What Are Night Splints and How Do They Work?
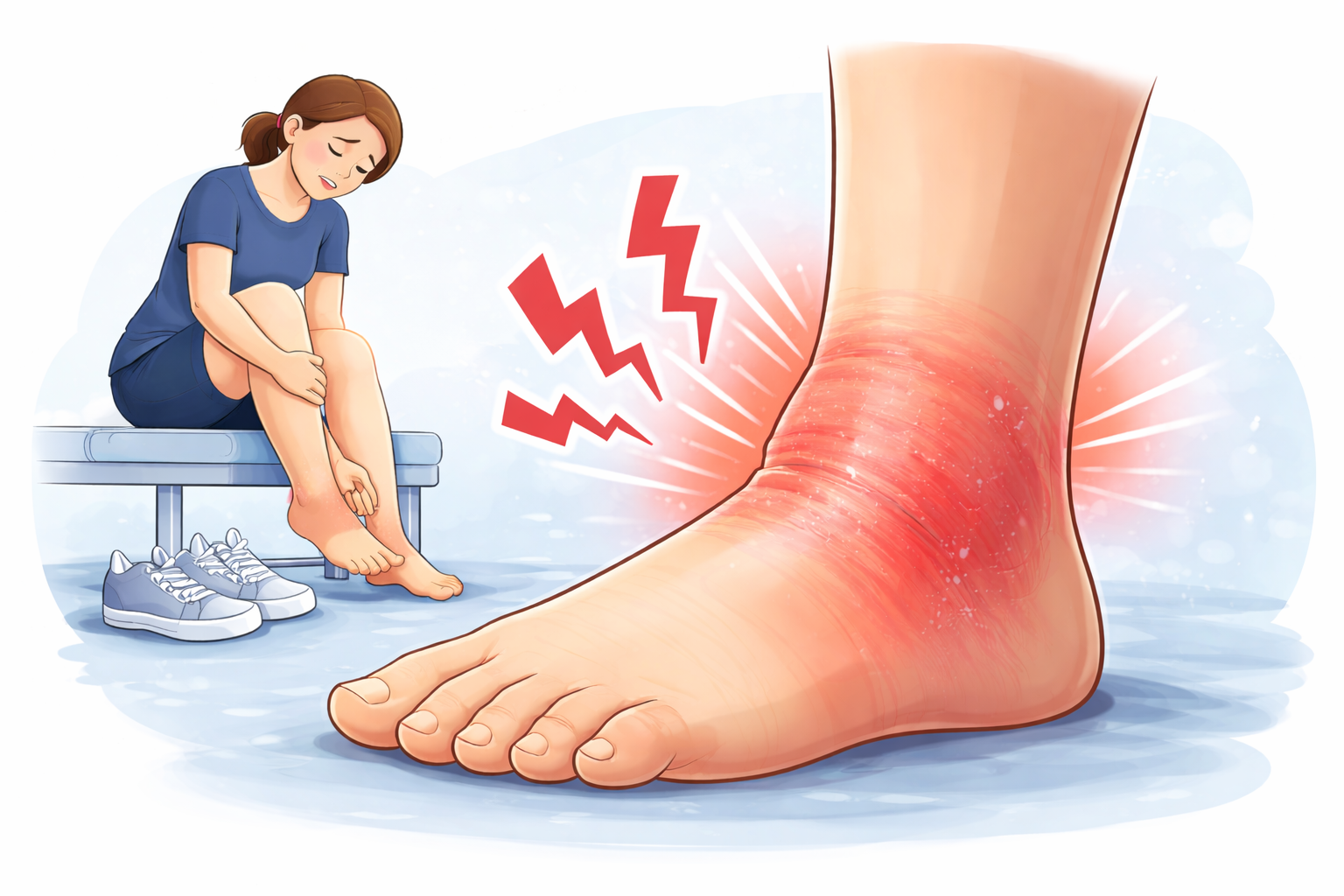
Night splints are specialized foot and ankle braces designed to be worn during sleep to treat plantar fasciitis and related foot pain conditions. These therapeutic braces maintain your ankle and foot in a specific position throughout the night, preventing the natural plantarflexion (downward pointing) that occurs during rest.
