What is Morton’s Neuroma (Interdigital Neuroma)?
Morton’s neuroma occurs when the tissue around one of the digital nerves leading to your toes becomes thick and inflamed. Despite being called a “neuroma,” this condition isn’t actually a tumor that can become cancerous. Instead, it’s a thickening of the nerve tissue caused by chronic irritation and pressure.
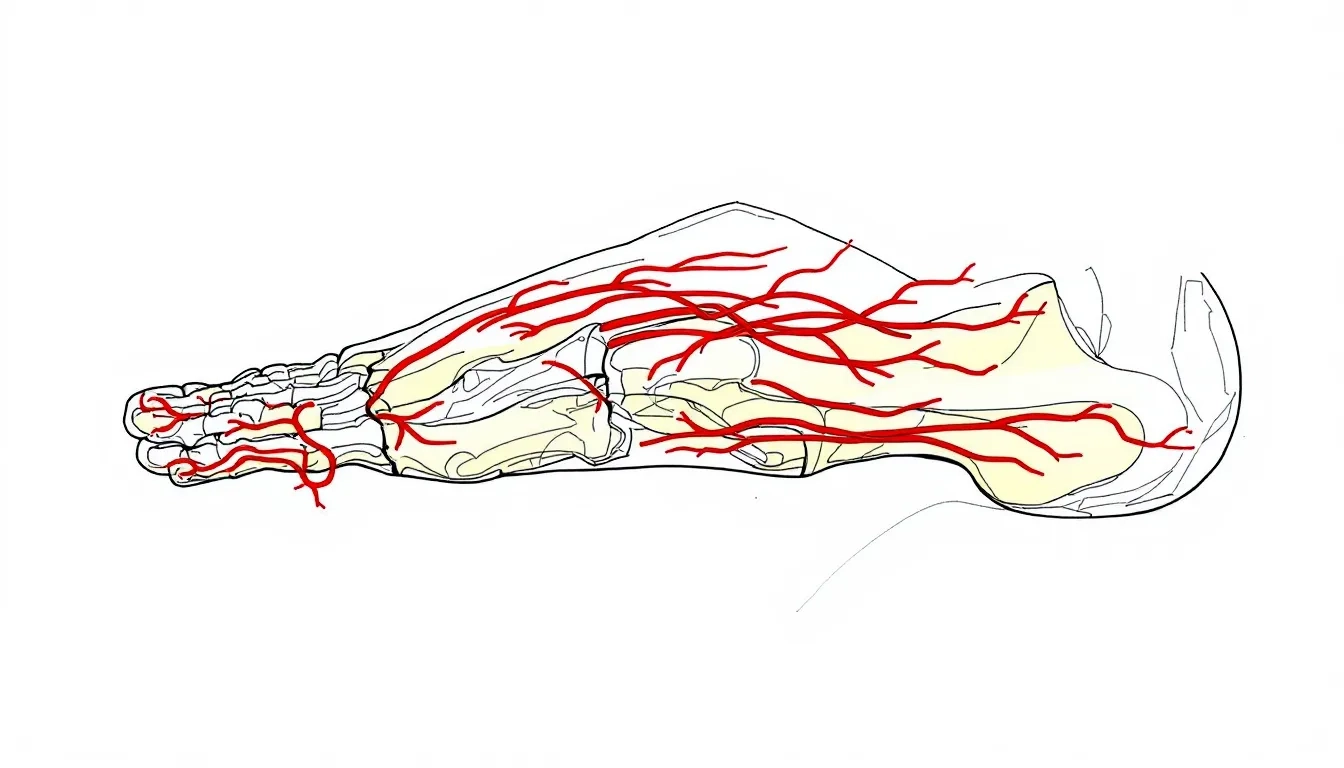
The condition most commonly develops between the metatarsal bones that connect to your third and fourth toes, though it can also occur between other toe bones. This area is particularly vulnerable because the nerve passes through a narrow space where it can easily become compressed.
