Vascular vs lymphatic Causes of leg and foot swelling
Peripheral edema—the medical term for swelling in legs and feet—occurs when excess fluid accumulates in your body’s tissues. Edema occurs when blood vessels, especially tiny capillaries, leak fluid that becomes trapped in the surrounding tissues, leading to swelling.
As fluid builds up, symptoms such as swollen ankles may develop. Understanding whether your swelling stems from vascular (blood circulation) problems or lymphatic (drainage system) issues is crucial because each requires different treatment approaches.
Vascular causes
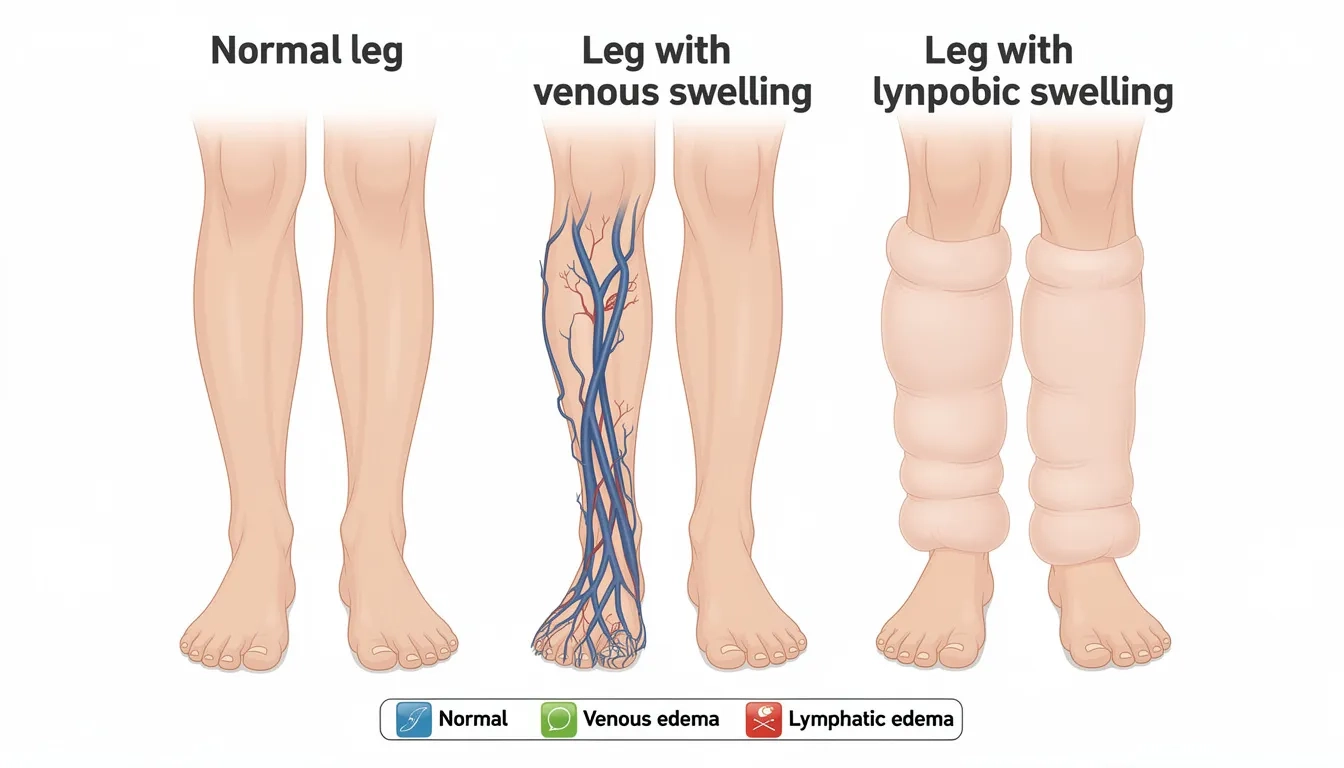
Chronic venous insufficiency represents the most common vascular cause of leg swelling. When one-way valves in your leg veins become incompetent, blood flows backward and pools in dependent veins, raising venous pressure and forcing fluid into surrounding tissues. This typically causes:
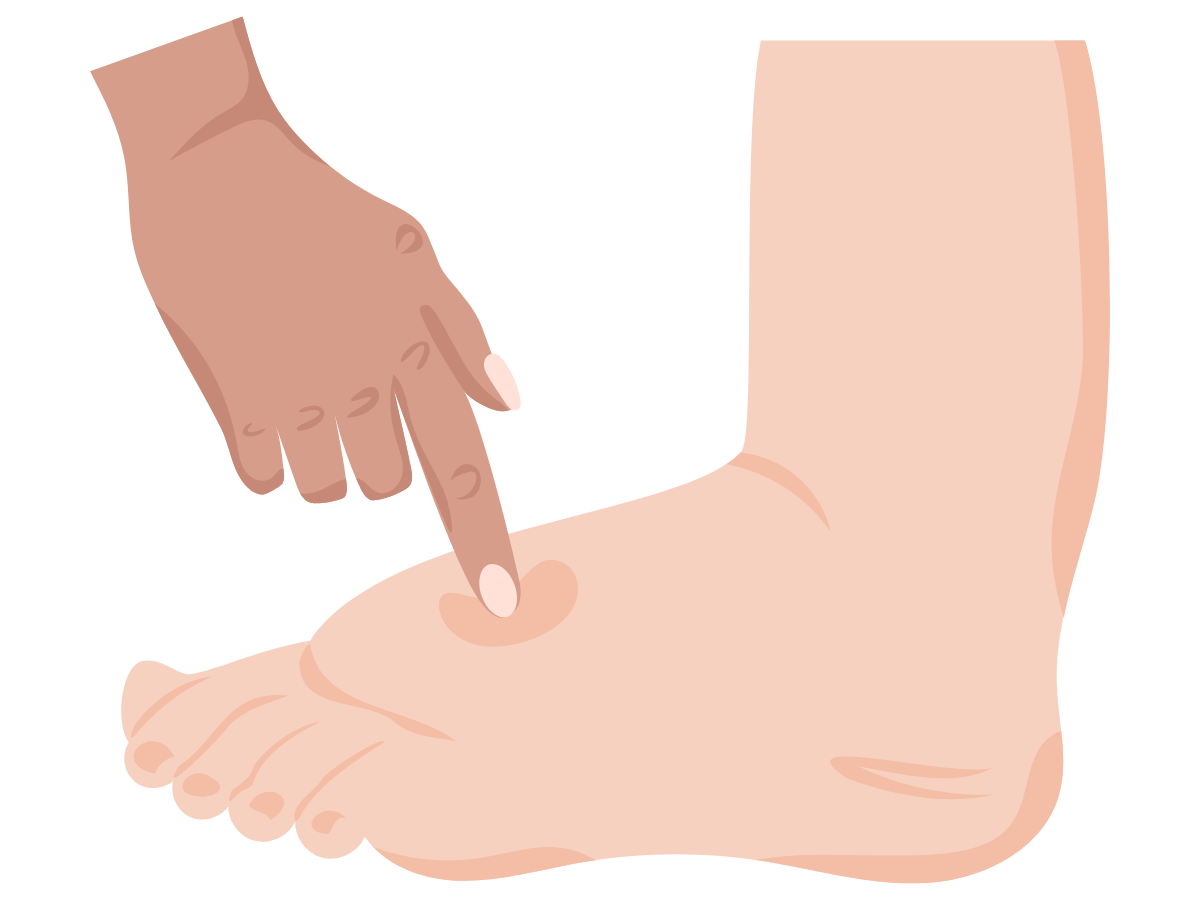