The primary mechanism behind night splints involves maintaining your ankle at approximately 90 degrees of dorsiflexion—essentially keeping your toes pointing upward toward your shin. This position creates a gentle stretch across the plantar fascia, the thick band of tissue that supports your arch and connects your heel to your toes. By preventing overnight tissue contraction, night splints address one of the fundamental problems that make morning pain so intense.
When you sleep, your feet naturally assume a relaxed, downward-pointing position. This allows both the plantar fascia and Achilles tendon to shorten and tighten over the 6-8 hours you spend in bed. The first steps you take upon waking suddenly stretch these contracted tissues, causing that characteristic sharp, stabbing pain that many patients describe as feeling like stepping on glass.

Night splints work by interrupting this cycle of overnight shortening and morning trauma. The brace keeps the plantar fascia stretched and supported all night long, ensuring continuous relief and support. The immediate benefits include reduced morning heel pain, improved mobility upon waking, and decreased overall inflammation in the affected tissues. Many patients report being able to walk normally within minutes of getting out of bed, rather than experiencing the prolonged limping and gradual pain reduction that typically characterizes untreated plantar fasciitis mornings.
The effectiveness of night splints lies in their ability to maintain therapeutic positioning for extended periods without requiring conscious effort from the patient. While you sleep, the splint does the work of keeping your tissues at their optimal length for healing and recovery.
The Science Behind Overnight Stretching
Understanding the anatomy of the plantar fascia helps explain why overnight stretching is so effective for heel pain relief. The plantar fascia is a tough, fibrous band of connective tissue that acts like a bowstring, supporting your foot’s arch and absorbing shock during walking and standing. This tissue experiences significant stress throughout the day, developing microscopic tears and inflammation that characterize plantar fasciitis.
Why Does the Plantar Fascia Shorten Overnight?
During rest periods, particularly the prolonged inactivity of sleep, the plantar fascia naturally shortens as part of the body’s protective response to injury. This tissue contraction serves a biological purpose—it helps immobilize damaged areas to prevent further injury. However, this same protective mechanism becomes problematic when you resume activity, as the shortened fascia must suddenly stretch to accommodate normal foot function. Rest is an important part of the recovery plan for plantar fasciitis, but it can also make the pain worse if not balanced with gentle stretches.
Benefits of Sustained Passive Stretching
The physiological benefits of sustained passive stretching for 6-8 hours are well-documented in research:
Maintains tissue length and flexibility
Reduces scar tissue formation
Promotes proper healing
Types of Night Splints: Comfort vs. Aggressive Models
The market offers two main types of night splints, each designed to address different patient needs and comfort preferences. Understanding the differences between comfort-oriented and aggressive models helps ensure you select the most appropriate option for your specific situation and tolerance level.
Comfort-Oriented Dorsal Night Splints
Dorsal night splints represent the comfort-oriented category and are typically recommended for first-time users or those with sensitivity to pressure. These lightweight devices attach to the top of your foot and shin, using adjustable straps to maintain dorsiflexion without completely encasing the foot. The dorsal design allows for better air circulation, reduces heat buildup, and provides a less restrictive feeling during sleep. Many patients find these models easier to adjust to and more tolerable for extended wear.
Aggressive Boot-Style Plantar Splints
Boot-style plantar splints offer more aggressive stretching and maximum therapeutic benefit for severe cases. These comprehensive devices encase the entire foot and lower leg, similar to a walking boot, and maintain precise positioning throughout the night. The boot design provides superior control over foot position and typically delivers a stronger, more consistent stretch to the plantar fascia and Achilles tendon. However, the increased effectiveness comes with reduced comfort and a longer adjustment period.
Adjustable models allow you to customize the degree of dorsiflexion based on your comfort level and treatment progression. These splints feature mechanisms that let you gradually increase the stretch as your tissues adapt, starting with gentle positioning and advancing to more aggressive stretching over time. Fixed-angle models maintain a predetermined position and are often preferred by patients who want consistent, predictable stretching without the complexity of adjustments.
