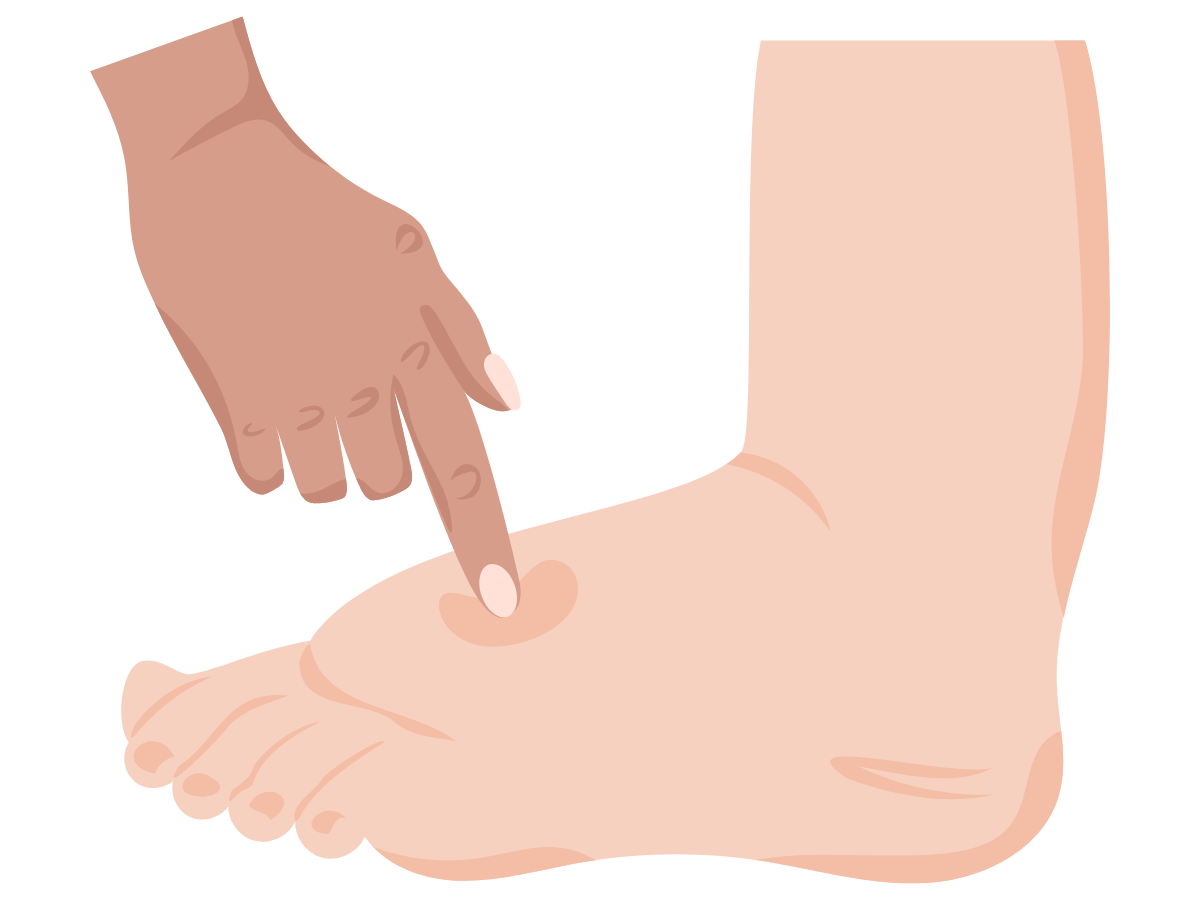
What Is Metatarsalgia?