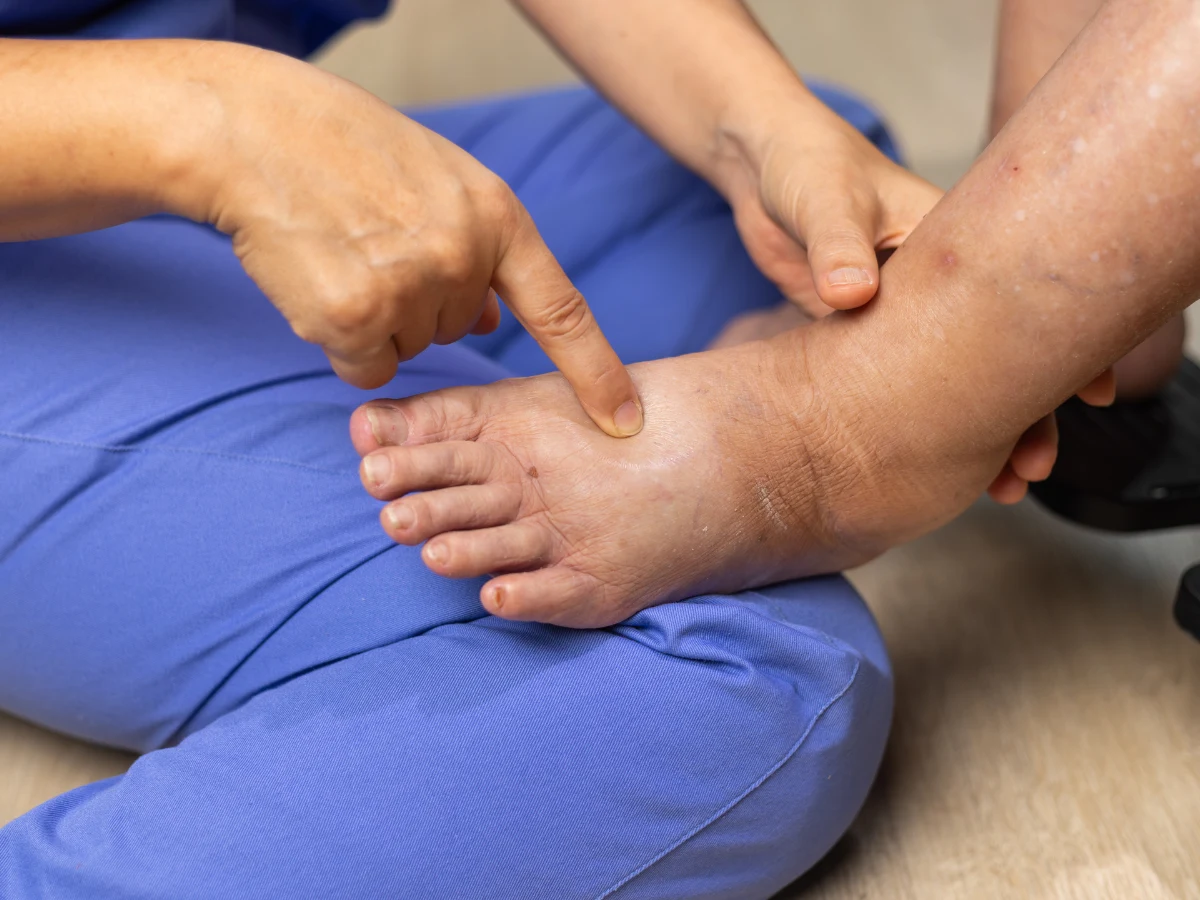
Pitting edema around ankles and lower legs that’s worse after prolonged standing
Brown hemosiderin pigmentation around the ankles
Varicose veins and spider veins
Stasis dermatitis or venous eczema
Bilateral swelling that improves overnight with elevation
Deep vein thrombosis (DVT) creates acute vascular obstruction when a blood clot forms in deep leg veins. Unlike chronic venous insufficiency, DVT typically causes sudden, unilateral leg swelling accompanied by pain, warmth, and redness in the affected leg.
Heart failure and other systemic conditions disrupt normal blood circulation, leading to bilateral dependent leg edema. Fluid buildup occurs because reduced cardiac output triggers neurohormonal activation, causing sodium and water retention that manifests first in the feet and ankles. Swelling in the lower legs can also be caused by right-sided congestive heart failure, known as cardiac edema.