The choice between soft padded versions and rigid shells depends on your specific comfort needs and pain severity. Soft splints use materials like neoprene and foam padding to provide cushioning and flexibility while maintaining therapeutic positioning. Rigid shells, typically made from hard plastic or lightweight metals, offer maximum support and stretch but may require a longer adjustment period.
When choosing between comfort and aggressiveness, consider several factors: the severity of your morning pain, your ability to sleep with devices on your feet, the duration of your symptoms, and your previous experience with orthotic devices. Patients with mild to moderate symptoms often achieve excellent results with comfort models, while those with severe, chronic plantar fasciitis may benefit from the more aggressive approach of boot-style splints.
Clinical Effectiveness and Research Evidence
The clinical effectiveness of night splints for plantar fasciitis has been thoroughly documented through multiple research studies spanning several decades. These investigations provide compelling evidence for the therapeutic value of overnight stretching in managing heel pain and improving long-term outcomes for patients with chronic foot pain.
A significant 2007 study examined 53 feet treated with night splints and demonstrated remarkable improvement rates within just two months of consistent use. The research tracked patients with chronic plantar fasciitis who had failed to respond to conventional treatments including rest, ice, stretching, and anti-inflammatory medications. After eight weeks of nightly splint use, 68% of participants reported significant pain reduction and improved morning mobility.
The groundbreaking 1999 randomized clinical trial represents one of the most comprehensive investigations into night splint effectiveness. This study followed 116 patients with diagnosed plantar fasciitis, comparing outcomes between those using night splints and control groups receiving standard care. The research methodology included objective pain measurements, functional assessments, and long-term follow-up to evaluate sustained benefits.
Perhaps most importantly, the study revealed a dramatic difference in recurrence rates between treatment groups. Patients who used night splints consistently showed only a 13.6% recurrence rate of symptoms compared to 29% in non-users over a 12-month follow-up period. This finding suggests that night splints not only provide immediate relief but also contribute to long-term resolution of plantar fasciitis.
Several factors affect treatment success rates, with research identifying key predictive elements. Age over 45 appears to correlate with better outcomes, possibly due to reduced activity levels and better compliance with wearing schedules. The duration of symptoms before starting night splint therapy also influences effectiveness, with patients who begin treatment within six months of symptom onset showing superior results compared to those with chronic conditions lasting over a year.
Compliance emerges as the most critical factor determining success. Studies consistently show that patients who wear their splints for at least six hours per night achieve significantly better outcomes than those with irregular use patterns. The research emphasizes that sporadic use provides minimal benefit, while consistent nightly wear creates the sustained tissue adaptation necessary for lasting improvement.
The research methodology employed in these studies involved careful patient selection, standardized outcome measures, and objective assessment tools. Participants underwent thorough examinations to confirm plantar fasciitis diagnoses, excluding those with other foot conditions that might confound results. Pain levels were measured using validated scales, and functional improvements were assessed through standardized walking tests and daily activity questionnaires.
Preventing Foot Drop: An Overlooked Benefit of Night Splints
Night splints are widely recognized for their effectiveness in treating plantar fasciitis and reducing that familiar morning heel pain. However, they also offer a lesser-known but important benefit: preventing foot drop. Foot drop is a condition where patients experience difficulty lifting the front part of the foot, which can lead to walking challenges and an increased risk of tripping. This issue can arise from various foot conditions, including nerve injuries, muscle weakness, or prolonged inactivity.
How Night Splints Help Prevent Foot Drop
By keeping your foot in a supportive dorsiflexion position throughout the night, a plantar fasciitis night splint provides a gentle stretch not only to the plantar fascia and Achilles tendon but also helps maintain the muscles and nerves responsible for lifting the foot. This positioning reduces tension and stress on the ankle and calf, helping to prevent the tightening and weakness that contribute to foot drop.
Who Can Benefit from Night Splints for Foot Drop Prevention?
