Understanding Psoriasis on Feet
Types of Foot Psoriasis
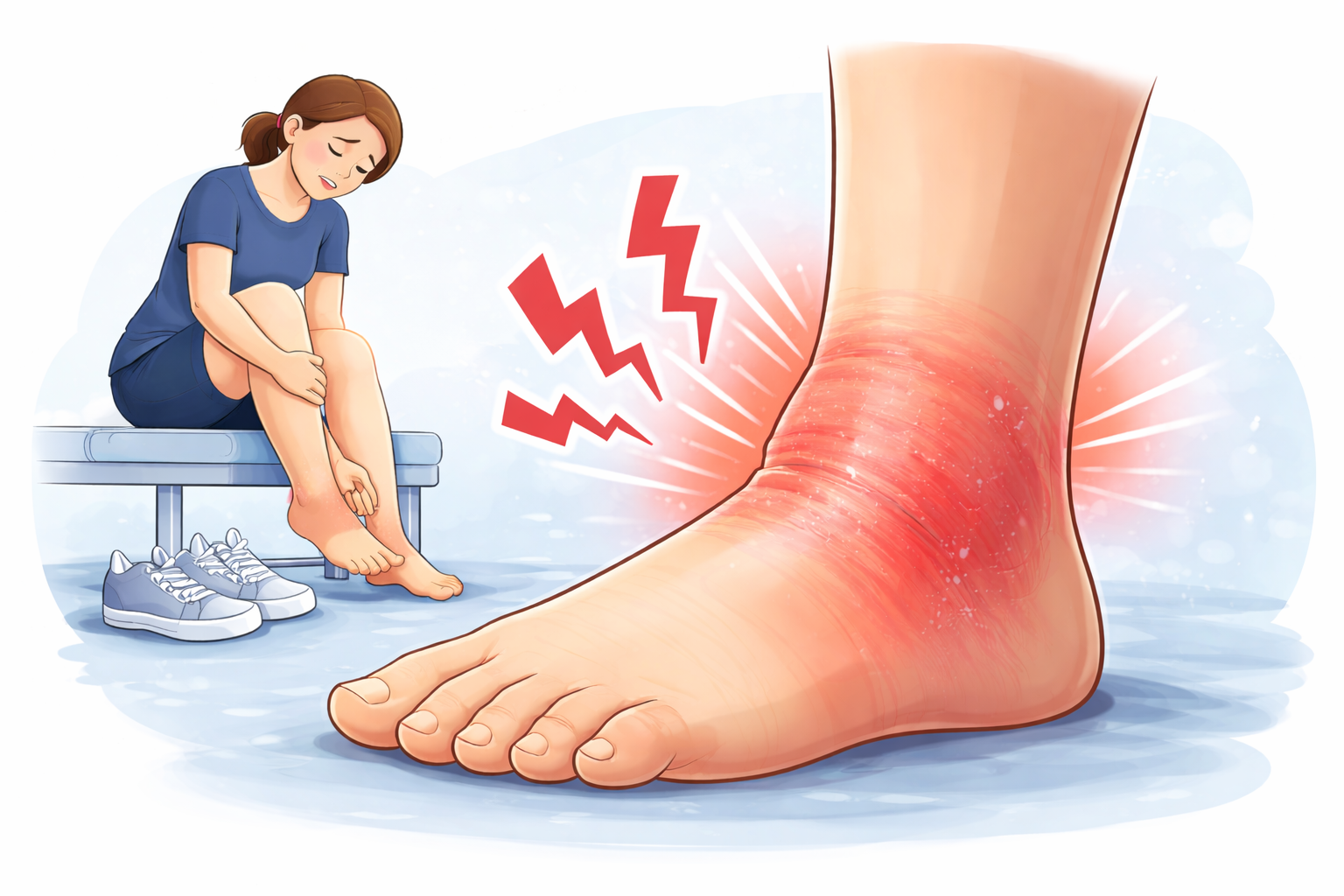
Psoriasis on feet can present in various forms, with plaque psoriasis being the most prevalent, affecting about 90% of individuals with the condition. Plaque psoriasis typically causes dry, raised patches known as plaques, which can lead to significant discomfort on the feet. Another variant, palmoplantar pustular psoriasis (PPP), results in small, pus-filled blisters on the soles of the feet, often leading to painful cracks. Nail psoriasis is also common, causing thickened, discolored nails, which can add another layer of discomfort.
Symptoms of Foot Psoriasis
Foot psoriasis symptoms can be particularly severe. The primary indicator is a dry, scaly rash with well-defined edges, often covered with white or silver skin. These plaques can be itchy and sore, and in severe cases, they may crack open and bleed. Palmoplantar pustular psoriasis is characterized by pus-filled blisters that can lead to painful fissures, which are symptoms that are not typically seen with conditions like eczema or athlete’s foot. Recognizing these symptoms early can facilitate more effective management and minimize flare-ups.
