What is Plantar Fasciitis?
The plantar fascia is a thick, fibrous band of tissue that runs along the bottom of your foot, connecting the heel bone to the toes. It works like a bowstring, supporting the arch of your foot and absorbing the stress of daily movement.
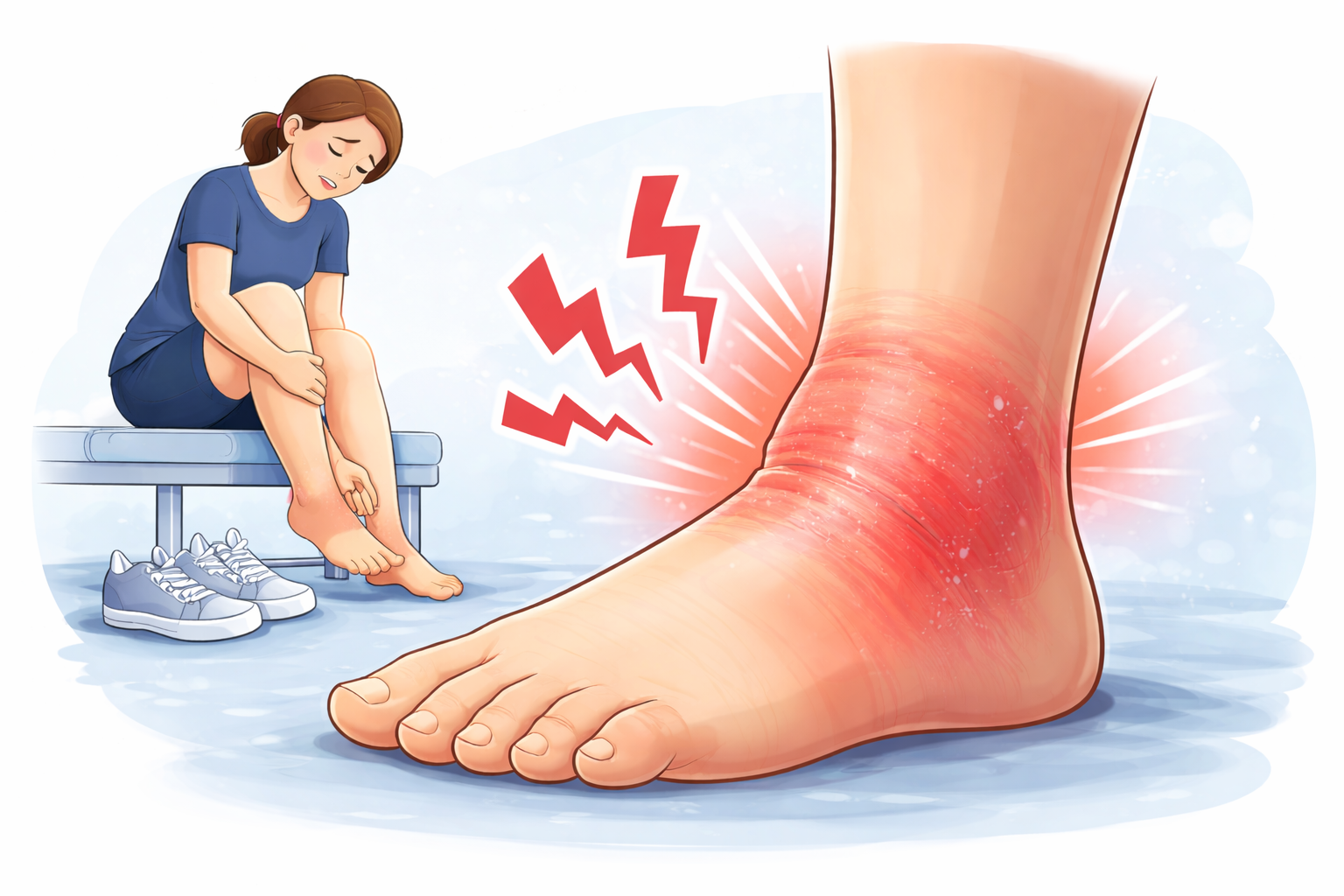
The heels are the area most commonly affected by plantar fasciitis, as this condition often causes pain and discomfort in that region.