Night splints are especially valuable for those managing multiple foot conditions such as:
Plantar fasciitis
Achilles tendonitis
Early signs of foot drop
The gentle stretch provided by the splint helps reduce inflammation, promote healthy blood flow, and minimize the risk of further complications.
Types of Night Splints for Foot Drop Prevention
There are two main types of night splints to consider:
Boot-style (plantar) splints: Offer firm, comprehensive support ideal for patients with severe symptoms or higher risk for foot drop.
Dorsal splints: Provide a more flexible fit, often preferred for milder cases or those prioritizing comfort.
Both types typically feature adjustable straps and a supportive design, allowing customization for extended wear without sacrificing comfort.
Combining Night Splints with Other Treatments
For enhanced results, night splints can be combined with other therapies such as orthotic insoles, physical therapy, and activity modifications. This comprehensive approach helps you regain a pain-free, active life.
For more information on complementary treatments for foot and ankle pain, consider exploring our guide on shockwave therapy for foot and ankle pain and strategies to improve patient safety and mobility in our fall risk assessment guide.
Consult a Healthcare Professional
It is important to consult with a healthcare professional like Evolve Health to determine the best type of night splint and treatment plan tailored to your specific symptoms and health needs.
By addressing plantar fasciitis and helping to prevent foot drop and related complications, night splints offer a comprehensive, cost-effective solution for managing heel pain, reducing morning pain, and supporting overall foot health.
Combining Night Splints with Daytime Insoles

A synergistic approach combining night stretching with daytime arch support creates a comprehensive treatment strategy that addresses plantar fasciitis around the clock. While night splints work to maintain optimal tissue length during sleep, supportive insoles provide crucial arch support and cushioning during the high-stress periods of standing, walking, and daily activities.
The combination strategy recognizes that plantar fasciitis requires both passive stretching and active support to achieve lasting relief. Night splints prevent overnight tissue shortening and morning trauma, while quality insoles reduce the repetitive stress that perpetuates inflammation and tissue damage throughout the day. This dual approach attacks the problem from multiple angles, creating optimal conditions for tissue healing and pain reduction.
Types of orthotic insoles that complement night splint therapy include arch support insoles, heel cups, and custom orthotics. Over-the-counter arch supports provide immediate relief for many patients and cost significantly less than custom options. These prefabricated insoles offer structured support that helps maintain proper foot alignment and reduces plantar fascia stress during daily activities.
Heel cups focus specifically on cushioning and supporting the heel area, where plantar fasciitis pain typically originates. These devices provide targeted relief by redistributing pressure away from sensitive heel bone areas while offering shock absorption during walking and standing. Many patients find heel cups particularly effective when combined with night splints, as the combination addresses both the stretching and cushioning aspects of treatment.
Timing recommendations for optimal treatment coordination involve wearing night splints during all sleeping periods and transitioning to supportive insoles immediately upon waking. Keep your insoles next to your bed so you can slip them into your house slippers or shoes before taking your first steps. This seamless transition from night stretching to daytime support prevents the sudden stress that can trigger morning pain episodes.
Cost-effective treatment combinations maximize therapeutic benefit while minimizing expenses. Patients can pair a quality night splint with well-designed over-the-counter arch supports for optimal results, often providing excellent relief at a fraction of the cost of custom orthotics or more invasive treatments. Many patients achieve significant relief with this combination, making it an ideal first-line approach before considering more expensive options.
The transition between night and day treatments should become a natural part of your routine. Before removing your night splint in the morning, have your supportive footwear ready to provide immediate cushioning and support. Avoid walking barefoot on hard surfaces, as this can immediately stress the newly-stretched plantar fascia and trigger pain episodes.
Top 3 Night Splints We Recommend Daily
Based on extensive clinical experience and patient feedback, we’ve identified three exceptional night splints that consistently deliver outstanding results for plantar fasciitis treatment. Each offers unique advantages that make them suitable for different patient needs and preferences. BraceAbility night splints have received various customer ratings, with some products rated as high as 4.2 out of 5 stars, reflecting their effectiveness and user satisfaction.
