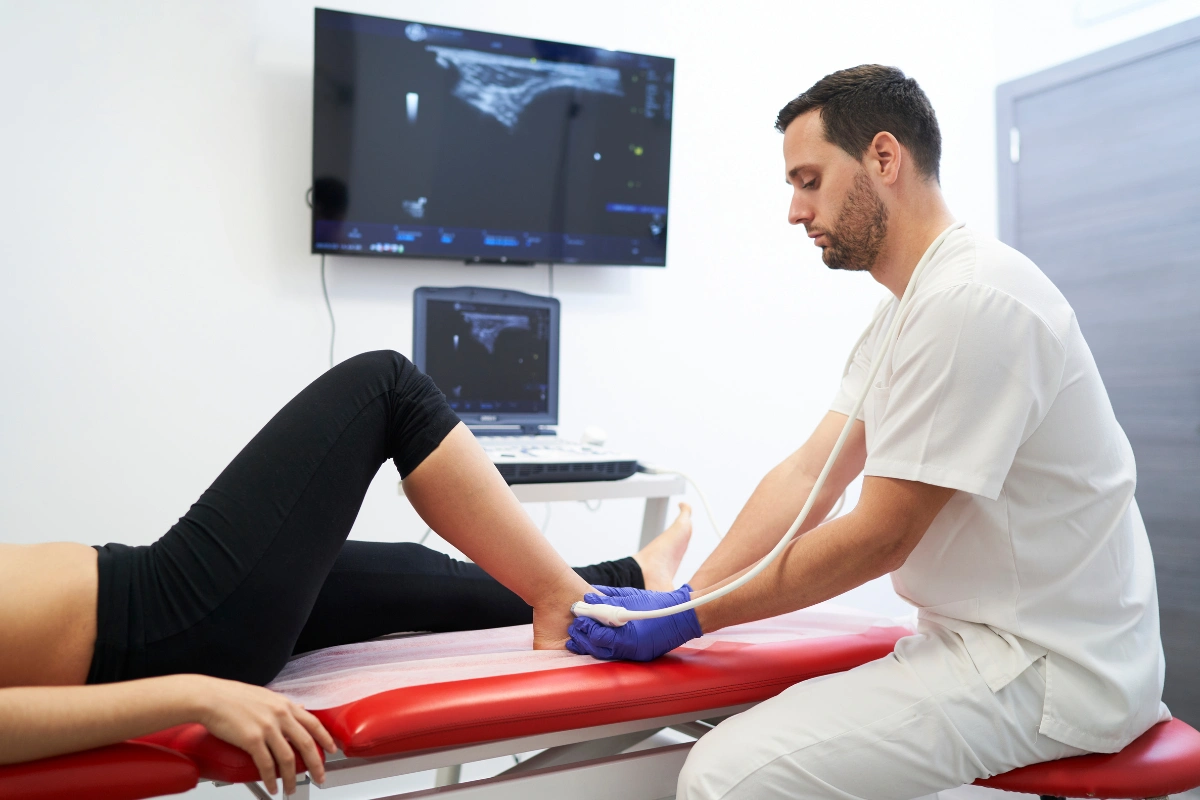
Proper diagnosis is crucial for effective treatment of achilles tendinitis. Healthcare providers use a combination of clinical evaluation and, when necessary, imaging studies to diagnose achilles tendinitis and rule out other conditions.
Physical Examination
The diagnostic process begins with a thorough physical exam. Your healthcare provider will palpate the tendon to identify areas of tenderness, swelling, or thickening. They’ll assess your ankle’s range of motion and test the strength of your calf muscles.
Specific tests help confirm the diagnosis:
Royal London Hospital test: Tenderness that decreases when the ankle is bent upward suggests achilles tendinitis
Painful arc test: Identifies the specific location of tendon problems
Calf raise test: Evaluates the tendon’s functional capacity
When Imaging Is Needed
Most cases of achilles tendinitis can be diagnosed clinically without imaging tests. However, magnetic resonance imaging (MRI) or ultrasound may be recommended in certain situations:
When symptoms don’t improve with conservative treatment
To rule out an achilles tendon rupture
When surgical planning is necessary
To assess the extent of tendon damage or degeneration
Ultrasound offers real-time visualization of the tendon and can detect areas of degeneration, thickening, or partial tears. MRI provides the most detailed view of tendon structure and is considered the gold standard for surgical planning.
