What Is Toenail Fungus (Onychomycosis)?
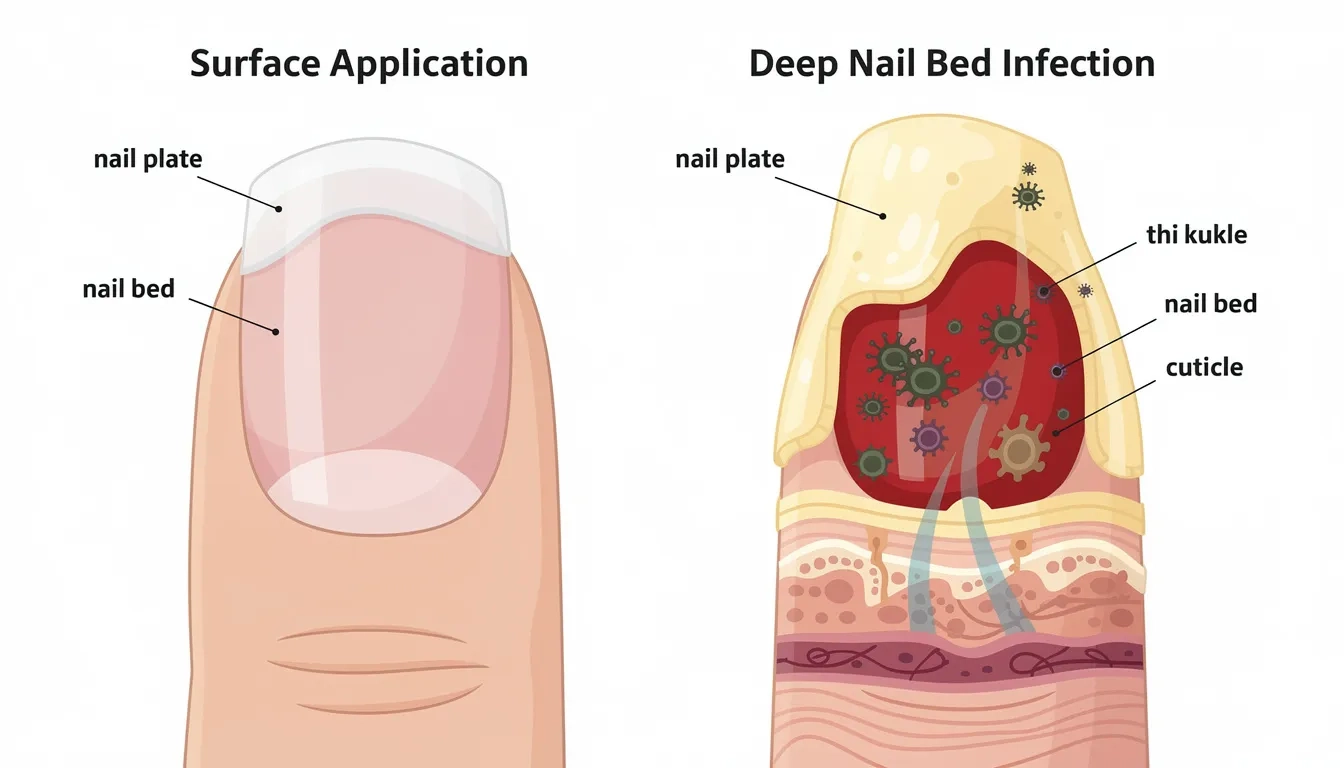
Toenail fungus, medically known as onychomycosis, is a chronic fungal infection that affects the nail plate, nail bed, and sometimes the surrounding tissue. Unlike a simple surface problem, this stubborn infection penetrates deep into the keratin structure of your toenails, making it notoriously difficult to eliminate with basic antifungal treatments.
The fungus can also infect the skin beneath the nail, which makes treatment more challenging because topical medications must reach both the nail and the skin beneath to be effective.