Certain medicines, such as blood pressure medicines (particularly calcium channel blockers like amlodipine) and NSAIDs, can cause leg, ankle, or foot swelling as a side effect. Hormonal therapies can also contribute to fluid retention and peripheral edema.
Lymphatic causes
Primary lymphedema results from congenital malformation of lymphatic vessels, while secondary lymphedema develops after cancer treatment, surgery, radiation, infection, or trauma damages the lymphatic system. Damage or blockage affecting lymph nodes can lead to fluid buildup and swelling, as lymph nodes play a crucial role in lymphatic drainage. Unlike venous edema, lymphedema often involves the dorsum of feet and toes, creating a characteristic “squared” toe appearance.
Mixed veno-lymphatic edema develops when longstanding venous hypertension overwhelms the lymphatic system’s drainage capacity. Regular movement of muscle and skin is necessary for the lymphatic system to effectively remove excess fluid. Over time, chronic venous insufficiency can progress to include lymphatic dysfunction, creating more complex swelling patterns.
Key distinguishing features of lymphatic swelling include:
Non-pitting edema in advanced stages
Thickened, fibrotic skin texture
Involvement of feet and toes
Recurrent cellulitis or skin infections
Progressive worsening despite elevation
Clinical differentiation
Healthcare providers distinguish vascular from lymphatic causes through several clinical features:
Pattern assessment: Bilateral swelling suggests systemic causes like heart failure or kidney disease, while unilateral swelling points toward DVT, localized venous disease, or lymphedema.
Timing evaluation: Sudden onset over hours to days indicates acute conditions like DVT, while gradual development over weeks to months suggests chronic venous insufficiency or lymphedema.
Physical characteristics: Pitting edema (leaves indentation when pressed) typically indicates venous or systemic causes, while non-pitting edema suggests lymphatic dysfunction or advanced chronic swelling.
Associated symptoms: Shortness of breath points toward heart or lung problems, while skin changes like brown pigmentation suggest chronic venous disease.
Accurate diagnosis guides appropriate treatment—diuretics work well for heart failure but provide little benefit for pure lymphedema, while compression therapy helps both venous and lymphatic conditions but must be avoided in severe peripheral arterial disease.
Diagnostic tests are often used to identify the underlying cause of swelling, providing detailed information necessary for accurate diagnosis. Persistent swelling in the legs may require a thorough examination to rule out serious conditions such as heart or kidney problems.
Common Symptoms and Red flags in Swollen Legs and Feet
Most leg and foot swelling begins subtly with evening puffiness that patients initially attribute to hot weather or prolonged standing. It is important to notice swelling early, as it can be an initial sign of vascular or systemic issues that may require prompt medical evaluation.
Swelling in the legs and feet can also be a sign of underlying health conditions such as heart failure, kidney disease, or liver disease. Understanding which symptoms indicate benign conditions versus those requiring urgent medical attention helps you respond appropriately to your swelling.
Typical benign symptoms
Evening ankle swelling that improves overnight represents the most common presentation of mild venous insufficiency. In mild cases, swelling often resolves with simple lifestyle changes such as leg elevation, reducing salt intake, or adjusting medications. Swelling may also occur in women who take estrogen, or during parts of the menstrual cycle.
This swelling typically:
Appears around the ankles and lower legs after standing or sitting for long periods
Creates pitting edema where pressing firmly leaves a temporary indentation
Improves significantly with leg elevation and overnight rest
Worsens during hot weather or after consuming too much salty food
Chronic skin changes develop gradually in persistent swelling conditions:
Shiny, stretched skin especially visible on the front of the shins
Brown or reddish discoloration around the ankles from venous stasis
Dry, flaky skin that may crack or develop eczema-like patches
Thickened, warty, or cobblestoned skin texture suggesting chronic lymphedema
Activity-related symptoms often accompany chronic leg edema:
Heaviness or aching in the legs after prolonged standing
Difficulty fitting into shoes later in the day
Sock marks that persist for hours after removal
General fatigue in the leg muscles
Red flag symptoms requiring urgent evaluation
Sudden unilateral swelling demands immediate medical assessment, especially when accompanied by:
• Calf pain or tenderness that worsens with walking
• Warmth and redness in the swollen area
• Visible surface veins on the affected leg
• Recent surgery, long travel, or prolonged immobilization
Systemic warning signs indicate potentially life-threatening conditions and require immediate medical care:
• Swelling combined with shortness of breath or chest discomfort
• Rapid weight gain of 3+ pounds over 2-3 days
• Swelling with fever, severe tenderness, or red streaking
• Trouble breathing when lying flat (orthopnea)
Swelling that worsens despite home care or is accompanied by symptoms like shortness of breath or chest pain should prompt a doctor’s visit due to potential serious underlying conditions.
Pregnancy-related concerns require immediate evaluation:
• Sudden or severe swelling during pregnancy
• Swelling with headaches, vision changes, or high blood pressure
• Any swelling accompanied by decreased fetal movement
These red flags may signal conditions ranging from blood clots and pulmonary embolism to heart failure decompensation or preeclampsia. When in doubt, seek same-day medical evaluation or immediate medical care rather than waiting to see if symptoms improve with home remedies.
Core Treatments: diuretics, elevation therapy, and compression protocols
Effective treatment for swelling in legs and feet typically combines targeted medication when indicated, mechanical strategies like elevation and compression, and lifestyle modifications tailored to the underlying cause. Early intervention is crucial to improve outcomes and prevent complications, so prompt consultation with a healthcare professional is recommended.
Home remedies for reducing edema include leg elevation, wearing compression socks, and engaging in regular, low-impact exercise such as walking or swimming. Success requires matching the treatment approach to whether your edema stems from vascular disease, lymphatic dysfunction, or systemic conditions.