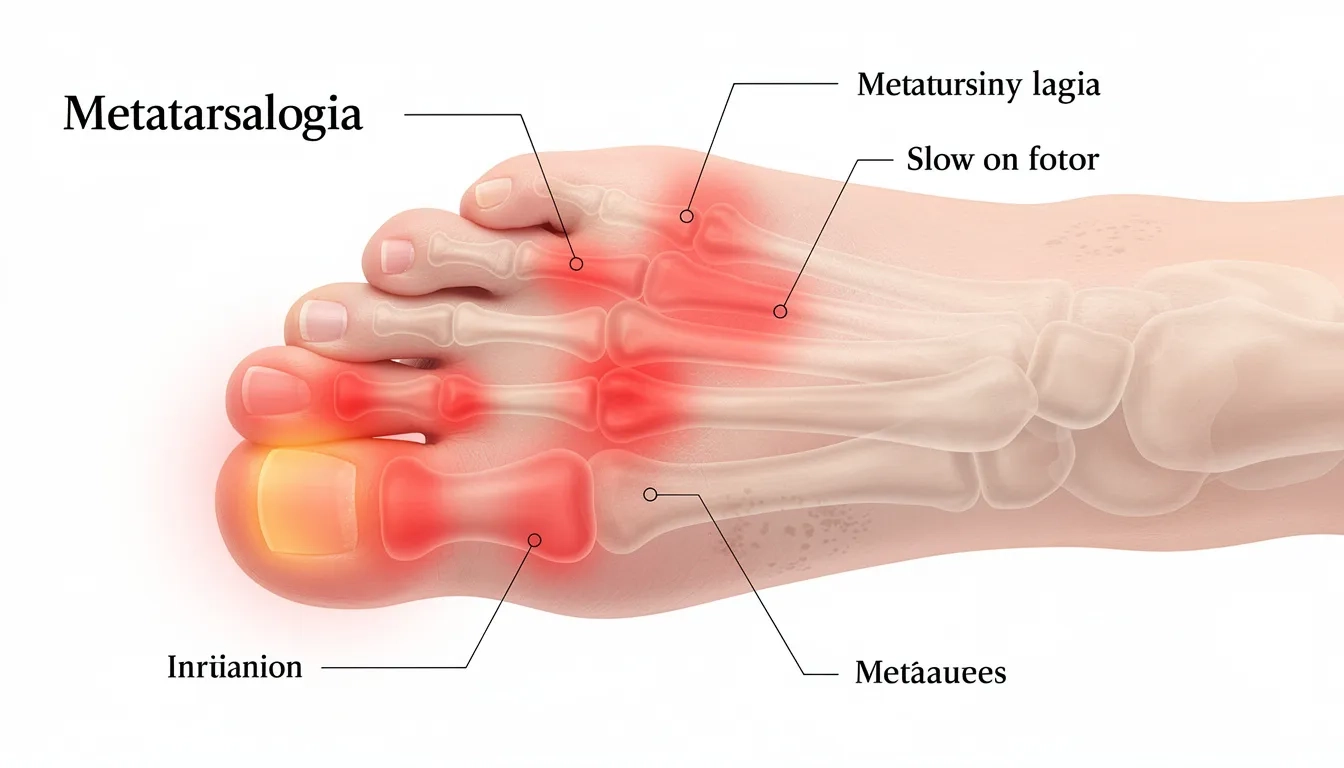
Metatarsalgia is a common term for pain in the ball of the foot, usually focused under the metatarsal head area (the long bones just behind the toes). It isn’t one single disease. Think of it as a pressure-related forefoot pain pattern that can be triggered by shoes, activity changes, foot structure, or inflammation. Repeated pressure or certain risk factors can cause someone to develop metatarsalgia.
Primary metatarsalgia is a type of metatarsalgia caused by structural issues in the foot, such as abnormalities in the metatarsal bones’ relationship with other parts of the foot.
Pain can be mild and annoying, or severe enough to change the way you walk. When the foot changes how it loads, it can also set off secondary discomfort in the arch, heel, ankles, knees, hips, or back over time.
Next, we’ll look at metatarsalgia causes in more detail.
Metatarsalgia Symptoms That Matter
A lot of people describe metatarsalgia pain in similar ways:
A burning pain or aching under the ball of the foot
A sharp, shooting pain when you push off the toes
Pain that gets worse after long periods of standing or walking
Tenderness under the second toe or big toe area
Feeling like there’s a rock in your shoe
If you’re noticing tingling or itching sensations in the feet at night, that may be a separate issue that can overlap with foot irritation. In that case, it’s worth reading about Itchy Feet at Night to understand possible causes and when to seek care.

What Causes Ball-of-Foot Pain?
Metatarsalgia usually comes from extra pressure placed repeatedly on the metatarsal bones and soft tissues. Common triggers include:
Shoes that concentrate pressure
High heels, narrow toe boxes, thin soles, or shoes without enough support can increase pressure under the ball of the foot. Shoes with flexible soles may provide less support and increase stress on the soft tissues of the foot, contributing to metatarsalgia. Even “good” athletic shoes can become a problem if the cushioning is worn out or the fit is too tight.
High impact sports and sudden training changes
Running, jumping, and fast direction changes can overload the forefoot, especially if you ramp up mileage quickly or train on a hard surface.
Foot structure and mechanics
High arches can shift load forward. Flat feet can change weight bearing patterns. A longer second metatarsal, bunions, and toe alignment issues can also force more pressure into one painful area.
Tight calf muscles and Achilles tendon tension
When the calf and Achilles are tight, the heel may lift earlier during gait, pushing more pressure toward the ball of your foot.