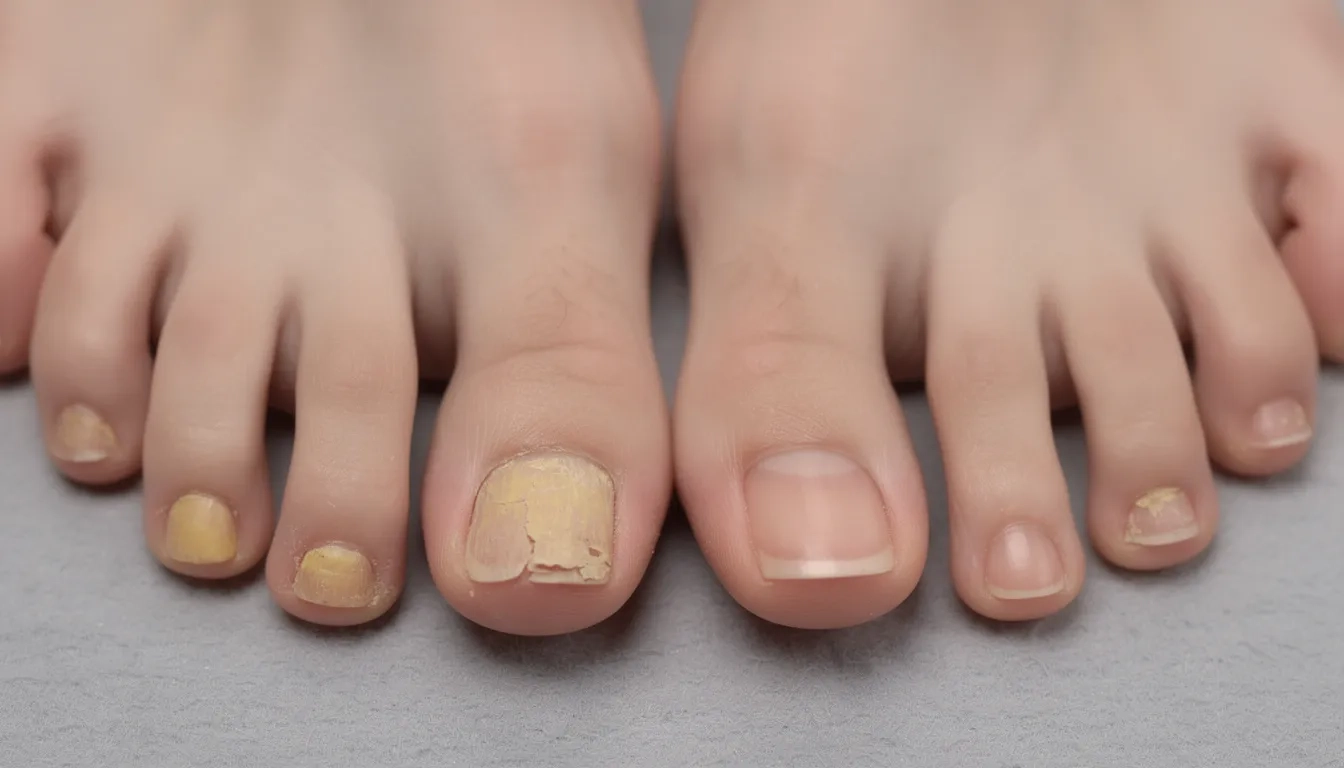
The condition typically manifests as yellowing, thickening, or browning of one or more toenails, often starting at the tip or edges and gradually spreading toward the base.
As the infection progresses, nails may become brittle, crumbly, or separate from the underlying nail bed, creating space where debris accumulates and fungus thrives.
Key characteristics of toenail fungus include:
Discoloration: Yellow, white, or brown streaks or patches
Thickening: Nails become difficult to trim and may curve abnormally
Texture changes: Brittle, crumbly, or powdery debris under the nail
Separation: Nail plate lifts away from the nail bed (onycholysis)
Odor: Musty or unpleasant smell from infected nails
Shape distortion: Nails may become misshapen or ingrown
Dermatophytes, particularly Trichophyton rubrum and T. mentagrophytes, cause approximately 90% of toenail infections. These microscopic fungi feed specifically on keratin—the protein that makes up your hair, skin, and nails—allowing them to establish persistent colonies within the nail structure.
The infection develops slowly over months or even years, often beginning as athlete’s foot that spreads from the surrounding skin to the nail edges. Toenail fungus thrives in warm, moist environments, which is why it is common in people who wear closed shoes for long periods or have sweaty feet.
What starts as a small discolored spot can eventually affect the entire nail if left untreated, and the condition becomes increasingly difficult to cure as it advances.
How Toenail Fungus Starts (And Why It Keeps Coming Back)
Understanding how fungal nail infections develop is crucial for both treatment and prevention. Fungal spores are everywhere in our environment, but certain conditions create the perfect storm for these opportunistic organisms to establish infection under your nails.
Common sources of initial infection:
Public facilities and communal areas: Walking barefoot in locker rooms, public showers, pool decks, and gym floors exposes feet to fungal spores
Shared items: Borrowing shoes, using communal nail clippers, or sharing towels can transfer fungi between people
Contaminated pedicure tools: Improperly sterilized instruments at nail salons pose infection risks
Personal footwear: Chronic use of damp, sweaty shoes creates ideal fungal breeding conditions
Wearing flip-flops or sandals in communal areas can help protect against toenail fungus.