Feature | Active Innovations Dorsal | Corflex Padded 90 Degree | FUTURO Plantar Support |
|---|---|---|---|
Type | Dorsal lightweight design | Boot-style aggressive | Adjustable comfort |
Comfort Rating | 9/10 | 7/10 | 8/10 |
Effectiveness | 8/10 | 9/10 | 8/10 |
Price Range | $35-45 | $45-60 | $25-35 |
Best For | First-time users | Severe symptoms | Budget-conscious |
Adjustability | Limited | Fixed angle | Fully adjustable |
Sleep Quality | Excellent | Good | Very good |
The Active Innovations Dorsal Night Splint earns top marks for comfort and ease of use, making it ideal for patients new to night splint therapy. Its lightweight design attaches only to the top of the foot, allowing for better air circulation and reduced bulk in bed. The adjustable straps provide a secure fit without creating pressure points, and most patients adapt to wearing it within just a few nights.
The Corflex Padded 90 Degree Night Splint delivers maximum therapeutic benefit through its boot-style design that maintains precise positioning throughout the night. This model provides the most aggressive stretch, making it particularly effective for patients with severe morning pain or chronic plantar fasciitis that hasn’t responded to other treatments. The additional padding helps offset the more restrictive design.
The FUTURO Plantar Fasciitis Night Support offers excellent value with fully adjustable features that allow you to customize the stretch based on your comfort level and treatment progression. Its versatile design works well for a wide range of foot sizes and shapes, and the moderate price point makes it accessible for patients seeking effective treatment without premium costs. The Runkelai Plantar Fasciitis Night Splint features a soft memory foam pad for added comfort, making it another excellent option for those prioritizing comfort during therapy.
For those interested in exploring these options further, you can find detailed specifications, sizing guides, and patient reviews by visiting our recommended products, where we provide a carefully curated selection of effective night splints for plantar fasciitis.

When selecting between these options, consider your primary goals and tolerance for device bulk. If comfort and easy adaptation are your main concerns, the Active Innovations dorsal model provides the smoothest introduction to night splint therapy. For maximum therapeutic effect, particularly with severe symptoms, the Corflex boot-style option delivers superior results despite requiring a longer adjustment period.
You can grab the exact night splints we give patients from our carefully curated selection, where we provide detailed specifications, sizing guides, and patient reviews to help you make the best choice for your specific needs. BraceAbility offers a variety of night splints for plantar fasciitis, including both dorsal and plantar styles, ensuring options for different preferences and treatment needs.
How to Use Night Splints Properly
Proper usage of your plantar fasciitis night splint begins with a gradual adjustment period that allows your body to adapt to sleeping with the device. Start by wearing the splint for just 2-3 hours before gradually increasing the duration by one hour each night until you can comfortably wear it throughout your entire sleep period. This progressive approach prevents discomfort and helps ensure long-term compliance. For best results, it is recommended to wear night splints consistently for several weeks and consult a healthcare professional for proper fitting.
Proper Fitting
Proper fitting represents the foundation of successful night splint therapy. The device should hold your ankle at approximately 90 degrees of dorsiflexion—imagine standing against a wall with your toes pulled toward your shin. The splint should feel snug but not painfully tight, and you should be able to wiggle your toes freely within the device. Excessive tightness can restrict blood flow and create pressure points that interfere with sleep quality.
Sizing Considerations
Sizing considerations vary significantly between manufacturers, so always consult the specific sizing chart for your chosen model. Most splints accommodate a range of foot sizes through adjustable straps and padding, but selecting the correct initial size ensures optimal fit and effectiveness. Measure your foot length and ankle circumference according to the manufacturer’s guidelines, and consider sizing up if you’re between sizes.
Sleep Position Modifications
Sleep position modifications can significantly improve your comfort level while wearing a night splint. Many patients find that sleeping on their back or on the side opposite the affected foot provides the most comfortable position. If you typically sleep on your stomach, you may need to use additional pillows to support the splinted leg and prevent awkward positioning that could cause discomfort or reduce effectiveness.