Ruling Out Other Conditions
Several conditions can mimic achilles tendinitis, making an accurate diagnosis essential. These include partial achilles rupture, retrocalcaneal bursitis, and referred pain from the lumbar spine.
Your healthcare provider will carefully evaluate your symptoms and examination findings to ensure you receive the correct diagnosis and appropriate treatment.
Early professional evaluation is particularly important because untreated achilles tendinitis can progress to more serious problems, including complete achilles rupture, which requires surgical repair and extensive rehabilitation.
Achilles Tendinitis Treatment Options That Work
Effective treatment of achilles tendinitis requires a comprehensive approach tailored to the specific type and severity of your condition. The good news is that most patients—over 80%—recover successfully with nonsurgical treatment when properly implemented.
1. Conservative Treatment Approaches
The foundation of achilles tendinitis treatment begins with conservative management:
R.I.C.E. Method: Rest, ice, compression, and elevation form the initial treatment approach. However, complete rest isn’t always ideal—controlled, pain-free movement often promotes better healing than complete immobilization.
Activity Modification: Rather than stopping all activity, modify your routine to avoid movements that aggravate symptoms. This might mean switching from running to swimming or cycling while your tendon heals.
Supportive Shoes and Orthotics: Proper footwear with adequate heel cushioning can significantly reduce stress on the achilles tendon. Heel lifts temporarily reduce tendon tension, while custom orthotics address underlying biomechanical issues.
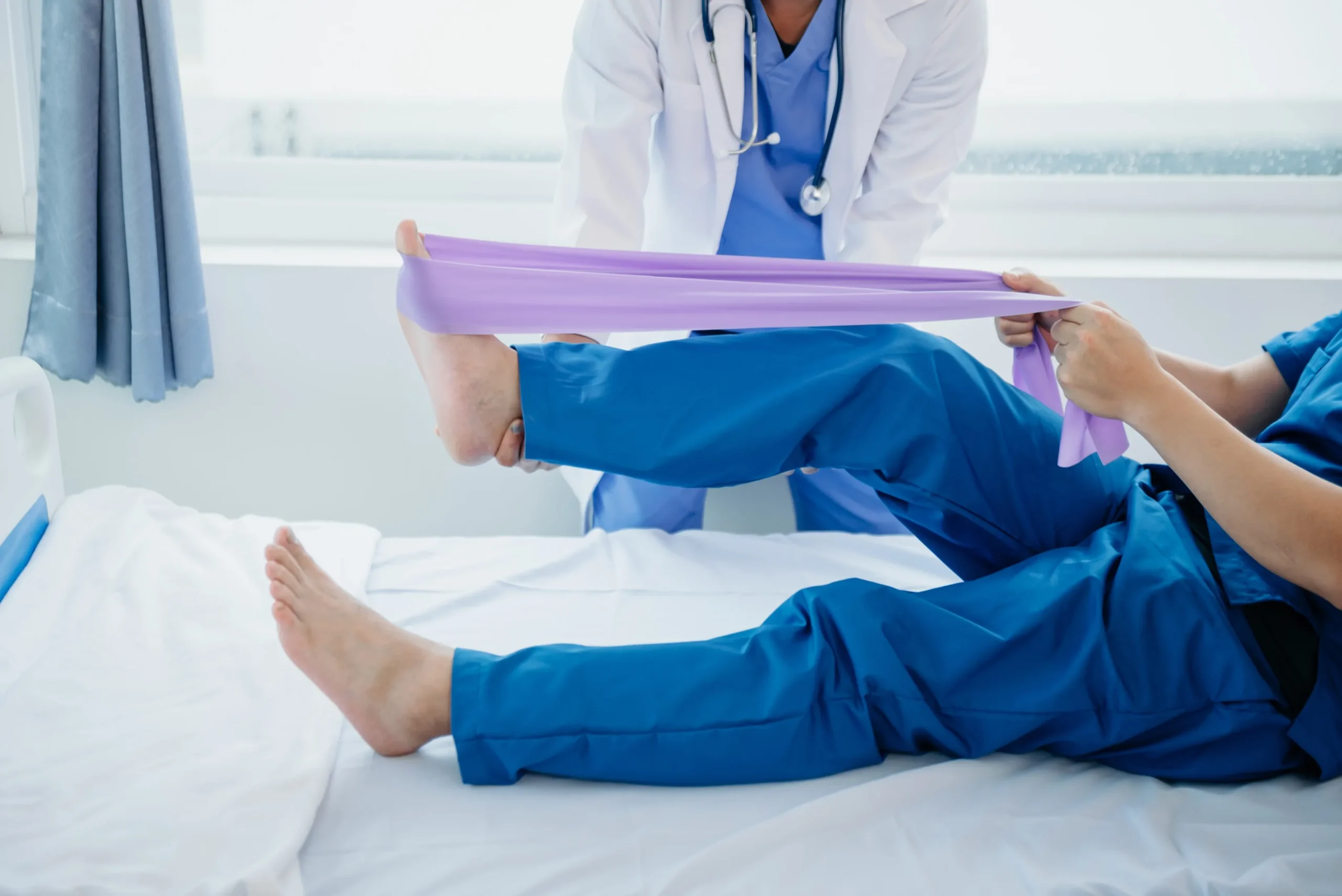
2. Physical Therapy and Exercise
Physical therapy represents the cornerstone of successful achilles tendinitis treatment. A skilled physical therapist will design a program specifically for your condition and recovery goals.
Eccentric Exercises: These specialized strengthening exercises, where the muscle lengthens while contracting, have shown remarkable success in treating achilles tendinopathy. Research demonstrates that up to 82% of patients experience significant symptom improvement within three months when properly performing eccentric calf exercises.
The exercises work by promoting healthy tissue remodeling and improving the tendon’s ability to handle mechanical loads. Your physical therapist will teach you the proper technique and progression to maximize benefits while avoiding further injury.
3. Pain Management