Entry points and infection mechanisms:
Microtrauma: Tight shoes, repetitive pressure from running, or nail injuries create microscopic cracks that allow fungal entry
Athlete’s foot progression: Active tinea pedis on surrounding skin frequently spreads to nail edges and under the free edge
Nail damage: Recent pedicures, aggressive cuticle cutting, or ingrown nail treatment can compromise nail barriers
Chronic moisture: Prolonged exposure to wet environments softens nails and increases fungal penetration. Keeping feet dry, especially after bathing or exercise, is important to reduce the risk of fungal infection.
Risk factors that increase susceptibility:
Age over 50: Slower nail growth and reduced circulation make older adults more vulnerable
Diabetes: High blood sugar impairs immune function and wound healing
Poor circulation: Reduced blood flow limits the body’s ability to fight infection
Immune suppression: Medications, chemotherapy, or conditions like HIV reduce antifungal defenses
Occupational exposure: Healthcare workers, athletes, and kitchen staff face higher infection risks
Hyperhidrosis: Excessive foot sweating creates persistently moist conditions
Why infections persist and recur:
The most frustrating aspect of toenail fungus is its tendency to return even after apparent successful treatment. Fungal spores can survive for months in shoes, socks, and household surfaces, essentially reinfecting you from your own environment.
Additionally, the slow growth rate of toenails—approximately 1 to 1.5 millimeters per month—means that even when antifungal treatments kill active fungi, the damaged nail must physically grow out and be replaced by healthy tissue.
Many people unknowingly harbor chronic athlete’s foot between their toes, which serves as a constant reservoir for reinfecting cleared nails. Without addressing both the nail infection and any coexisting skin fungus, the cycle continues indefinitely.
Why Many Drugstore Antifungal Creams Don’t Fix Toenail Fungus
The harsh reality is that most over-the-counter antifungal creams are specifically formulated for skin conditions like athlete’s foot, not for penetrating the dense, keratin-rich structure of infected toenails.
Clotrimazole, for example, is also commonly used to treat jock itch, another fungal skin infection affecting the groin and inner thighs. This fundamental mismatch between product design and target tissue explains why so many people experience frustration when their drugstore purchases fail to clear nail infections.
The nail penetration barrier:
Healthy toenails consist of tightly packed keratin layers that form an effective barrier against moisture, chemicals, and unfortunately, topical medications. Standard antifungal creams containing clotrimazole, miconazole, or even low-concentration terbinafine simply cannot achieve therapeutic levels within the nail plate where fungi reside.
Clotrimazole is a common antifungal ingredient found in over-the-counter creams for toenail fungus. The infection lives not just on the surface, but deep within the nail structure and in the nail bed underneath.
When nails are thickened, distorted, or separated from the nail bed due to chronic infection, this barrier becomes even more formidable. Subungual debris—the crumbly, powdery material that accumulates under infected nails—further blocks medication penetration and provides additional nutrients for fungal growth.
Common Application Mistakes:
Insufficient quantity: Dabbing a small amount of cream on the nail surface without covering edges, cuticles, and skin underneath the free edge
Inconsistent use: Applying medication sporadically rather than daily for the months required to see results
Premature discontinuation: Stopping treatment when nails still look infected, expecting faster results than biologically possible
Ignoring preparation: Failing to trim, file, or clean nails before application reduces already limited penetration
Timeline misunderstandings:
Perhaps the biggest reason OTC treatments appear to “fail” is unrealistic expectations about improvement timelines. Even highly effective prescription medications require 6 to 12 months to show complete results because the infected nail must be entirely replaced by new, healthy growth.
Most people abandon treatment after a few weeks when they see no visible change, not realizing the medication may be working at the microscopic level.
Product limitations:
Many drugstore “nail fungus” products are actually cosmetic treatments designed to improve appearance rather than eliminate infection. These may temporarily make nails look better by filling in ridges or providing coverage, but they don’t address the underlying fungal problem and may even trap moisture, worsening the condition.
The difference between these cosmetic products and actual antifungal medicine is important—only medicines are formulated to treat the infection itself.
Non-medicated oils, vinegar soaks, and hydrogen peroxide treatments popular on social media are often described as home remedies. While these home remedies lack clinical evidence for effectiveness against established toenail infections, they may provide modest benefits for very mild cases or early-stage disease.
Topical Antifungal Creams and Solutions for Toenail Fungus
Topical treatments for toenail fungus include creams, ointments, and nail polishes.
When properly selected and applied, topical antifungals can effectively treat mild to moderate toenail infections—particularly those affecting less than half the nail plate, showing clear nail growth at the base, and involving only a few nails.