When this tough band is overstretched or subjected to too much stress, tiny tears develop in the tissue. These small tears can cause inflammation, leading to pain and stiffness.
Most patients describe the discomfort as a stabbing pain near the heel, especially during the first steps in the morning or after long periods of sitting. The pain can also feel like pressing down on a bruise, adding to the discomfort.
Symptoms of Plantar Fasciitis Pain
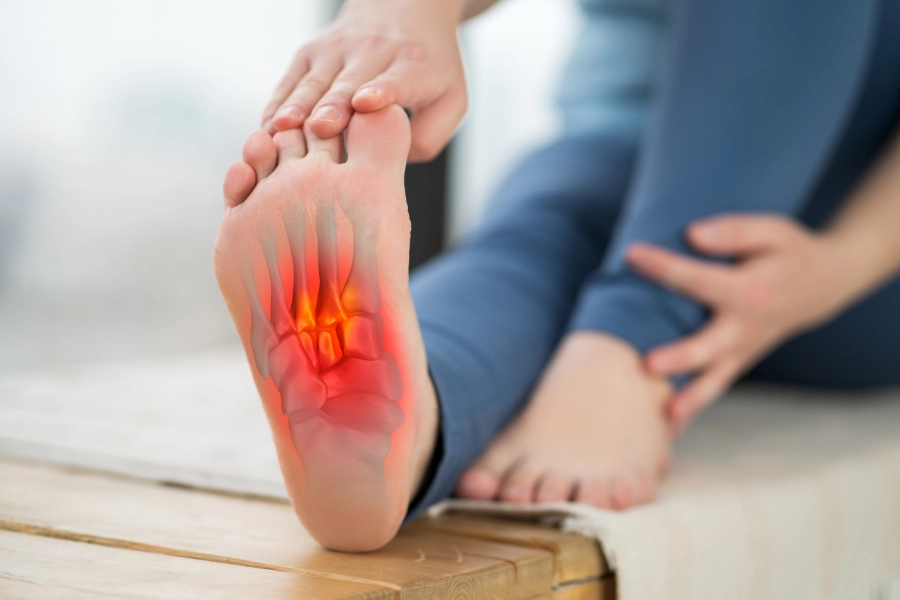
The most common plantar fasciitis symptoms include:
Heel pain that is worst when you first get out of bed.
A stabbing or aching sensation in the arch or heel.
Pain that worsens after standing on hard surfaces or walking long distances.
Stiffness in the calf muscles or tightness in the Achilles tendon.
Swelling or tenderness at the bottom of the heel.
Plantar fasciitis pain is typically sharp and most noticeable with your first steps in the morning or after periods of rest, and it can be distinguished from other foot conditions by its location and timing.
Symptoms can vary in intensity. Some people feel pain only after exercise, while others develop chronic heel pain that interferes with daily life. Most people develop plantar fasciitis around age 40, making it a common issue for middle-aged individuals.
Causes and Risk Factors
Understanding what causes plantar fasciitis is essential, as it often develops gradually and is typically linked to repetitive strain or poor foot mechanics. Common causes include:
Standing, walking, or running on hard surfaces for long periods.
Wearing shoes that lack extra arch support or cushioning.
Flat feet or very high arches alter pressure distribution.
Tight lower leg muscles or Achilles tendons that strain the fascia.
Rapid weight gain or obesity, as well as other health conditions such as flat feet, which put more stress on the plantar fascia and contribute to plantar fasciitis.
Sports activities with repetitive jumping or impact, such as basketball or running.
How is Plantar Fasciitis Diagnosed?