Daily maintenance and cleaning instructions help extend the life of your splint while maintaining hygiene. Remove any removable padding and wash it separately according to manufacturer instructions—typically in cool water with mild soap. The main splint components can usually be cleaned with antibacterial wipes or a damp cloth with gentle soap. Allow all components to dry completely before reassembling to prevent odor and material degradation.
Signs of proper fit include the ability to sleep comfortably for at least 6 hours, absence of pressure points or red marks upon removal, and gradual improvement in morning pain over 2-4 weeks of consistent use. The splint should maintain your foot in the correct position without slipping or sliding during sleep, and you should notice reduced stiffness when taking your first steps each morning.
Warning signs that indicate need for adjustment include persistent pain or pressure points, numbness or tingling in your foot or toes, skin irritation or breakdown, or inability to sleep due to discomfort after several weeks of gradual adjustment. These symptoms suggest that the splint may be too tight, improperly positioned, or inappropriate for your specific foot anatomy.
Complementary Treatments to Maximize Results
Morning stretching routines enhance the benefits of night splint therapy by maintaining tissue flexibility as you transition from sleep to active movement. Begin each day with gentle calf stretches and plantar fascia stretches before putting weight on your feet. The towel stretch, performed while sitting on the edge of your bed, provides an excellent bridge between overnight stretching and standing activities.
Ice therapy and anti-inflammatory strategies work synergistically with night splints to control inflammation and pain. Apply ice to your heel for 15-20 minutes in the evening before putting on your night splint, and again in the morning if you experience any residual discomfort. The combination of cold therapy and sustained stretching helps reduce inflammation while promoting tissue healing.
Footwear modifications represent a crucial component of comprehensive plantar fasciitis treatment. Choose shoes with adequate arch support, cushioned soles, and proper heel height (approximately 1-2 inches). Avoid walking barefoot on hard surfaces, and consider keeping supportive slippers beside your bed for immediate use upon waking. Quality footwear maintains the benefits of night splint therapy throughout your active hours.
Heel cushioning options provide targeted relief during daily activities. Gel heel pads, foam inserts, and specialized heel cups can significantly reduce the impact forces that stress the plantar fascia during walking and standing. These simple additions to your regular footwear help prevent re-injury while your tissues heal and strengthen.

Activity modifications help reduce daily plantar fascia stress while your night splint therapy promotes healing. Avoid high-impact activities like running or jumping until your symptoms improve significantly. Replace these activities with low-impact alternatives such as swimming or cycling that maintain cardiovascular fitness without stressing your feet. Gradually return to higher-impact activities as your symptoms resolve.
Physical therapy exercises work synergistically with night splint therapy to address strength imbalances and biomechanical factors contributing to plantar fasciitis. Focus on exercises that strengthen your calf muscles, improve ankle flexibility, and enhance overall foot and leg alignment. A qualified physical therapist can design a specific program that complements your night splint use and addresses your individual needs.
The key to maximizing results with complementary treatments lies in consistency and timing. Perform stretching routines daily, apply ice therapy regularly, wear supportive footwear consistently, and maintain activity modifications until your symptoms resolve. This comprehensive approach addresses all aspects of plantar fasciitis while your night splint provides the foundation of overnight tissue management.
When to See a Healthcare Provider
Professional evaluation becomes particularly important if you have diabetes, circulation problems, or other health conditions that affect foot health and healing. These comorbidities may require specialized treatment approaches and closer monitoring to prevent complications while using night splints and other conservative treatments.
The decision to seek professional care shouldn’t be delayed if you experience severe symptoms or notice signs of infection such as increased redness, warmth, or discharge from any areas where the splint contacts your skin. Early intervention can prevent complications and help ensure that your treatment plan remains safe and effective.
Seeking Expert Care for Coastal Lifestyles in Boynton Beach
Living an active, coastal lifestyle in Boynton Beach means your feet take on unique stresses from activities like beach walking, water sports, and outdoor recreation. If plantar fasciitis or foot pain interferes with your ability to enjoy these activities, it’s essential to seek expert care tailored to your needs.