Inflammatory conditions and other foot problems
Rheumatoid arthritis or other inflammatory conditions may make forefoot pain more likely. In some cases, metatarsalgia-like symptoms are actually another condition such as Morton’s neuroma, plantar plate irritation, or a stress fracture.
Diagnosis and Assessment: How Podiatrists Identify Metatarsalgia
When you visit a health care professional for metatarsalgia pain, the diagnostic process is thorough and tailored to uncover the root cause of your discomfort. A podiatrist will start by reviewing your medical history, asking about your symptoms, daily activities, and any previous foot problems. This helps them understand how long you’ve been experiencing pain and what might be making the problem worse.
Next, a physical examination focuses on the metatarsal area, checking for signs of inflammation like redness, swelling, or tenderness. The podiatrist will gently press on different parts of your foot and toes to pinpoint the most affected area. They’ll also assess your range of motion and look for issues such as a tight Achilles tendon or high arches, which can increase pressure on the ball of the foot.
A key part of the assessment is watching how you walk. Gait analysis helps identify abnormal walking patterns that may be contributing to metatarsalgia pain. The podiatrist will also examine your shoes for wear patterns or lack of support, as improper footwear can often lead to or worsen foot pain.
If there’s concern about a possible stress fracture or other underlying foot problems, an x-ray may be recommended. This imaging helps rule out more serious conditions and ensures the right treatment plan is chosen. By combining these steps, your podiatrist can accurately diagnose metatarsalgia and develop a personalized approach to relieve your pain and restore healthy foot function.

Metatarsalgia vs. Other Forefoot Problems
Ball-of-foot pain isn’t always metatarsalgia, and this matters because treatment changes.
Metatarsalgia typically feels like a pressure bruise or burning ache under the metatarsal area that worsens with walking. Left untreated, metatarsalgia can lead to a further increase in pain and may develop into a chronic condition. If left untreated, metatarsalgia might also lead to pain in other parts of the same foot or in the other foot. Limping because of the foot pain of metatarsalgia can cause pain in other parts of the body, such as the low back or hip.
A stress fracture often feels more focal and sharp, and may worsen with impact even when you try to “push through.”
Morton’s neuroma is more likely when pain radiates into the toes, with tingling, numbness, or a “zapping” sensation between toes.
If your symptoms persist or intensify, it’s smart to get assessed rather than guessing.
How to Relieve Metatarsalgia at Home
Most mild to moderate cases improve when you reduce pressure and let irritated tissues settle. Home treatment is often effective for addressing mild metatarsalgia and can include simple self-care measures. The goal is pain reduction now, then improved function long-term.
Conservative treatment for metatarsalgia includes RICE (Rest, Ice, Compression, Elevation) and NSAIDs to help reduce pain and inflammation.
Activity modification, such as pacing yourself and taking regular breaks, can also help manage metatarsalgia symptoms.
Step 1: Reduce pressure for a short window
If the painful area is flaring, take a brief break from the activity that triggered it. That might mean swapping high impact sports for low impact options like cycling or swimming for a week or two.
Step 2: Ice and simple pain relievers when appropriate
An ice pack can reduce inflammation and calm the painful area. Over the counter pain relievers may help some people, but they don’t address the underlying pressure problem.
Step 3: Fix the shoe problem first
This is where many people get stuck. If the shoe continues to increase pressure, symptoms keep returning.
If you also deal with heel or arch issues, your footwear choice matters even more. A helpful starting point is our guide to Shoes for plantar fasciitis because many of the same features that reduce heel strain also reduce forefoot overload, like supportive cushioning and smart structure.
Step 4: Add padding the right way
Metatarsal pads can relieve pressure, but placement matters. A pad usually works best when it sits slightly behind the painful metatarsal head to help spread weight bearing forces, not directly on top of the most painful spot. If it feels worse, it may be positioned incorrectly or the shoe may not have enough volume.
Step 5: Address tight calves and mechanics
Gentle calf stretching and improving ankle mobility can reduce how much pressure shifts forward during gait. If tight calf muscles or a tight Achilles tendon are driving early heel lift, forefoot pain often keeps returning until that pattern improves.
When to Seek Custom Orthotics
Over the counter options help many people, especially when the main issue is footwear and mild pressure overload. But custom orthotics can be a stronger choice when the pain is recurring, when foot shape creates uneven loading, or when you need a precise pressure redistribution strategy.
Consider a podiatry evaluation for orthotics if:
Your pain keeps returning after you change shoes and reduce activity.
The pain is consistently in the same metatarsal head area.
You have high arches, flat feet, or toe deformities that clearly change loading.
You walk or stand for work and cannot avoid long periods on hard floors.
When a Metatarsalgia Podiatrist in Houston Can Help
If you’re searching for a metatarsalgia podiatrist Houston patients rely on, a focused foot evaluation can speed up recovery and prevent chronic pain. A health care professional will typically review your medical history, examine foot structure, test tender points, and evaluate shoes and gait.