Branches from the lateral plantar nerves, which join with the common digital nerves in this region, can also contribute to the development of Morton’s neuroma through compression and trauma.
Key facts about Morton’s neuroma:
• Affects approximately 8-33 per 100,000 adults annually
• Women are 4-8 times more likely to develop the condition than men
• 85% of cases occur between the third and fourth toes
• Most common in people aged 40-60
• Also known as interdigital neuroma or Morton’s entrapment
• Can affect one or both feet, though bilateral cases are less common
The affected nerve becomes irritated due to repeated compression, leading to inflammation and eventually the formation of fibrous tissue around the nerve. This process creates the characteristic symptoms that make walking uncomfortable and can significantly impact your quality of life.
Morton’s Neuroma Symptoms
The common symptoms of Morton’s neuroma are distinctive and often described in very specific ways by patients. Understanding these common symptoms can help you recognize when you might need medical attention and differentiate this condition from other causes of foot pain.
The most common symptom is sharp pain, burning pain in the ball of your foot, particularly in the area between your affected toes. This burning pain often feels like an electric shock that shoots through your foot and may radiate into the adjacent toes.
Many patients describe the sensation as feeling like they’re “walking on a marble” or having a pebble stuck in their shoe that they can’t shake out. Persistent pain in the ball of the foot is a hallmark symptom of Morton’s neuroma.

Additional symptoms include:
• Tingling and numbness between the affected toes
• Symptoms may include tingling or numbness spreading into the toes
• A sensation of thickness or swelling in the ball of the foot
• Pain that worsens when you wear shoes, especially tight shoes or high heels
• Discomfort that intensifies during walking, running, or standing for long periods
• Relief when you remove your shoes, massage your foot, or rest
• Pain that may radiate up into your leg in severe cases
• Night pain that can wake you from sleep in advanced cases
The symptoms begin gradually and tend to worsen over time if left untreated. In some cases, multiple Morton’s neuromas can develop, causing similar symptoms in different areas of the forefoot. Initially, you might only notice discomfort when wearing certain shoes or after prolonged activity. However, as the condition progresses, the pain can become constant and significantly interfere with daily activities.
What makes Morton’s neuroma particularly frustrating is that the pain often improves when you remove your shoes and massage the affected area, leading many people to initially attribute their discomfort to poor footwear choices rather than an underlying medical condition.
Causes and Risk Factors
Morton’s neuroma develops when the digital nerve becomes compressed and irritated over time. Understanding the primary causes and risk factors can help you make informed decisions about prevention and treatment.
The exact cause isn’t always clear, but the condition typically results from repetitive trauma or pressure on the nerve between your toe bones. When the metatarsal bones squeeze the nerve repeatedly, it becomes inflamed and eventually develops the characteristic thickening that causes symptoms.

Several factors significantly increase your risk of developing Morton’s neuroma:
Footwear Choices
Wearing high-heeled shoes that force weight onto the ball of your foot
Tight shoes or narrow shoes that compress the toes together
Shoes without adequate arch support or cushioning
Footwear with a narrow toe box that doesn’t allow proper toe spacing
Foot Structure and Biomechanics
High arches that place extra pressure on the ball of your foot
Flat feet can lead to nerve compression
Bunions or hammertoes that alter normal foot mechanics
Previous foot injuries that have changed your gait or foot structure
Activity-Related Factors
High-impact sports like running, tennis, or basketball
Activities that involve repetitive stress on the forefoot
Occupations requiring prolonged standing or walking
Sudden increases in activity level without proper conditioning
Demographics
Being female (women develop the condition 4-8 times more often than men)
Age between 40-60 years
Having excess weight that increases pressure on your feet (making efforts to lose weight can help reduce your risk of developing Morton’s neuroma)
Previous history of foot problems or ankle conditions
The combination of these risk factors often determines who develops Morton’s neuroma. For example, a middle-aged woman who wears high-heeled shoes regularly and has bunions faces a much higher risk than someone who wears appropriate footwear and has normal foot anatomy.