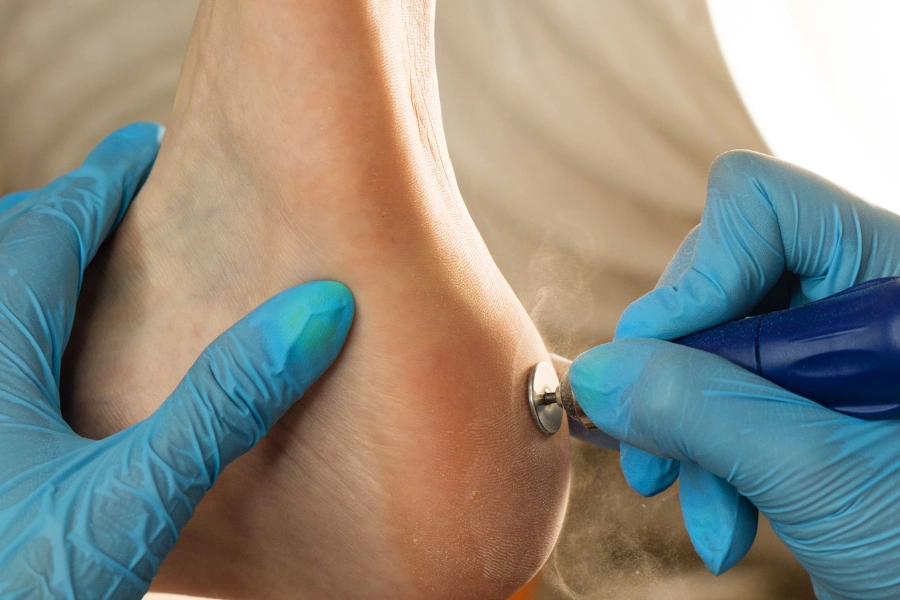
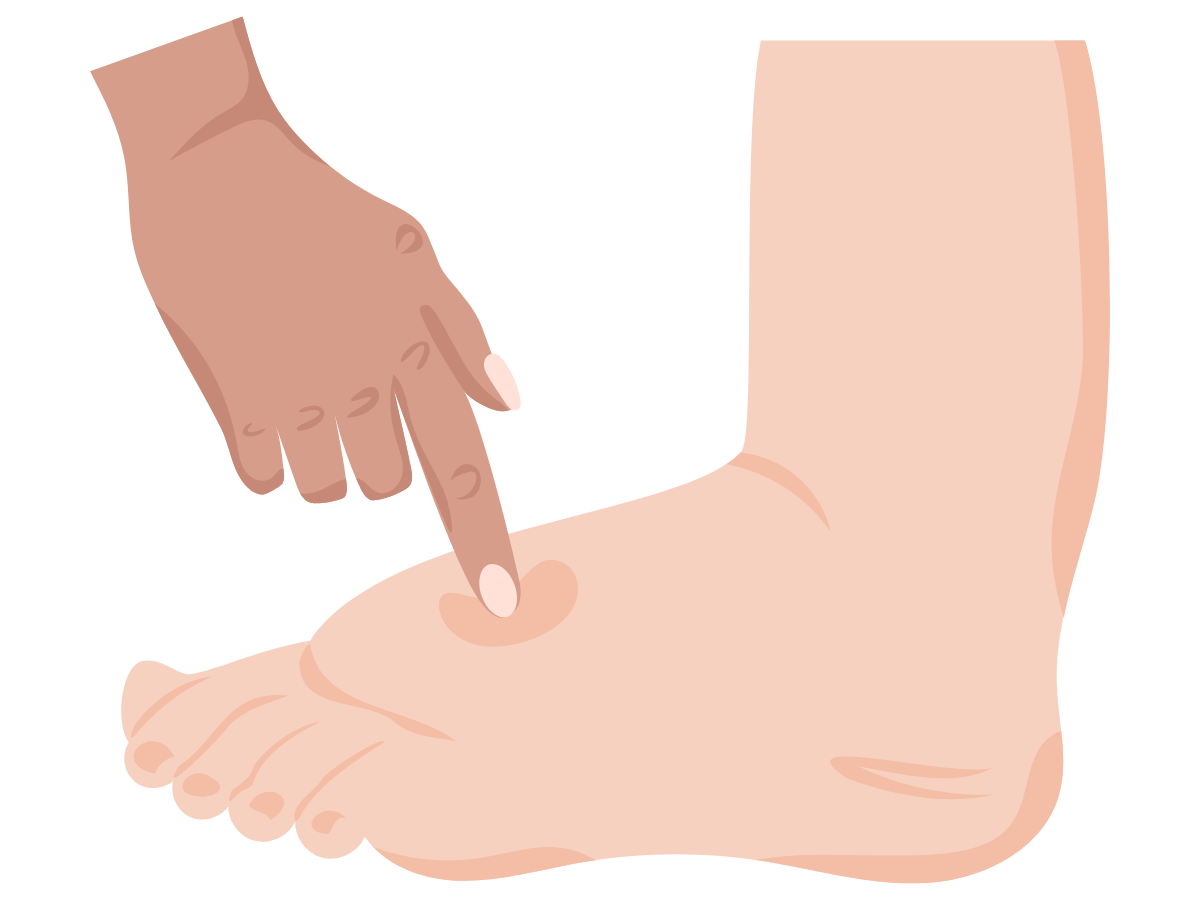
Diagnosis begins with a physical exam. To diagnose plantar fasciitis, your doctor will press on the bottom of your foot to identify tender spots and ask questions about your medical history, activity level, and daily routine.
In most cases, imaging is not required. However, if pain is severe or does not improve, your doctor may order X-rays, an MRI, or an ultrasound to rule out stress fractures, heel spurs, or other conditions affecting the foot.
Accurate diagnosis is important because foot pain can also be caused by Achilles tendinitis, tarsal tunnel syndrome, or even stress fractures.
What to Expect After Diagnosis
After your doctor has diagnosed you with plantar fasciitis, you’ll begin a treatment plan designed to reduce pain and promote healing of the plantar fascia.
Most people start with nonsurgical treatments, which may include resting your foot, applying ice to decrease inflammation, and using over-the-counter medications to manage pain. Your doctor might recommend wearing supportive shoes for plantar fasciitis or adding orthotic insoles to provide extra cushioning and support for your arch.
Physical therapy is often a key part of treating plantar fasciitis, as targeted exercises can stretch and strengthen the plantar fascia and surrounding muscles. Night splints may also be suggested to keep your foot in a stretched position while you sleep, helping to reduce morning pain and stiffness.
A night splint keeps the foot at a 90-degree angle to provide a constant stretch while you sleep, which can be particularly effective in managing symptoms. Some patients also benefit from using massage rollers or ice packs for daily relief at home.