At Evolve Health, we understand the demands of Boynton Beach lifestyles and offer comprehensive evaluation and personalized treatment plans. You can easily schedule at our local clinic to receive specialized care that addresses your foot health and helps you get back to the activities you love.
Integration with medical treatments and injection therapy may become necessary for chronic or severe cases that don’t respond adequately to conservative measures alone. Corticosteroid injections, platelet-rich plasma therapy, or other advanced treatments can be combined with continued night splint use to provide comprehensive symptom management and promote healing.
Long-term management strategies for chronic cases often involve ongoing use of night splints combined with lifestyle modifications, orthotic support, and regular monitoring. Healthcare providers can help develop sustainable treatment plans that prevent symptom recurrence while maintaining your quality of life and activity levels.
Professional evaluation becomes particularly important if you have diabetes, circulation problems, or other health conditions that affect foot health and healing. These comorbidities may require specialized treatment approaches and closer monitoring to prevent complications while using night splints and other conservative treatments.
The decision to seek professional care shouldn’t be delayed if you experience severe symptoms or notice signs of infection such as increased redness, warmth, or discharge from any areas where the splint contacts your skin. Early intervention can prevent complications and help ensure that your treatment plan remains safe and effective.
FAQs
How long should I wear a night splint each night?
For optimal results, it is recommended to wear a night splint for 6 to 8 hours during sleep. Starting with shorter periods and gradually increasing wear time can help your body adjust comfortably to the device. Are night splints uncomfortable to wear?
Comfort levels vary depending on the type and fit of the splint. Comfort-oriented dorsal splints tend to be lighter and less restrictive, making them easier to tolerate, especially for first-time users. Boot-style splints provide a firmer stretch but may require an adjustment period. Proper sizing and gradual wear time increase can improve comfort.
How soon will I notice improvement after using a night splint?
Many patients begin to notice reduced morning pain and improved mobility within 2 to 4 weeks of consistent use. Significant relief typically occurs within 2 to 3 months. Consistency in wearing the splint every night is crucial for effective results.
Can I walk or move around while wearing a night splint?
Night splints are designed to be worn while resting or sleeping and are not intended for walking. It is important to remove the splint before getting out of bed to avoid injury or falls.
Are night splints suitable for everyone with plantar fasciitis?
While night splints are beneficial for many patients, those with severe foot deformities, circulation problems, or certain medical conditions should consult a healthcare provider before use. A professional evaluation ensures the splint is appropriate and properly fitted.
Conclusion
Night splints for plantar fasciitis represent one of the most effective conservative treatments available for heel pain and morning stiffness. The science behind overnight stretching is compelling—by maintaining your plantar fascia at optimal length for 6-8 hours each night, these devices interrupt the cycle of tissue shortening and morning trauma that perpetuates plantar fasciitis symptoms.
The choice between comfort-oriented and aggressive models depends on your individual needs, tolerance, and symptom severity. Whether you select a lightweight dorsal splint for ease of use or a more comprehensive boot-style device for maximum therapeutic benefit, consistency remains the key to success. Research consistently demonstrates that patients who wear their splints regularly achieve significantly better outcomes than those with sporadic use patterns.
Combining night splints with daytime arch support, proper footwear, and complementary treatments creates a comprehensive approach that addresses plantar fasciitis throughout the entire day. This synergistic strategy maximizes your chances of achieving lasting relief while preventing symptom recurrence.
Remember that night splint therapy requires patience and persistence. Most patients begin noticing improvement within 2-4 weeks of consistent use, with significant relief typically achieved within 2-3 months. The investment in quality night splints and commitment to regular use can provide lasting benefits that far outweigh the temporary inconvenience of adapting to sleeping with the device.
Don’t let another morning begin with that sharp, stabbing pain in your heel. Take action today by grabbing the exact night splints we give patients and starting your journey toward pain-free mornings and improved mobility.