The following sections present evidence-based protocols for:
Diuretic therapy—when these “water pills” help versus when they may cause harm
Elevation therapy—precise positioning techniques and daily schedules for maximum benefit
Compression protocols—medical-grade pressure levels, wear schedules, and realistic improvement timelines
These treatments should be supervised or initially guided by a healthcare provider, particularly if you have heart failure, kidney disease, diabetes, or peripheral arterial disease. We’ll also cover important safety considerations and when to modify standard protocols.
The key principle: identify whether fluid buildup results from systemic overload (requiring diuretics), mechanical circulatory problems (responding to elevation and compression), or lymphatic obstruction (needing specialized drainage techniques).
Diuretics: when they help, when they don’t, and expected timelines
Diuretics, commonly called “water pills,” remove excess fluid from the body by increasing kidney water and sodium excretion. However, these prescription medications treat specific causes of leg edema—not all forms of swelling respond to diuretic therapy. Early diagnosis is crucial to identify the underlying cause of leg and foot swelling, ensuring that the most effective treatment is chosen.
Appropriate diuretic uses:
Heart failure-related edema: Loop diuretics like furosemide represent first-line therapy for fluid overload from heart failure. Swelling in the lower legs can also be caused by right-sided congestive heart failure, known as cardiac oedema. Properly dosed diuretics typically begin reducing leg and foot swelling within 24-72 hours, with patients often noticing decreased ankle circumference and easier shoe fitting by the third day of treatment.
Kidney or liver-related edema: Patients with nephrotic syndrome, advanced chronic kidney disease, or cirrhosis may require diuretics combined with dietary sodium restriction. These conditions often need specialized monitoring by nephrology or hepatology specialists.
Medication-induced swelling: Short-term diuretic therapy can provide relief when calcium channel blockers or other medications cause ankle edema and the offending drugs cannot be immediately discontinued.
When diuretics are ineffective or harmful:
Pure lymphatic edema (lymphedema): Since lymphatic fluid contains high protein concentrations trapped in tissues, standard diuretics remove intravascular water but don’t address the underlying protein-rich lymph accumulation. Diuretics may actually worsen lymphedema by concentrating proteins in the interstitial space.
Isolated chronic venous insufficiency: For patients with varicose veins and venous valve incompetence without systemic fluid overload, compression therapy and elevation provide more benefit than chronic diuretic use, which can lead to electrolyte imbalances and kidney problems.
Required monitoring for diuretic therapy:
Baseline kidney function and electrolyte levels before starting treatment
Laboratory recheck after 7-10 days, sooner in older or frail patients
Daily weight monitoring at home to detect over-diuresis or rapid fluid reaccumulation
Regular blood pressure checks to avoid dangerous hypotension
Warning against self-treatment: Never start over-the-counter diuretics or use leftover prescription “water pills” without medical supervision. Unsupervised diuretic use, especially during hot weather or illness, can cause dangerous dehydration, kidney injury, and electrolyte disturbances in older adults.
Elevation therapy: precise positioning and daily schedule
Leg elevation represents one of the safest and most effective swollen legs remedies when performed correctly and consistently. Proper elevation leverages gravity to assist venous and lymphatic return, reducing hydrostatic pressure in leg vessels.
Correct positioning technique:
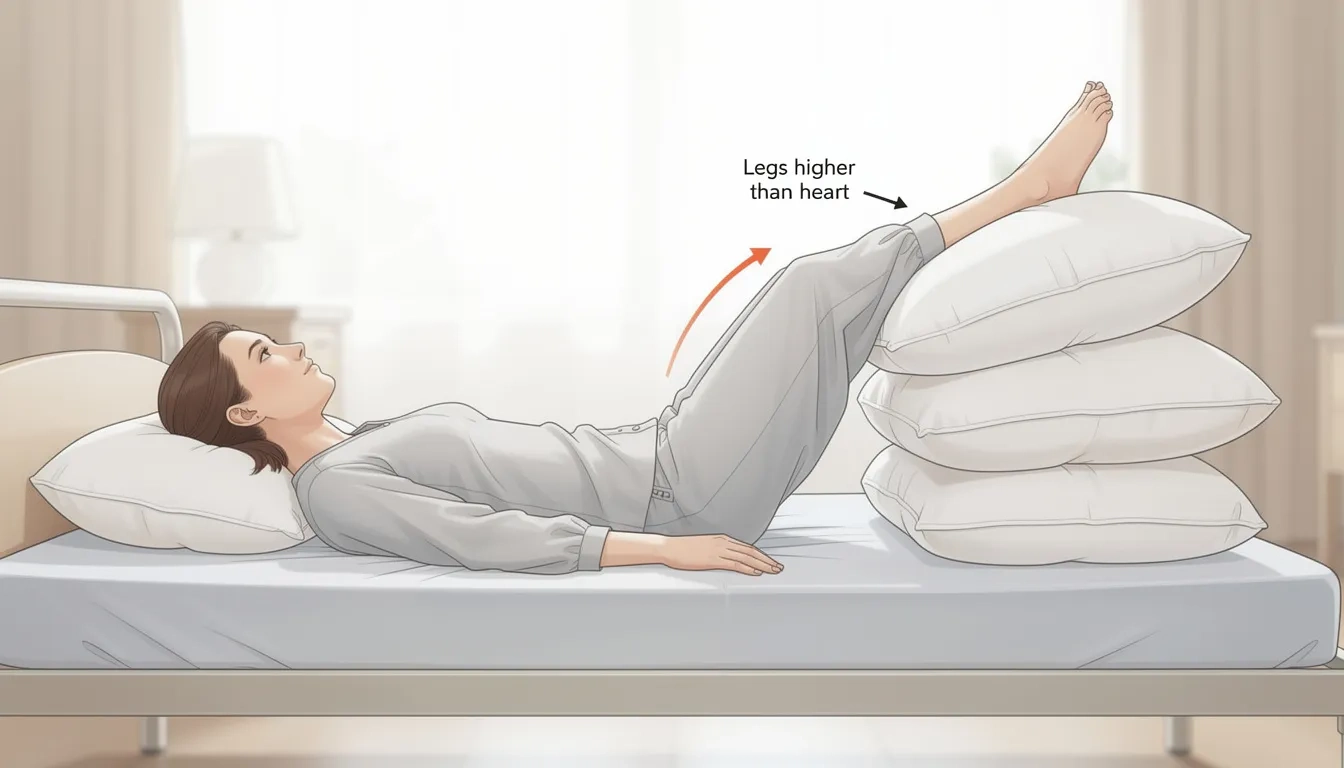
Position feet above heart level—not just on a low footstool or ottoman
Use 2-3 firm pillows or a foam wedge to angle legs at approximately 30-45 degrees
Ensure the entire leg from ankle to hip is supported to prevent pressure points
Lie flat on your back rather than sitting up, which maintains leg elevation above heart level
Daily elevation schedule:
Perform 15-30 minute elevation sessions 2-3 times daily
Schedule sessions for mid-afternoon and evening when swelling typically peaks
Add a longer 45-60 minute session after work shifts involving prolonged standing
Consider sleeping with the foot of the bed elevated 4-6 inches for severe venous insufficiency
Expected improvement timelines:
Mild daily swelling: People with mild ankle edema from prolonged standing often notice significant improvement within one week of consistent elevation therapy. Shoes may fit more comfortably, and visible ankle swelling diminishes noticeably.