For more detailed guidance on managing plantar fasciitis, including effective home treatments and prevention tips, you can visit our treatment for plantar fasciitis service for expert advice and resources.
It’s important to follow your doctor’s instructions and attend any recommended follow-up appointments to track your progress. With consistent care and the right combination of treatments, most people experience significant improvement and can return to their usual activities without ongoing pain.
Does Plantar Fasciitis Heal On Its Own?

This is the question almost every patient asks: Does plantar fasciitis heal naturally? The answer is yes — but it often takes time, and recovery can be frustrating without supportive care.
In some cases, symptoms improve within a few months with rest, proper footwear, and stretching.
For others, pain can linger for 6–12 months or even longer if untreated.
Without treatment, plantar fasciitis can become chronic, leading to altered walking patterns that create problems in the knees, hips, or back.
So while plantar fasciitis may go away on its own eventually, active treatment speeds recovery and lowers the risk of long-term complications. Recovery from plantar fasciitis cure can take 3 to 12 months with non-surgical treatments, depending on the severity of the condition and adherence to treatment plans.
At-Home Treatments to Relieve Pain

Conservative care is the first step in managing plantar fasciitis. At-home measures are often effective ways to treat plantar fasciitis and manage symptoms. By easing stress on the fascia and encouraging healing, simple at-home measures can make a noticeable difference in symptoms.
Stretching
Gentle stretching of the calf muscles and plantar fascia reduces tightness and relieves pressure on the heel. Daily stretches, especially in the morning and after long periods of sitting, help improve flexibility and promote healing.