Causes and Triggers
While the exact cause of psoriasis remains under research, it is generally considered an inherited inflammatory disease triggered by several factors. Skin injuries, such as cuts or burns, are known to worsen psoriasis on feet. Other triggers include certain medications, infections, emotional stress, and lifestyle factors like smoking and heavy alcohol consumption. Identifying and avoiding these triggers is crucial for effective management.
Diagnosis and Differentiation
Diagnostic Methods
Accurate diagnosis of foot psoriasis is essential for effective treatment. Psoriasis is frequently confused with other skin conditions like eczema and athlete’s foot. Typically, diagnosis involves a physical examination, where a dermatologist looks for silvery scales on the skin, and may include a biopsy to confirm the presence of psoriasis and rule out other conditions. The process also considers family history, as psoriasis often has a genetic component.
Psoriasis vs. Eczema vs. Athlete’s Foot
Psoriasis plaques are generally covered with a thick, white or silver scale, which distinguishes them from eczema or athlete’s foot. Athlete’s foot usually presents as a reddish, scaly rash between the toes, while eczema typically affects the front of the ankle and does not usually involve the nails. Understanding these distinctions is vital for ensuring appropriate treatment, as severe psoriasis can mimic other conditions, necessitating professional evaluation.
Treatment Options for Foot Psoriasis
While psoriasis is a chronic condition without a cure, several treatment options can help alleviate symptoms and manage flare-ups. These include:
Topical Treatments: Often the first line of defense, topical treatments include over-the-counter emollients, mild steroid creams, and keratolytic agents like salicylic acid. These treatments can reduce inflammation and soothe the skin.
Light Therapy (Phototherapy): Exposing the skin to ultraviolet light in a controlled setting can significantly benefit psoriasis. UVB phototherapy and psoralen-UVA (PUVA) therapy are common methods used to reduce symptoms.
Systemic Treatments: For severe cases of foot psoriasis, systemic treatments like biologics (e.g., adalimumab) may be prescribed. These medications target specific parts of the immune system to reduce inflammation and improve symptoms.
Lifestyle Changes and Self-Care Practices
Moisturizing and Skincare
Regular moisturizing is critical for managing psoriasis on feet. Using thick creams, particularly those containing urea or salicylic acid, can help alleviate dryness and prevent cracking. Incorporating oatmeal baths into your routine and opting for comfortable footwear can also reduce symptoms.
Diet and Exercise
Maintaining a healthy weight through a balanced diet can help mitigate flare-ups. Regular exercise—particularly low-impact activities like swimming or walking—can enhance overall health and improve medication efficacy.
Avoiding Triggers
Identifying and steering clear of known triggers, such as alcohol and smoking, can significantly improve the management of foot psoriasis. Stress management techniques, including meditation and yoga, can also be beneficial in reducing flare-ups
When to See a Specialist
Severe Symptoms
It is crucial to consult a specialist if symptoms of psoriasis on feet worsen or do not respond to initial treatments. Severe psoriasis can lead to painful cracking, and a healthcare professional can provide targeted interventions to manage the condition effectively.
Persistent Issues
If symptoms remain unresolved with home treatments or over-the-counter options, it’s time to seek a dermatologist’s expertise. Chronic discomfort and mobility difficulties due to foot psoriasis warrant professional assessment and intervention.
Managing Psoriatic Arthritis
For individuals experiencing psoriatic arthritis (PsA) in the feet, characterized by inflammation and joint pain, consulting a specialist is vital. Effective management strategies include rest, supportive footwear, and potentially physiotherapy or surgery for long-standing issues.
Nail Psoriasis
Nail psoriasis can also affect toenails, causing discomfort and difficulty with mobility. Symptoms may include pitting, thickening, and discoloration of nails. Treatment for nail psoriasis typically involves topical medications or, in severe cases, systemic therapies.

Common Questions About psoriasis
What are the most common symptoms of foot psoriasis?
The most common symptoms of foot psoriasis include a dry, scaly rash with well-defined edges, itchy and sore plaques, and pus-filled blisters, and in severe cases, the plaques can crack and bleed.
How can I differentiate foot psoriasis from athlete's foot or eczema?
You can differentiate foot psoriasis from athlete’s foot or eczema by looking for thick, white or silver scales on the plaques for psoriasis, a scaly, reddish rash between the toes for athlete’s foot, and eczema affecting the front of the ankle without involving the nails.
What are the best treatment options for foot psoriasis?
The best treatment options for foot psoriasis include topical treatments, light therapy, and systemic treatments such as biologics and retinoids. Consider consulting a dermatologist to determine the most suitable option for your condition.
When should I see a specialist for foot psoriasis?
You should see a specialist for foot psoriasis if you have severe symptoms or if your symptoms do not improve with home treatments and over-the-counter medications. Seeking specialized care can help address the condition effectively.
How can I manage psoriatic arthritis in my feet?
To manage psoriatic arthritis in your feet, focus on resting inflamed joints, using supportive footwear, and considering various treatments such as NSAIDs, corticosteroid shots, DMARDs, and biologics. Physiotherapy and surgery may also be necessary for severe cases.