Anti-inflammatory medications can provide short-term pain relief, though they offer limited benefit for chronic degenerative tendinopathy. Your healthcare provider may recommend NSAIDs for acute symptoms while emphasizing that addressing the underlying tendon problem requires more comprehensive treatment.
For some patients, a walking boot may be necessary during severe flare-ups to reduce pain and allow the initial healing process to begin.
4. Advanced Treatment Options
When conservative treatments don’t provide sufficient relief after several months, advanced therapies may be considered:
Extracorporeal Shock Wave Therapy: Also known as extracorporeal shockwave therapy, this treatment uses acoustic waves to stimulate healing in degenerative tendons. While not all patients respond, many experience significant pain reduction and improved function.
Injection Therapies: Platelet-rich plasma (PRP) injections show promise in some patients, though research results remain mixed. It’s important to note that corticosteroid injections are contraindicated for achilles tendinitis due to the risk of tendon rupture.
5. Surgical Intervention
Achilles tendinitis surgery becomes necessary for fewer than 10% of patients when nonsurgical treatments fail after six months or more of consistent conservative management. Surgical procedures may include:
Tendon debridement to remove unhealthy tissue
Removal of bone spurs in insertional cases
Tendon repair for partial tears
In severe cases, tendon transfer procedures
Post-surgical rehabilitation is crucial for optimal outcomes and typically involves several months of progressive physical therapy to restore strength and function.
Prevention Strategies

Preventing achilles tendinitis is far easier than treating it, and many cases can be avoided with proper attention to risk factors and training principles.
1. Proper Warm-Up and Stretching
Always begin physical activity with a thorough warm-up that gradually increases blood flow to your muscles and tendons. Dynamic stretching before activity and static stretching afterward can help maintain calf muscle flexibility and reduce tendon tension.
Focus particularly on calf muscle stretches, as tight calf muscles significantly increase stress on the achilles tendon. Hold stretches for at least 30 seconds and repeat them several times for maximum benefit.
2. Gradual Activity Progression
Follow the “10% rule” when increasing training intensity or duration—never increase your activity level by more than 10% per week. This gradual progression allows your tendons time to adapt to increased demands without becoming overwhelmed.