Icing
Applying cold therapy is another effective way to reduce inflammation. A common method is rolling a frozen bottle under the affected foot for 10 to 15 minutes, which not only cools the painful area but also massages the tissue. Additionally, icing the heel for 10 to 20 minutes can further help reduce inflammation and provide relief.
Supportive Shoes
Wearing sturdy, cushioned shoes is essential. Proper footwear supports the arch and reduces impact on the heel, while walking barefoot or using flimsy sandals can make symptoms worse. Choosing shoes with extra arch support can prevent flare-ups and reduce daily discomfort. You can also add inserts or custom orthotics to your shoes to provide extra arch support, customize comfort, and improve overall foot health.
Over-the-Counter Medications
Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, can ease both pain and swelling when used occasionally. These medications are not a long-term cure, but they provide short-term relief that allows patients to stay mobile and continue stretching exercises.
Most people notice improvement within a few weeks of consistent care. However, if pain persists beyond two weeks, it is best to seek medical advice from a podiatrist for further evaluation and treatment.
How Long Does Plantar Fasciitis Last?
A common concern is how long plantar fasciitis lasts. Recovery time varies:
With consistent treatment, symptoms may resolve in a few months.
Some patients need 6–12 months to fully heal.
Rarely, plantar fasciitis can last more than a year if ignored.
Factors such as age, activity level, foot structure, and weight all influence recovery speed. Following a doctor’s treatment plan shortens healing time and prevents flare-ups.
Prevention Tips
Preventing plantar fasciitis is often easier than curing it. Helpful strategies include:
Wearing supportive shoes and replacing sneakers every 6–9 months.
Stretching the calves and Achilles tendon before and after exercise.
Avoiding long periods of standing on hard surfaces without breaks.
Maintaining a healthy weight reduces pressure on the fascia.
Alternating high-impact workouts with low-impact activities such as swimming or cycling.
Living With Plantar Fasciitis
Living with this condition requires patience and lifestyle adjustments. Many patients find they need to change footwear, pace themselves during activities, and build stretching routines into their day. Supportive aids such as custom orthotics or cushioned insoles can make a big difference in staying active without constant pain.
At Evolve Health, our podiatrists help patients create tailored plans that blend home care, medical treatment, and prevention strategies.
When to See a Doctor

Book an appointment if:
Pain lasts longer than two weeks despite at-home care.
You notice swelling, redness, or warmth in the affected foot.
Pain interferes with work, sleep, or exercise.
You develop chronic pain in both feet or additional problems, such as knee or back pain.
Book an Appointment now to meet with a podiatrist and explore treatment options.
Conclusion
So, can plantar fasciitis go away on its own? Sometimes, but the better question is, how quickly do you want it to heal? For many, active treatment is the difference between months of discomfort and a faster, safer recovery.
With the right mix of at-home treatments, professional care, and prevention strategies, plantar fasciitis can be managed and often fully resolved.
FAQs
Does plantar fasciitis heal without treatment?
Plantar fasciitis can sometimes heal on its own, but this process often takes several months to a year. Without treatment, the pain may persist longer and increase the risk of complications such as chronic heel pain or altered walking patterns.
What is the best treatment for plantar fasciitis?
The most effective treatment usually combines regular stretching exercises, wearing supportive shoes, and using orthotic inserts to provide extra arch support. For persistent cases, additional treatments like corticosteroid injections, shockwave therapy, or surgery may be recommended by a healthcare professional.
How long does plantar fasciitis last?
With proper care and treatment, plantar fasciitis symptoms often improve within a few months. However, if left untreated, the condition can persist for over a year and lead to chronic pain and mobility issues.
Is plantar fasciitis curable?
Yes, plantar fasciitis cure generally depends on conservative treatments such as rest, stretching, and proper footwear. Surgery is rarely necessary but may be considered for severe or long-lasting cases that do not respond to other treatments.
When should I see a doctor for heel pain?
You should see a doctor if your heel pain lasts longer than two weeks, worsens, or interferes with your daily activities such as walking. Early evaluation by a podiatrist helps ensure accurate diagnosis and effective treatment to prevent complications.