Diagnosis and When to See a Doctor
Recognizing when to seek medical attention is crucial for effective treatment of morton’s neuroma. Early diagnosis often leads to better outcomes with nonsurgical treatment options, while delayed diagnosis may require more aggressive interventions.
You should consult a foot and ankle surgeon from Evolve Health in Florida or Texas, or your primary care physician if you experience persistent forefoot pain that doesn’t improve with rest and proper footwear. Specifically, seek medical attention if your symptoms last more than a few days, interfere with daily activities, or continue to worsen despite conservative measures.
During your appointment, your healthcare provider will conduct a thorough medical history and physical exam. They’ll ask about your symptoms, when they started, what makes them better or worse, and review your shoe wear habits and activity level.
As part of this evaluation, your provider will also assess your general health to inform both the diagnosis and the most suitable treatment options. This information helps determine whether your symptoms are consistent with morton’s neuroma or another ankle condition.
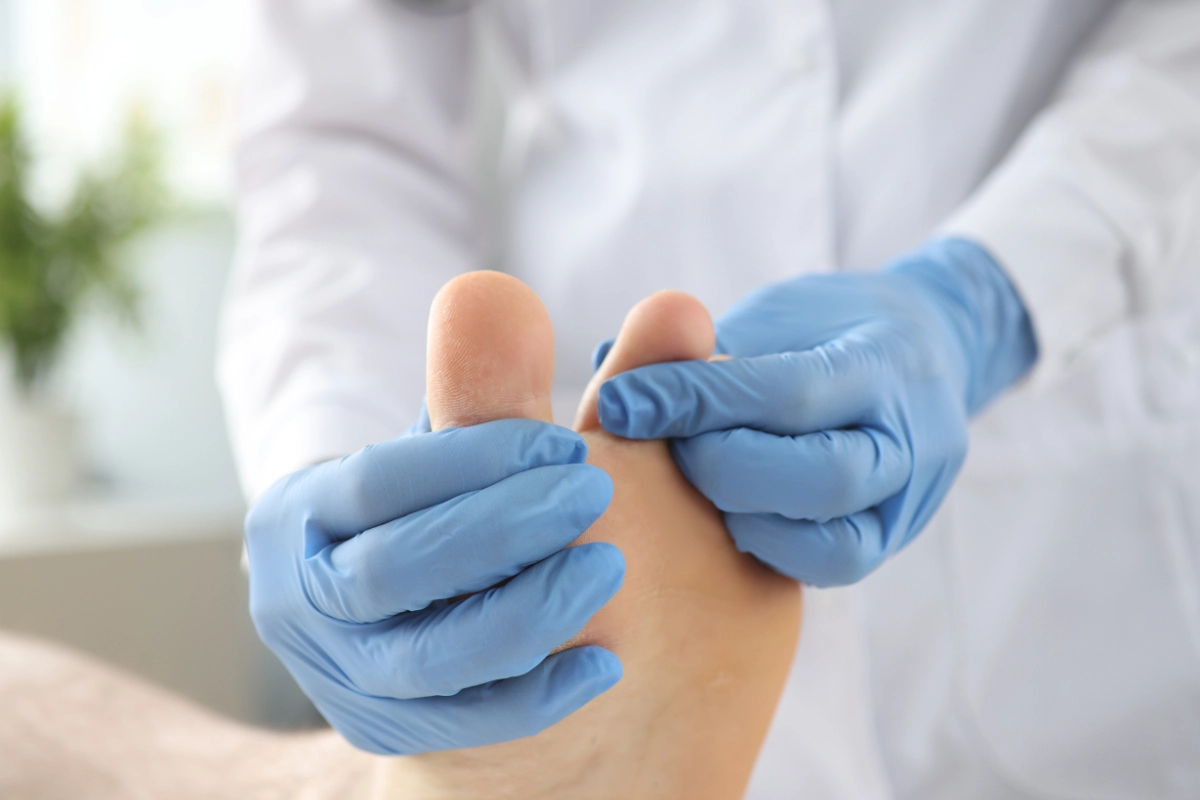
The physical examination typically includes several specific tests:
Mulder’s Click Test: Your doctor will squeeze the sides of your foot while pressing on the area between your toes. A positive test produces a clicking sensation and reproduces your pain, strongly suggesting morton’s neuroma. Another diagnostic method, the thumb index finger squeeze test, can also reproduce symptoms of Morton’s neuroma during examination.