The key lies in choosing formulations specifically designed for nail penetration rather than general-purpose skin creams.
Active ingredients and their mechanisms:
Terbinafine: Disrupts fungal cell membrane synthesis, offering fungicidal activity against dermatophytes
Clotrimazole and miconazole: Azole antifungals that inhibit ergosterol synthesis, primarily fungistatic
Ciclopirox: Broad-spectrum agent that chelates metal ions essential for fungal enzyme function
Tolnaftate: Prevents ergosterol formation, particularly effective in combination with penetration enhancers
Amorolfine: Dual-action morpholine that disrupts fungal cell membrane integrity
Efinaconazole and tavaborole: Newer prescription agents designed specifically for nail penetration
Formulation types and their applications:
A variety of nail fungus treatments are available as topical products, including:
Creams and ointments: Best suited for treating surrounding skin, nail folds, and coexisting athlete’s foot
Solutions and lacquers: Formulated with solvents and penetration enhancers to traverse nail keratin
Medicated polishes: Provide sustained drug delivery while allowing some cosmetic coverage
Combination products: Often include urea or other keratolytics to soften and thin nail plates
Optimal application protocol:
Preparation phase: Soak feet in warm water for 5-10 minutes to soften nail tissue
Mechanical preparation: Trim nails straight across and file down thickened areas with a disposable emery board
Cleaning: Remove debris from under the nail and around cuticles with sanitized tools
Application: Apply medication to entire nail surface, edges, underneath the free edge, and surrounding skin
Drying: Allow complete absorption before putting on socks or shoes
Consistency: Repeat daily or as directed for the full treatment duration
Realistic timeline expectations:
8-12 weeks: Initial signs of improvement may become visible as clear nail begins growing from the base
4-6 months: Smaller toenails may show significant clearing
9-12 months: Large toenails typically require nearly a full year for complete replacement
Ongoing maintenance: Many clinicians recommend continued weekly application for several months after visible clearing
Enhancing topical effectiveness:
Regular mechanical debridement—professionally filing or trimming thickened nails every 4-6 weeks—can dramatically improve drug penetration. Some patients benefit from using 20-40% urea creams under medical supervision to soften and thin stubborn nail plates before applying antifungal medications.
The addition of antifungal powder or spray in shoes helps reduce fungal load and prevents reinfection from contaminated footwear during the extended treatment period.
Prescription-Strength Topical Options
When over-the-counter products prove insufficient, prescription topical agents offer superior nail penetration and clinical efficacy, albeit with longer treatment requirements and higher costs.
Ciclopirox 8% nail lacquer (Penlac): Applied daily with weekly removal of accumulated layers using alcohol; clinical studies show mycological cure rates around 30-36% over 48 weeks of use, making it most appropriate for early infections
Efinaconazole 10% solution (Jublia): Daily application for 48 weeks with superior nail penetration; clinical trials demonstrate mycological cure rates approaching 55% and complete cure (both clinical and laboratory clearance) around 15-18%
Tavaborole 5% solution (Kerydin): Once-daily application targeting fungal protein synthesis; mycological cure rates of 31-36% with complete cure rates of 6-9% in phase III studies
Amorolfine 5% lacquer (available outside the US): Weekly or twice-weekly application with nail preparation; international studies report mycological cure rates between 38-54% for mild to moderate cases
These prescription options are particularly valuable for patients who cannot tolerate oral antifungals due to liver disease, drug interactions, or personal preference. While cure rates may be lower than systemic therapy, the safety profile is excellent with minimal side effects limited to occasional local irritation or contact dermatitis.
How to Apply Antifungal Cream for Best Results
Success with topical antifungal treatments depends heavily on proper application technique and consistent daily execution over many months. This step-by-step approach maximizes medication penetration and coverage:
Evening application routine:
Wash thoroughly: Use soap and warm water, paying special attention to areas between toes
Dry completely: Use a clean towel and ensure no moisture remains, especially between digits
Trim and file: Cut nails straight across monthly; lightly file thickened areas weekly
Clean debris: Use a sanitized tool to gently remove loose material from under nail edges
Apply medication: Use enough product to cover the entire nail, cuticle area, and adjacent skin
Include surrounding area: Treat skin between affected toes where athlete’s foot commonly hides
Allow drying time: Wait 10-15 minutes before putting on socks or going to bed
Coverage essentials:
A thin, even layer works better than a thick application that may not absorb properly. Include the sides of the nail where infection often begins, the area under the free edge if accessible, and any skin showing signs of athlete’s foot. Many treatment failures result from inadequate coverage of these critical zones.