Chronic venous or lymphatic edema: Established swelling from chronic venous insufficiency or lymphedema requires several weeks of regular elevation combined with compression therapy before measurable changes in leg circumference and skin texture become apparent.
Workplace modifications for prevention:
Standing workers should take 2-5 minute walk-and-flex breaks every hour
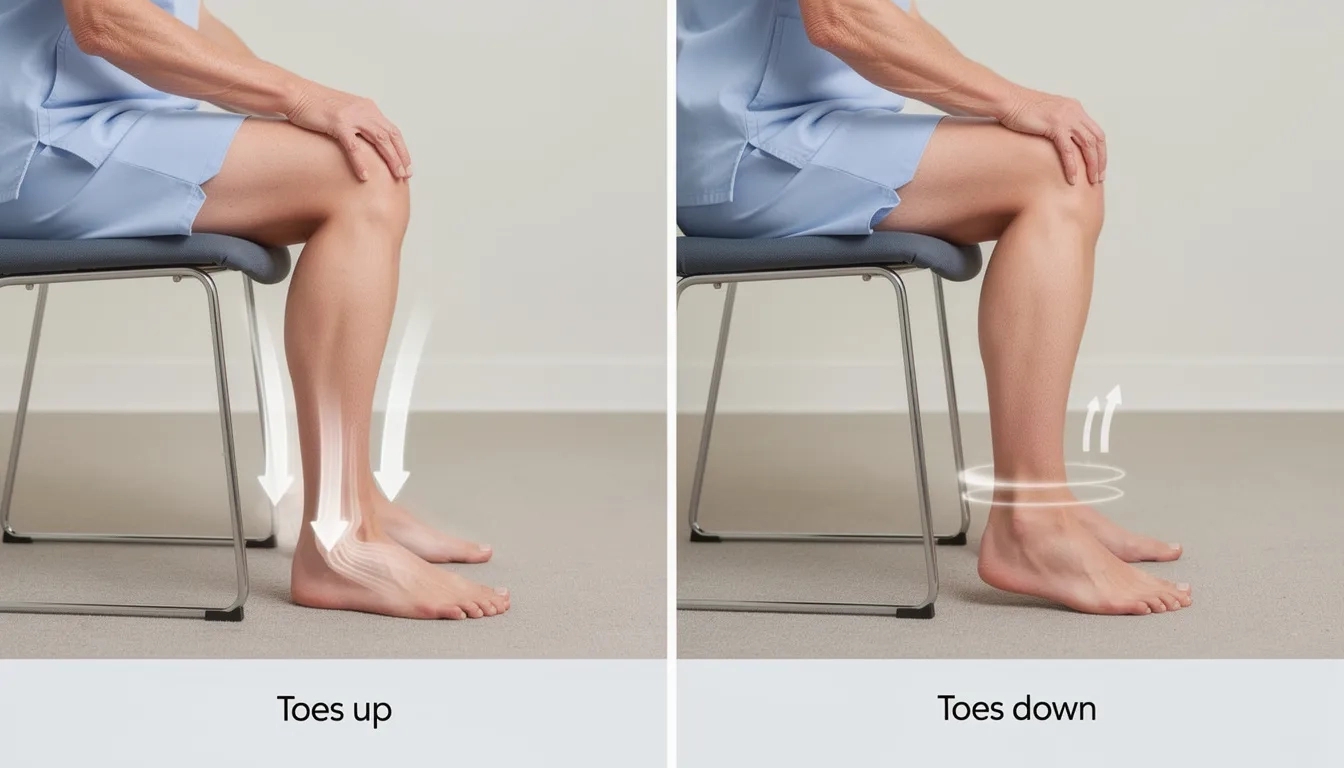
Desk workers should avoid letting legs dangle; use a footrest and perform ankle pump exercises (flexing feet up and down) several times hourly
Travelers should walk airline aisles or stop cars frequently during long trips
Remember that elevation therapy alone rarely resolves moderate or severe edema but significantly enhances the effectiveness of compression stockings and appropriate medical treatments when used in combination.
Compression therapy: Stockings, Wraps, and Protocols by Severity
Compression therapy forms the backbone of leg edema treatment for venous and many lymphatic causes. External pressure from properly fitted garments reduces venous diameter, improves valve function, accelerates blood flow, and assists lymphatic drainage.
Wearing compression garments is essential for reducing swelling and maintaining mobility, especially in cases of lymphedema.
Types of compression devices:
Graduated compression stockings provide highest pressure at the ankle, decreasing up the calf or thigh. These come in knee-high, thigh-high, or pantyhose styles depending on the distribution of swelling.