Imaging such as an x ray may be recommended if a stress fracture, arthritis, or other foot problems are suspected.
During relief planning, it can help to connect with forefoot specialists who understand how daily load patterns, commuting, and footwear choices combine to trigger recurring forefoot pain. For local care options, you can explore Evolve Health clinics in the area, including Houston forefoot specialists and Houston foot specialists depending on what’s closest to you.
If insurance is part of your decision, you may also want to read Find Podiatrist that accepts Aetna so you know what to check before booking and how to avoid surprises.
What Treatment Can Look Like in a Clinic
Metatarsalgia treatment options vary based on what’s causing the pressure overload. Individualized treatment plans are essential for effective pain relief and recovery, with surgery considered a last resort. The goal of treatment and rehabilitation for metatarsalgia is to restore normal range of motion, strength, and function of the foot. Depending on your case, a podiatrist may recommend:
Targeted padding and metatarsal pads with correct placement
Orthotics or arch supports to redistribute pressure
Shoe changes with a wide toe box and better cushioning
Physical therapy style exercises to improve mechanics and reduce recurrence; physical therapy for metatarsalgia may involve gentle stretches and strengthening exercises
Treatment for related conditions if the pain source isn’t true metatarsalgia
Corticosteroid injections can help reduce inflammation and pain in severe cases of metatarsalgia, and if home remedies aren’t providing enough relief, a cortisone injection may be recommended.
Surgery is usually reserved for severe cases that don’t respond to conservative care or when structural issues require correction. Surgery may be considered if metatarsalgia symptoms interfere with normal activities and have not responded to other treatments.
Fat Pad and Metatarsalgia: Understanding the Connection
The fat pad beneath the ball of the foot acts as a natural cushion, absorbing shock and protecting the metatarsal bones from extra pressure during walking and standing. Over time, however, this soft tissue can thin out—a condition known as fat pad atrophy—which leaves the metatarsal area more vulnerable to pain and injury.
Several factors can contribute to fat pad loss, including aging, frequent wearing of high heels, and chronic pain that alters the way you walk. When the fat pad is no longer able to provide enough support, more pressure is placed directly on the metatarsal bones, often resulting in metatarsalgia pain.
To help reduce pain and protect the fat pad, it’s important to choose shoes with a wide toe box and a soft, cushioned insole. Wearing shoes that fit well and offer enough support can relieve pressure on the ball of the foot and prevent further damage. For those carrying extra weight, losing weight can also decrease the load on the metatarsal area and improve overall foot comfort.
Metatarsal pads and arch supports are useful tools for redistributing pressure away from the most painful spots. These devices can be especially helpful when combined with other treatment options recommended by a health care professional. If you’re experiencing chronic pain or suspect fat pad atrophy, a podiatrist can guide you toward the best treatment to reduce pain, relieve pressure, and restore healthy function to your foot.
Preventing Metatarsalgia from Coming Back
The most consistent prevention strategy is simple: keep pressure balanced.
Replace worn athletic shoes before they lose cushioning and support.
Avoid high heeled shoes when you know you’ll be on your feet for long periods.
Build training volume gradually instead of jumping suddenly into higher mileage or harder surfaces.
Stay consistent with calf mobility if tight calf muscles are part of your pattern.
Evolve Health Approach
At Evolve Health, we focus on the root driver of forefoot pain: pressure, mechanics, and structure. That means we don’t just tell patients to “rest and ice” and hope it disappears. We look at why the metatarsal area is overloaded, how your shoes and daily routine contribute, and whether padding solutions or custom orthotics are needed to improve function and keep pain from returning.
FAQs
How long does metatarsalgia take to heal?
Mild cases often improve within a few weeks when pressure is reduced and shoes are corrected. Persistent cases can last longer, especially if the underlying pressure pattern isn’t changed.
Do metatarsal pads really work?
They can, especially when placed correctly and paired with the right shoe. If a pad increases pain, it may be too far forward, too thick, or your shoe may not have enough room.
Can metatarsalgia be a stress fracture?
Yes, forefoot pain can sometimes be a stress fracture, especially if pain is sharp, focal, and worsens with impact. An exam and possibly imaging help clarify.
What shoes are best for ball-of-foot pain?
Look for a wide toe box, good cushioning, and a supportive structure that doesn’t force the forefoot to absorb all the load. If you also have heel or arch pain, this Shoes for plantar fasciitis guide is a useful reference.
When should I see a podiatrist?
If pain lasts more than two to three weeks, keeps returning, or becomes severe pain that changes how you walk, it’s time to see a specialist.