Consistency factors:
Missing applications or stopping treatment early is the primary cause of topical therapy failure. Set a daily reminder, keep medication visible in your bathroom, and track progress with photos taken monthly under consistent lighting. Remember that the nail may continue looking abnormal for months even when treatment is working effectively.

Oral Antifungal Medications: When Pills Make More Sense
Oral antifungals represent the most effective single treatment for moderate to severe toenail infections, offering significantly higher cure rates than topical therapy alone. These systemic medications are particularly appropriate when more than 50% of the nail plate is affected, multiple nails are involved, or the infection has reached the nail matrix near the cuticle.
Primary oral agents and their efficacy:
Terbinafine (Lamisil): The gold standard oral medication taken at 250mg daily for 12 weeks for toenails; large-scale studies like the LION trial demonstrate mycological cure rates around 76% compared to 38% for itraconazole
Itraconazole (Sporanox): Available as continuous dosing (200mg daily for 12 weeks) or pulse therapy (200mg twice daily for one week per month, repeated for 3-4 cycles); generally less effective than terbinafine but useful when drug interactions preclude terbinafine use
Fluconazole: Used off-label at doses of 150-300mg once weekly for 6-12 months; moderate effectiveness but longer treatment duration required
Advantages of systemic therapy:
The major benefit of oral antifungals lies in their ability to achieve therapeutic drug concentrations throughout the nail unit, including areas impossible to reach with topical applications. Terbinafine, in particular, concentrates in nail keratin and persists for months after the treatment course ends, providing continued antifungal activity as healthy nail replaces infected tissue.
Treatment duration is also more manageable—typically 6-12 weeks of active medication versus up to 48 weeks for topical therapies, though complete visible clearing still requires many months as new nail grows out.
Safety considerations and monitoring:
All oral antifungals require medical supervision due to potential side effects and drug interactions:
Liver function monitoring: Baseline and periodic blood tests to detect rare but serious hepatotoxicity
Drug interactions: Particularly important with itraconazole, which strongly inhibits liver enzymes that metabolize many medications
Side effects: Common issues include gastrointestinal upset, taste disturbances, headache, and skin rash; serious reactions like Stevens-Johnson syndrome are rare but possible
Combination strategies:
Many practitioners combine oral and topical therapy to maximize cure rates and reduce recurrence risk. A typical approach involves oral medication for the initial 12-week period followed by topical lacquer or solution for 6-12 months to target any residual fungal elements and prevent reinfection.
This multimodal approach is particularly valuable for patients with diabetes, peripheral vascular disease, or other factors that impair healing and increase recurrence risk.
Laser, Nail Removal, and Other Advanced Options
When conventional antifungal treatments fail or prove inappropriate, several advanced in-office procedures, including laser treatment, offer alternative approaches to managing persistent or severe toenail infections.
Laser therapy mechanisms and protocols:
Modern laser systems, typically using 1064nm Nd:YAG wavelengths, deliver focused energy that passes through the nail plate to heat and damage fungal cells within the nail bed.
Laser therapy for toenail fungus uses focused beams of light to destroy fungal cells and spores, but often requires multiple sessions for optimal results. The procedure is performed in-office without anesthesia, with each session lasting 10-30 minutes depending on the number of affected nails.
Treatment protocols usually involve 3-4 sessions spaced 4-6 weeks apart, allowing time for heat-damaged fungal elements to be eliminated by the body’s immune system. Some patients experience mild warmth or tingling during treatment, but significant discomfort is uncommon.
Evidence and effectiveness:
Laser therapy research shows mixed results, with reported mycological cure rates ranging from 30-60% across different studies. However, many trials have methodological limitations, small sample sizes, or industry funding that may influence results. Head-to-head comparisons with oral terbinafine are limited, and insurance coverage is often denied as the treatment is considered investigational or cosmetic.
The best laser outcomes typically occur when combined with aggressive mechanical debridement and topical antifungal therapy rather than as standalone treatment.
Mechanical debridement and nail thinning:
Professional nail debridement using specialized burrs and files can immediately reduce nail thickness and fungal load while dramatically improving topical medication penetration. Podiatrists perform this procedure periodically during treatment, removing as much infected nail material as safely possible.
For severely thickened or painful nails, this mechanical approach may provide more immediate symptom relief than medications alone while supporting the overall treatment plan.