Compression pressure classes (measured in mmHg):
Light compression (8-15 mmHg): Mild daily swelling, travel prevention
Moderate compression (15-20 mmHg): Early venous insufficiency, mild varicose veins
Medical-grade compression (20-30 mmHg): Chronic venous insufficiency, moderate lymphedema
Firm medical compression (30-40 mmHg): Advanced venous disease, severe lymphedema, ulcer prevention
Protocol examples by condition severity:
For mild swelling: Start with 15-20 mmHg knee-high stockings worn during waking hours and removed at bedtime. Reassess symptoms and swelling reduction after 2-4 weeks of consistent use.
For moderate venous edema: Use 20-30 mmHg medical-grade stockings combined with daily elevation therapy. Most patients notice reduced heaviness and aching within days, with measurable circumference reduction over 2-6 weeks.
For advanced lymphedema: Begin with multi-layer compression bandaging or higher-pressure wraps supervised by a certified lymphedema therapist, then transition to custom-fitted compression garments for long-term management. Wearing compression garments is a key part of controlling lymphedema, as it helps reduce swelling and maintain mobility.
Realistic improvement timelines:
Symptom relief (reduced heaviness, aching, and fatigue) often occurs within days of starting appropriate compression
Visible reduction in ankle and calf circumference typically measures over 2-4 weeks of consistent daily use
Skin texture improvements and reduced discoloration may take several months in chronic conditions. Wearing compression garments and reducing salt in the diet often relieves edema.
Daily wear protocol:
Apply compression stockings first thing in the morning before significant swelling develops
Remove garments at bedtime unless specifically directed otherwise by a lymphedema specialist
Replace stockings every 4-6 months as elastic compression degrades with washing and wear
For properly fitted, medical-grade compression gear that meets clinical standards, grab clinic-trusted compression gear rather than relying on pharmacy or department store alternatives that may provide inadequate pressure or improper fit.

Home Remedies and lifestyle changes for leg edema treatment
While medical-grade compression, elevation, and targeted medications form the foundation of effective treatment, daily lifestyle habits strongly influence how much swelling patients experience. Regular exercise and movement can improve circulation and help reduce swelling.
Lifestyle factors contributing to edema include prolonged sitting or standing, high salt intake, obesity, and pregnancy. Evidence-informed home remedies can significantly enhance the effectiveness of your primary treatment plan.
Exercise and movement strategies
Regular low-impact exercise improves both venous and lymphatic circulation:
Walking 20-30 minutes daily activates the calf muscle pump, helping push fluid upward
Pool walking or water aerobics provides hydrostatic pressure while exercising
Stationary cycling promotes leg muscle contractions without prolonged standing
Yoga poses involving leg elevation can combine stretching with therapeutic positioning
Targeted muscle activation exercises:
Ankle pump exercises (pointing and flexing feet) can be performed hourly during desk work
Calf raises help strengthen the muscle pump mechanism
Seated leg extensions activate quadriceps muscles that assist venous return
Activity modification for swelling prevention:
Avoid uninterrupted sitting or standing for more than 1-2 hours
Take movement breaks during long flights, car trips, or work shifts
Alternate sitting and standing throughout the workday when possible
Elevate legs during lunch breaks or while watching television
Dietary and fluid management
Sodium intake moderation helps prevent fluid retention:
Limit processed foods, canned soups, and restaurant meals high in sodium
Read food labels and choose products with less than 140mg sodium per serving
Use herbs, spices, and lemon juice instead of salt for flavoring
Be aware that high-salt diets can reduce the effectiveness of both diuretics and compression therapy
Fluid balance considerations:
Maintain adequate hydration—dehydration can worsen swelling by triggering fluid retention
Avoid extreme fluid restriction unless specifically directed by a cardiologist or nephrologist
Limit alcohol consumption, which can contribute to fluid imbalances
Monitor caffeine intake, as excessive amounts may affect fluid regulation
Weight management and footwear
Gradual weight loss in overweight individuals provides multiple benefits:
Reduces pressure on veins and lymphatic vessels in the legs
Decreases overall fluid volume and cardiac workload
Improves mobility, making elevation and exercise easier to maintain
Even modest weight loss (5-10% of body weight) can significantly reduce leg swelling
Appropriate footwear selection:
Choose flat or low-heeled shoes that provide adequate support
Avoid high heels that impair calf muscle pump function
Ensure shoes have adjustable features (laces or velcro) to accommodate daily size variations
Replace tight socks or hosiery that create constricting bands around calves or ankles
Skin care and infection prevention
Protective skin care becomes especially important with chronic edema:
Apply fragrance-free moisturizers daily to prevent cracking and breakdown
Keep feet clean and dry, paying attention to areas between toes
Inspect legs and feet daily for cuts, sores, or signs of infection
Seek prompt medical attention for any wounds that don’t heal within a few days
Important limitation: While topical creams and gels marketed for swelling may provide temporary comfort, they cannot address the underlying vascular or lymphatic problems causing fluid accumulation. Focus on proven mechanical treatments while using topical products only for skin protection and comfort.
Remember that home remedies work best as supplements to—not replacements for—appropriate medical treatment. Persistent or worsening swelling despite consistent home care warrants professional evaluation to identify and treat underlying conditions.
When Compression, Diuretics, or Elevation Therapy May Be Unsafe or Require Modification
Standard treatment protocols for leg and foot swelling, also known as edema, must sometimes be adjusted or avoided in certain medical conditions to ensure safety and effectiveness.
In some cases, leg and foot swelling may indicate a serious underlying condition, such as Peripheral Arterial Disease (PAD), which requires prompt medical evaluation to prevent complications. Understanding these contraindications and necessary precautions is essential for safe management of swelling.
Compression Therapy Precautions
Compression therapy is a cornerstone treatment for many causes of leg swelling; however, it may be unsafe in patients with significant arterial insufficiency. Peripheral arterial disease (PAD) reduces blood flow to the legs, and applying high-pressure compression garments can further impair circulation, risking tissue damage.
Warning signs of PAD include cold or numb feet and toes (often in one leg), leg pain during walking (claudication), non-healing wounds or sores on the feet or lower legs, and weak or absent pulses in the feet. Before initiating compression therapy above 15-20 mmHg, patients suspected of having PAD should undergo vascular assessment, including ankle-brachial index testing. Those with severe arterial disease may require lower pressure garments or alternative treatments.