If you’re returning to activity after time off, be especially conservative in your progression. It often takes several weeks or months to safely return to previous activity levels.
3. Footwear and Equipment
Invest in quality athletic shoes appropriate for your specific activities. Replace shoes regularly—typically every 300-500 miles for runners—as worn shoes lose their shock-absorbing properties. Consider heel lifts or custom orthotics if you have biomechanical issues that predispose you to tendon problems.
4. Strength and Flexibility Maintenance
Maintain strong, flexible calf muscles through regular strengthening exercises and stretching. Eccentric calf exercises aren’t just for treating achilles tendinitis—they’re also excellent for prevention. Include both gastrocnemius and soleus muscle exercises in your routine.
Cross-training with low-impact activities like swimming or cycling can maintain fitness while reducing repetitive stress on your achilles tendons. This approach is particularly valuable for runners and other athletes who perform repetitive heel-strike activities.
5. Listen to Your Body
Pay attention to early warning signs like morning stiffness or mild tendon pain. Address these symptoms immediately with rest, ice, and gentle stretching rather than pushing through discomfort. Early intervention can prevent minor tendon irritation from progressing to chronic tendinopathy.
Evolve Health - Your Partner in Recovery
At Evolve Health, we understand that achilles tendinitis can significantly impact your active lifestyle and daily comfort. Our comprehensive approach to foot and ankle Services combines the latest evidence-based treatments with personalized care plans designed to get you back to the activities you love.
Our experienced team of specialists works collaboratively to address not just your immediate symptoms, but also the underlying factors that contributed to your condition, ensuring long-term success and helping prevent future injuries.
Frequently Asked Questions
How long does Achilles tendinitis take to heal?
Recovery time varies significantly depending on the severity and chronicity of your condition. With proper conservative management, many patients experience substantial improvement within 3-6 months. However, some chronic cases may require 6-12 months or longer for complete resolution. Early treatment typically leads to faster recovery, which is why seeking prompt medical attention for persistent heel pain is crucial.
Can I continue exercising with Achilles tendinitis?
Complete activity cessation isn’t always necessary or beneficial. The key is modifying your activities to avoid aggravating movements while maintaining general fitness. Swimming, cycling, and upper body exercises typically don’t stress the achilles tendon. Our Doctors at Evolve Health can help you develop an appropriate exercise program that promotes healing while maintaining fitness.
Do I need imaging tests for diagnosis?
Most cases of achilles tendinitis can be accurately diagnosed through physical examination alone. Imaging tests like ultrasound or MRI are typically reserved for cases that don’t respond to conservative treatment, when surgical planning is necessary, or to rule out complications like tendon rupture.
What shoes should I wear during recovery?
Supportive shoes with good heel cushioning are essential during recovery. Avoid flat shoes, flip-flops, or worn-out athletic shoes. Many patients benefit from heel lifts that temporarily reduce tension on the achilles tendon. Your healthcare provider may recommend specific footwear or orthotic devices based on your individual needs and biomechanics.
When should I see a specialist?
Consider seeing a specialist if your symptoms persist despite 2-3 weeks of conservative self-care, if you experience severe pain that limits daily activities, or if you suspect a more serious injury like an achilles rupture. Sports medicine physicians, orthopaedic surgeons, and physical therapists all play important roles in diagnosing and treating achilles tendon problems.
Conclusion
Achilles tendinitis doesn’t have to sideline you indefinitely. With proper diagnosis, appropriate treatment, and consistent rehabilitation, most people can successfully return to their desired activity levels and prevent future episodes. The key is recognizing symptoms early and seeking appropriate care before minor tendon irritation progresses to chronic, degenerative changes.
Remember that conservative treatment succeeds in the vast majority of cases, but it requires patience and consistency. Whether you’re dealing with insertional or non-insertional achilles tendinitis, working with experienced healthcare providers who understand the latest treatment approaches can make all the difference in your recovery.
Don’t let heel pain keep you from the activities you love. Take the first step toward recovery by finding a location near you and scheduling your comprehensive evaluation today.