Surgical options for severe cases:
Temporary nail removal (avulsion): Complete removal of the nail plate allows direct application of topical antifungals to the exposed nail bed; new nail growth is monitored and treated as it emerges
Permanent nail removal (matrixectomy): Destruction of the nail matrix prevents future nail growth; while this eliminates the fungal substrate, it results in permanent cosmetic changes and is rarely chosen except for chronically painful, repeatedly infected nails
Partial procedures: Selective removal of infected portions while preserving healthy nail sections may be appropriate for localized infections or ingrown nail complications
These surgical approaches are generally reserved for severe cases where medical therapy has failed, pain significantly impacts daily activities, or secondary bacterial infections have developed. Ultimately, these advanced treatments are designed to completely rid the nail of fungal infection and restore healthy nail growth.
For severe nail issues such as ingrown toenails, consider professional ingrown toenail treatment from a podiatrist to prevent complications and promote healing.
Daily Habits That Make Antifungal Creams Work Faster
Medication alone addresses only half of the toenail fungus equation—your daily habits control moisture, friction, and environmental fungal exposure that determine treatment success and long-term prevention. Implementing these evidence-based strategies can significantly accelerate healing and prevent recurrence.
Foot hygiene and foot care fundamentals:
Daily washing: Clean feet thoroughly with soap and water, paying special attention to areas between toes where athlete’s foot commonly persists
Complete drying: Use a separate, clean towel for feet to prevent spreading infection; ensure complete moisture removal, especially between digits
Antifungal powders: Apply daily to feet and inside shoes to reduce fungal load and absorb excess moisture
Evening inspection: Check feet daily for new lesions, increased redness, or signs of secondary bacterial infection
Foot care: Incorporate both home foot care practices and consider professional foot care treatments, such as visiting a podiatrist for persistent or severe cases
Footwear and sock management:
Moisture-wicking materials: Choose socks made from synthetic blends or merino wool rather than cotton, which retains moisture against the skin
Sock rotation: Change socks at least daily, more frequently if feet sweat heavily or after exercise
Shoe alternation: Rotate between at least two pairs of shoes, allowing 24 hours for each pair to dry completely between wears
Breathable footwear: Select shoes with mesh panels, leather uppers, or other breathable materials when possible; avoid plastic or synthetic materials that trap moisture
Environmental decontamination:
Shoe disinfection: Use antifungal sprays or UV sanitizers in shoes; remove and replace insoles regularly
Household surfaces: Clean shower floors, bath mats, and bedroom carpets with antifungal solutions; consider replacing heavily contaminated items
Laundry practices: Wash socks and towels in hot water with antifungal additives; dry on high heat when fabric allows
Public precautions: Wear flip flops in locker rooms, public showers, pool areas, and hotel rooms
Nail care optimization:
Regular trimming: Keep nails short and straight-cut to reduce trauma and debris accumulation
Professional debridement: Schedule periodic appointments for nail thinning and debris removal to improve medication penetration
Tool sanitation: Disinfect nail clippers, files, and other implements between uses; avoid sharing with family members. When visiting a nail salon, bring your own tools to reduce the risk of toenail fungus contamination.
Gentle handling: Avoid aggressive cuticle cutting, deep cleaning under nails, or other trauma that creates infection entry points
Systemic health optimization:
Blood sugar control: Maintain optimal glucose levels if diabetic to support immune function and healing
Circulation enhancement: Regular exercise, leg elevation, and compression stockings can improve blood flow to feet
Stress management: Chronic stress impairs immune function and may slow healing responses
Adequate sleep: Quality sleep supports immune system function and tissue repair processes
These daily practices should continue throughout treatment and for several months after visible clearing to prevent recurrence from environmental recontamination.
Learn more about why your feet may swell and effective treatments in our guide on Why Do My Feet Swell.

The Role of Nail Polish: Friend or Foe in Toenail Fungus Treatment?
Nail polish is a double-edged sword when it comes to treating toenail fungus. For many, the urge to cover up discolored or thickened nails with polish is strong, especially when symptoms of infection are visible and cause embarrassment. However, regular nail polish can actually make toenail fungus worse by trapping moisture against the nail and creating an environment where fungus thrives. This can allow the infection to spread further beneath the nail and into the surrounding skin, making treatment more difficult.
On the other hand, there are specialized antifungal nail polishes available that are formulated to help treat toenail fungus. Some of these products contain tea tree oil or other antifungal agents, which can help inhibit fungal growth while providing a cosmetic cover. These medicated polishes are designed to allow the nail to breathe and deliver active ingredients directly to the affected nail, supporting the overall treatment process.
It’s important to note that even antifungal nail polishes should be used as part of a comprehensive treatment plan, not as a standalone solution. Relying solely on polish can mask the symptoms of toenail fungus, making it harder to monitor progress and potentially delaying more effective treatments. If you’re considering using any type of nail polish during your treatment, consult a doctor or dermatologist first. They can recommend the best course of action for your specific infection and help you choose products that won’t interfere with your recovery.