Signs that compression is too tight include numbness, tingling, pain, coldness or bluish discoloration of toes, worsening wounds, or inability to tolerate the garment. Patients with diabetic neuropathy may not feel these symptoms and require careful monitoring.
Diuretic Therapy Safety Considerations
Diuretics, or “water pills,” help reduce fluid buildup but must be used cautiously in certain populations. Older adults are at higher risk of dehydration, blood pressure drops, kidney injury, dizziness, and electrolyte imbalances when using diuretics.
Patients with kidney disease need specialized dosing and monitoring due to reduced kidney function and increased risk of electrolyte disturbances. Additionally, diuretics can interact adversely with blood pressure medications, NSAIDs, lithium, digoxin, and other drugs, necessitating careful medical supervision.
Elevation Therapy Modifications
Elevation therapy assists venous and lymphatic return by positioning the legs above heart level but may require adjustments for some patients. Those with severe heart failure may experience shortness of breath when lying flat (orthopnea), and patients with respiratory conditions like COPD or sleep apnea may need gradual position changes or modified elevation with the upper body slightly raised.
Mobility limitations from recent surgeries (hip, knee, back) or severe arthritis may require padding or alternative positioning. Patients with balance issues should have assistance when changing positions.
During pregnancy, especially after the first trimester, flat back positioning should be avoided due to supine hypotensive syndrome; side-lying with legs elevated on pillows is a safer alternative. Any sudden, severe swelling during pregnancy warrants immediate medical evaluation.
Understanding these precautions and modifying treatment accordingly helps ensure safe and effective management of leg and foot swelling for diverse patient needs.
Professional evaluation recommendations
Before starting intensive treatment protocols, certain patients benefit from vascular assessment:
Anyone with suspected arterial disease based on symptoms or risk factors
Patients with diabetes, especially those with neuropathy
Those with multiple cardiovascular risk factors or known heart disease
People taking blood thinners or with history of bleeding complications
A comprehensive evaluation typically includes pulse examination, ankle-brachial index measurement, and sometimes duplex ultrasound to assess both arterial and venous circulation safely.
Remember that these precautions don’t necessarily prevent treatment—they guide appropriate modifications to ensure both safety and effectiveness of your leg edema treatment plan.
When to suspect and rule out DVT (deep vein thrombosis)
Deep vein thrombosis represents a medical emergency disguised as simple leg swelling. People may experience swelling in one leg due to DVT, but swelling in the legs can also indicate serious conditions like heart failure, kidney failure, or liver failure.
This blood clot in a deep leg vein can break loose and travel to the lungs, causing potentially fatal pulmonary embolism. Recognizing DVT symptoms and seeking prompt evaluation can be life-saving.
Hallmark DVT symptoms and presentation
Classic DVT features that distinguish it from benign swelling:
Unilateral involvement: DVT typically affects only one leg, creating noticeable asymmetry between limbs. This contrasts with heart failure, kidney disease, or medication-related edema that usually causes bilateral swelling.
Rapid onset timeline: Swelling from DVT develops over hours to a few days rather than the gradual progression seen in chronic venous insufficiency or lymphedema that worsens over weeks to months.
Associated pain patterns:
New calf or thigh pain, often described as cramping or aching
Pain that worsens when standing, walking, or flexing the foot upward
Tenderness along the path of deep veins, particularly in the calf
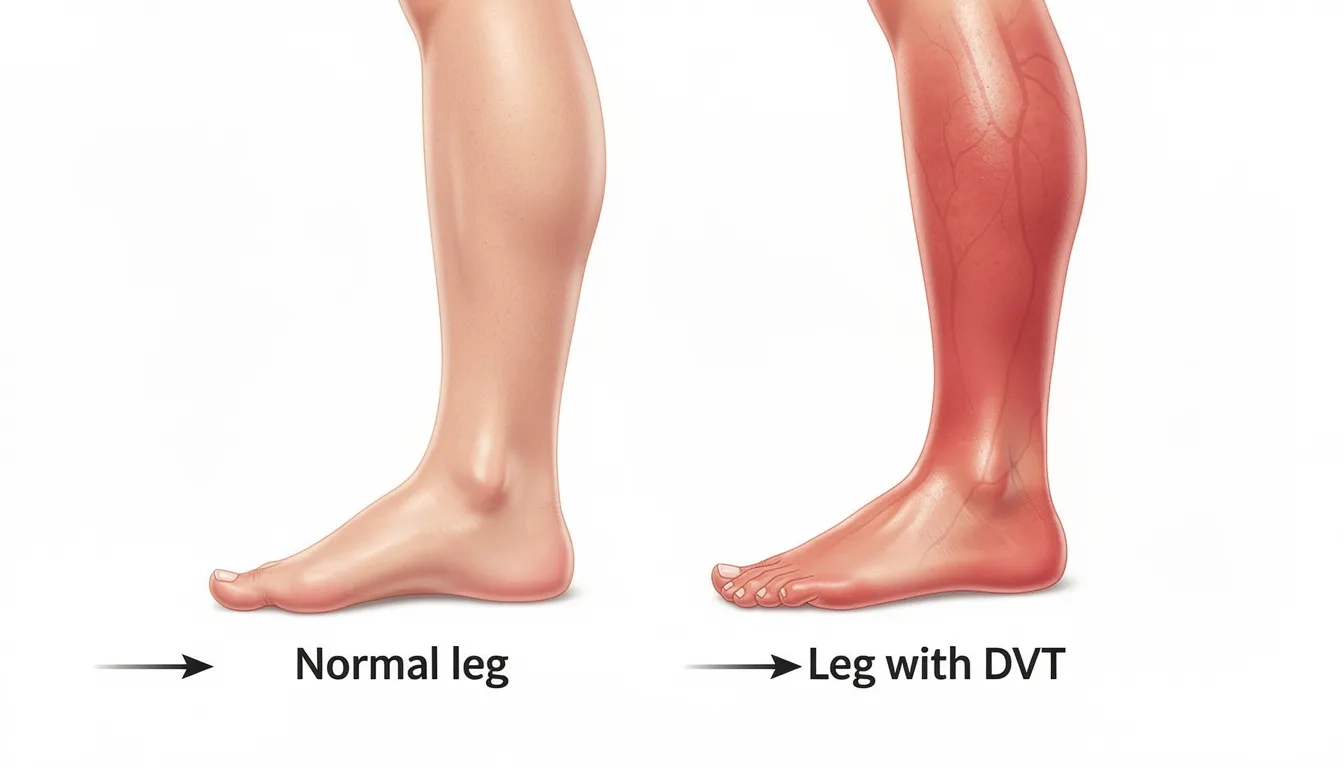
Physical signs:
Warmth in the affected leg compared to the unaffected side
Redness or discoloration over the swollen area
Visible dilated surface veins as blood seeks alternative pathways
Swelling that extends from the foot up into the calf or thigh
Major DVT risk factors
Recent surgical procedures dramatically increase clot risk:
Hip, knee, pelvic, or abdominal surgery within the past 3 months
Any major surgery requiring general anesthesia and prolonged bed rest
Orthopedic procedures involving bone or joint manipulation
Immobilization events:
Long-haul flights over 4-6 hours without adequate movement
Extended car trips with limited stopping and leg movement
Prolonged bed rest due to illness or injury
Plaster casts or immobilization devices on lower extremities
Medical conditions and medications:
Active cancer diagnosis or ongoing chemotherapy treatment
Pregnancy or the first 6 weeks after delivery
Estrogen-containing birth control or hormone replacement therapy