In summary, while certain antifungal polishes may support your toenail fungus treatment, regular nail polish is generally best avoided until the infection is fully resolved. Always prioritize the health of your nail and follow your doctor’s advice for the most effective results.
Before-and-After Expectations: Timelines and What Results Really Look Like
Understanding realistic healing timelines prevents premature treatment abandonment and helps set appropriate expectations for both patients and family members. Toenail growth rates and infection clearance patterns follow predictable biological patterns, though individual variation is common.
Nail growth fundamentals:
Toenails grow approximately 1-1.5 millimeters per month, making complete replacement of a large toenail a 9-18 month process even under optimal conditions. Age, circulation, nutrition, and overall health significantly influence growth rates, with older adults often experiencing slower nail replacement.
The healing process requires physically growing out all infected nail material and replacing it with healthy tissue—a gradual biological process that cannot be accelerated beyond normal physiological limits.
Typical healing progression patterns:
Weeks 1-8: Usually no visible improvement; medication works at cellular level to inhibit fungal growth and reproduction
Weeks 8-16: First signs of clear nail growth may appear at the cuticle as a narrow band of normal-colored nail
Months 4-6: Clear zone progressively advances toward nail tip; some reduction in thickness and debris accumulation
Months 6-12: Continued improvement with clear nail replacing infected areas; smaller nails may achieve complete clearing
Months 9-18: Large toenails approach complete clearing; final assessment typically performed at 12-18 months
Normal healing variations:
Some patients notice alternating bands of clear and slightly discolored nail growth, reflecting periods when treatment was interrupted or fungal activity fluctuated. This pattern does not indicate treatment failure if the overall trend shows progressive improvement.
Nail thickness may improve gradually rather than returning immediately to normal, particularly in cases of long-standing infection or advanced age. Some permanent changes in nail contour or subtle color variation may persist even after successful fungal eradication.
Signs of treatment success:
Clear proximal growth: New nail emerging from the cuticle appears normal in color and thickness
Reduced debris: Less accumulation of powdery material under the nail
Improved texture: Nail becomes easier to trim and less brittle or crumbly
Laboratory confirmation: Negative fungal culture or microscopy when testing is performed
Warning signs requiring evaluation:
Increased pain, redness, or swelling: May indicate secondary bacterial infection
Rapid worsening: Sudden darkening or nail loss suggests complications
No improvement after 4-6 months: May indicate treatment resistance, incorrect diagnosis, or compliance issues
Spreading infection: New involvement of previously unaffected nails
Managing expectations realistically:
Even with optimal treatment, some nails may not achieve perfect cosmetic appearance, particularly in elderly patients or those with decades of infection history. The primary goals are fungal eradication, symptom relief, and prevention of progression rather than cosmetic perfection.
Patients should understand that visible improvement lags significantly behind microbiological cure—the fungus may be eliminated months before the nail appears completely normal.
Products We Hand Patients Every Week
In our clinical practice, we’ve identified specific evidence-based antifungal formulations that consistently deliver superior results when properly applied as par
t of comprehensive treatment plans. Rather than relying on trial-and-error with drugstore options, we recommend targeted products that address both nail penetration challenges and environmental fungal control. For those seeking over-the-counter options, Fungi-Nail is a notable product containing tolnaftate, an FDA-approved antifungal specifically formulated to treat toenail fungus.
Our nail-penetrating antifungal approach:
We typically combine a prescription-strength topical solution designed for nail penetration with a broad-spectrum cream for surrounding skin and athlete’s foot treatment. This dual approach addresses fungus within the nail structure while eliminating skin reservoirs that commonly cause reinfection.
For patients requiring nail softening prior to medication application, we often recommend medical-grade urea formulations that safely thin thickened nail plates, dramatically improving drug penetration without causing irritation when used as directed.
Shoe and environmental control:
Effective treatment extends beyond topical medications to include comprehensive environmental decontamination. We provide patients with professional-grade antifungal sprays and powders specifically formulated for footwear disinfection and daily moisture control.
These products target the fungal spores that survive in shoes, socks, and household surfaces, breaking the cycle of reinfection that undermines even effective nail treatments.
Professional-grade selection criteria:
The antifungal products we recommend meet stringent criteria for clinical effectiveness, safety, and patient compliance. Each formulation is selected based on published research, real-world patient outcomes in our practice, and compatibility with various treatment protocols.
You can explore our complete selection of clinically-proven options through our proven antifungal lineup, where we’ve curated the specific products we use daily in patient care.
Matching products to patient needs:
Rather than one-size-fits-all recommendations, we customize product selection based on infection severity, nail thickness, skin sensitivity, and lifestyle factors. Patients with diabetes receive different formulations than athletes, and elderly patients may need different application techniques than younger individuals.
The key principle is matching active ingredients (terbinafine, clotrimazole, ciclopirox, tolnaftate, or urea) with delivery systems optimized for individual patient anatomy and treatment goals. Even the strongest formulations require consistent daily application, proper nail preparation, and sufficient treatment duration to achieve lasting results.
Evolve Health: Our Comprehensive Toenail and Foot Treatment Approach
At Evolve Health, we recognize that successful toenail fungus treatment requires far more than simply prescribing antifungal medication. Our integrative approach addresses the complex interplay of factors that contribute to chronic nail infections while supporting your body’s natural healing processes.
Comprehensive diagnostic evaluation:
Every patient receives a thorough examination that goes beyond simply looking at discolored nails. We assess circulation, nerve function, biomechanical factors, and systemic health conditions that may predispose to infection or impair healing responses. Consulting a podiatrist is recommended for accurate diagnosis and treatment planning for toenail fungus, especially in complex or persistent cases.
Laboratory confirmation using microscopy and fungal culture helps distinguish true fungal infections from conditions like psoriasis, trauma-related changes, or nail dystrophy that can mimic fungal disease. This precision diagnosis prevents months of ineffective treatment targeting the wrong underlying cause.
Our detailed medical history review identifies medications, supplements, and health conditions that may influence treatment selection, particularly when considering oral antifungal therapy that requires careful monitoring and drug interaction screening.
Personalized treatment planning:
Rather than following rigid protocols, we develop individualized treatment strategies that consider your specific infection pattern, health status, lifestyle demands, and treatment preferences. This might involve topical monotherapy for early disease, combination oral and topical therapy for moderate infections, or multimodal approaches including laser therapy for resistant cases.
We integrate conventional antifungal medications with evidence-based supportive therapies, addressing factors like circulation enhancement, immune system optimization, and stress management that influence healing outcomes. Learn more about our comprehensive approach through our specialized treatment programs.
Ongoing support and monitoring:
Treatment success depends heavily on patient education, compliance support, and regular progress monitoring. We provide detailed instructions for medication application, nail care techniques, and environmental control measures that many patients have never learned properly.
Regular follow-up appointments every 2-3 months allow us to track nail regrowth patterns, adjust treatment protocols as needed, and identify early signs of recurrence or complications. We also address related foot health issues like chronic athlete’s foot, calluses, and biomechanical problems that often coexist with fungal nails.
Frequently Asked Questions (FAQs)
What are the most effective antifungal treatments for toenail fungus?
Oral antifungal medications such as terbinafine and itraconazole are often the most effective for moderate to severe toenail fungus. Topical treatments like medicated nail polishes and antifungal creams can be effective for mild cases or in combination with oral therapy. Consistent application and nail care are essential for success.
How long does it take to treat toenail fungus?
Treatment duration varies depending on severity but typically ranges from several months to over a year. Oral medications are usually taken for 6 to 12 weeks, but visible nail improvement requires time for new healthy nail growth, which can take 9 to 18 months.
Can home remedies like tea tree oil or vinegar cure toenail fungus?
While some natural remedies such as tea tree oil have antifungal properties and may provide mild symptom relief, they are not proven cures for established toenail fungus. They may be used as complementary therapies but should not replace medical treatment.
Is toenail fungus contagious?
Yes, toenail fungus can spread through direct contact with infected nails or contaminated surfaces such as communal showers, locker rooms, and swimming pools. Wearing shower shoes or flip-flops in communal areas helps reduce the risk.
Are there any risks with oral antifungal medications?
Oral antifungals can have side effects, including liver damage and drug interactions. Regular monitoring of liver function and consultation with a healthcare provider are important during treatment, especially for people with liver disease or those taking other medications.
When should I see a doctor for toenail fungus?
If symptoms worsen, do not improve after several months of treatment, or if you have underlying health conditions like diabetes, consult a podiatrist or dermatologist for accurate diagnosis and personalized treatment.
Conclusion
Toenail fungus is a common and often persistent condition that requires a comprehensive treatment approach combining antifungal medications, proper nail care, and lifestyle adjustments.
While oral antifungal drugs provide the highest cure rates, topical treatments and natural remedies can support healing, especially in mild cases. Patience and consistency are key, as visible improvement takes time due to slow nail growth.
Preventing reinfection through good foot hygiene, wearing shower shoes in communal areas, and maintaining dry, healthy feet is essential for long-term success. Consulting Evolve Health professionals ensures accurate diagnosis and the best course of treatment tailored to individual needs, helping you regain healthy, clear nails and avoid recurrence.