Personal or family history of previous blood clots
Known inherited clotting disorders (thrombophilia)
Critical response protocols
What NOT to do when DVT is suspected:
Do not massage the swollen, painful leg
Avoid applying heat pads or taking hot baths
Don’t rely solely on over-the-counter pain medications while delaying medical care
Never assume symptoms will resolve on their own
When to seek emergency care immediately:
Sudden, unexplained swelling in one leg with pain
Any leg swelling accompanied by chest pain, sudden shortness of breath, or coughing up blood (potential signs of pulmonary embolism)
Swelling with severe pain that prevents walking or weight-bearing
Same-day urgent evaluation needed for:
New unilateral leg swelling in anyone with risk factors
Swelling with calf tenderness and warmth
Any doubt about whether symptoms could represent DVT
Diagnostic approach and treatment urgency
Standard diagnostic testing for suspected DVT includes:
Duplex venous ultrasound to visualize blood flow and detect clots
D-dimer blood test (though this can be elevated in many conditions)
Clinical assessment using validated scoring systems
Why prompt diagnosis matters:
Early anticoagulation (blood thinning) treatment prevents clot extension
Reduces risk of life-threatening pulmonary embolism
Minimizes long-term complications like post-thrombotic syndrome
If you suspect DVT based on symptoms and risk factors, don’t wait to see if improvement occurs with elevation or compression. Schedule a same-day vascular check for immediate ultrasound evaluation and appropriate treatment if a clot is confirmed.
Remember: missed DVT can be fatal, while prompt treatment is highly effective and safe. When in doubt, seek urgent medical evaluation rather than risking a potentially catastrophic outcome.
Effective Treatment for Leg and Foot Swelling at Evolve Health
At Evolve Health, we understand how leg and foot swelling can impact your daily life and mobility. Our physician-led multi-specialty clinics in Florida and Texas offer comprehensive care tailored to the underlying cause of your edema. Whether your swelling is due to vascular issues, lymphatic dysfunction, or systemic conditions like heart failure, our expert team utilizes a combination of targeted diuretics, elevation therapy, and properly fitted medical-grade compression to reduce swelling effectively and safely.
Our approach begins with a thorough physical examination and diagnostic testing to identify the root cause of your leg and foot swelling. We then develop a personalized treatment plan that may include lifestyle modifications, advanced compression therapy, and, when appropriate, medication management. We emphasize early diagnosis and intervention to prevent complications and improve your quality of life.
To learn more about the common causes of foot swelling and effective treatments, visit our detailed guide at Why Do My Feet Swell. If you are ready to take the next step toward relief, schedule a consultation with our specialists.
Frequently Asked Questions (FAQs)
1. What causes leg and foot swelling?
Leg and foot swelling, or edema, can result from fluid trapped in the body’s tissues due to conditions such as chronic venous insufficiency, deep vein thrombosis, lymphatic system failure, heart failure, kidney disease, or side effects of certain medications.
2. How does Evolve Health diagnose the cause of swelling?
Our specialists perform a comprehensive physical examination, review your medical history, and utilize diagnostic tests such as duplex ultrasound and blood work to determine the precise cause of your swelling and tailor your treatment accordingly.
3. Are compression stockings effective for reducing swelling?
Yes, wearing properly fitted medical-grade compression stockings helps improve blood flow and lymphatic drainage, reducing fluid buildup and discomfort. At Evolve Health, we ensure you receive the right compression level and fit for your condition.
4. When should I seek immediate medical care for leg swelling?
Seek urgent care if you experience sudden swelling in one leg accompanied by pain, redness, warmth, or if swelling is associated with chest pain or difficulty breathing, as these may indicate a blood clot or other serious condition.
5. Can lifestyle changes help manage leg and foot swelling?
Absolutely. Regular low-impact exercise, leg elevation, maintaining a healthy weight, reducing salt intake, and avoiding prolonged standing or sitting can help reduce swelling and improve circulation.
Conclusion
Managing leg and foot swelling effectively requires a precise diagnosis and a comprehensive treatment plan tailored to your unique needs. At Evolve Health, our expert team is dedicated to providing personalized care using proven medical treatments combined with lifestyle guidance to reduce edema and restore your mobility. Don’t let swelling limit your life—explore our resources and connect with our specialists today to start your journey toward healthier legs and feet.