Foot Squeeze Test: Pressure applied to the sides of your foot while compressing the area between the metatarsal bones can reproduce symptoms and help locate the affected nerve.
Range of Motion Assessment: Your provider will evaluate how your foot and ankle move to identify any biomechanical issues that might contribute to nerve compression.
Most cases of morton’s neuroma can be diagnosed based on your symptoms and physical examination alone. However, if the diagnosis is unclear or symptoms don’t respond to initial treatment, your doctor may recommend imaging studies.
Magnetic resonance imaging (MRI) can visualize the thickened nerve tissue and rule out other causes of forefoot pain. Ultrasound is another option that can effectively identify morton’s neuromas and is often less expensive than an MRI. X-rays are typically normal in morton’s neuroma but may be ordered to exclude bone problems or arthritis.
Your healthcare provider will also consider other conditions that can cause similar symptoms, including stress fractures, metatarsalgia, arthritis, or other forms of nerve damage. This differential diagnosis process ensures you receive the most appropriate treatment plan for your specific condition.
Non-Surgical Treatment Options For Morton Neuroma
The good news about morton’s neuroma is that many people find significant relief with nonsurgical treatment approaches. Conservative management is always the first line of therapy and can be highly effective, especially when started early in the course of the condition. These approaches aim to improve symptoms and quality of life.
The foundation of conservative treatment involves modifying the factors that contribute to nerve compression and inflammation. Success with these approaches requires patience and consistency, as improvement often takes several weeks to months.
Footwear Modifications
The most important step is changing to appropriate footwear that reduces pressure on the affected nerve. This means choosing shoes with a wide toe box that allows your toes to spread naturally, avoiding high heels that shift weight to the ball of your foot, and selecting shoes with good arch support and cushioning.
Avoid choosing to wear tight shoes, as this can worsen symptoms and increase nerve compression. Athletic shoes with these features are often ideal for daily wear during treatment. If you must wear dress shoes for work, look for styles with lower heels (less than 2 inches) and roomier toe areas.
Orthotic Devices and Padding
Custom or over-the-counter shoe inserts can help redistribute pressure away from the painful area. Metatarsal pads are particularly useful – these small cushions are placed behind the ball of your foot to help separate the metatarsal bones and reduce pressure on the nerve.
Orthotic devices prescribed by a foot specialist can address underlying biomechanical issues like high arches or flat feet that contribute to nerve compression. These custom inserts often provide better long-term results than generic options.
Anti-Inflammatory Medications
Over-the-counter anti-inflammatory medications like ibuprofen or naproxen can help reduce inflammation around the affected nerve and provide pain relief. These medications are most effective when taken regularly as directed, rather than only when pain is severe.
Activity Modification
Temporarily reducing high-impact activities that worsen your symptoms allows the inflamed nerve tissue to heal. This doesn’t mean complete bed rest, but rather avoiding activities that consistently reproduce your pain while maintaining general fitness through low-impact alternatives like swimming or cycling.
Physical Therapy and Other Treatments
A physical therapist can teach you exercises to improve foot mechanics, strengthen supporting muscles, and address any gait abnormalities that contribute to nerve compression. They may also use techniques like ultrasound therapy or specialized massage to reduce inflammation.
Icing the affected area for 15-20 minutes several times daily can help control inflammation and provide temporary pain relief.
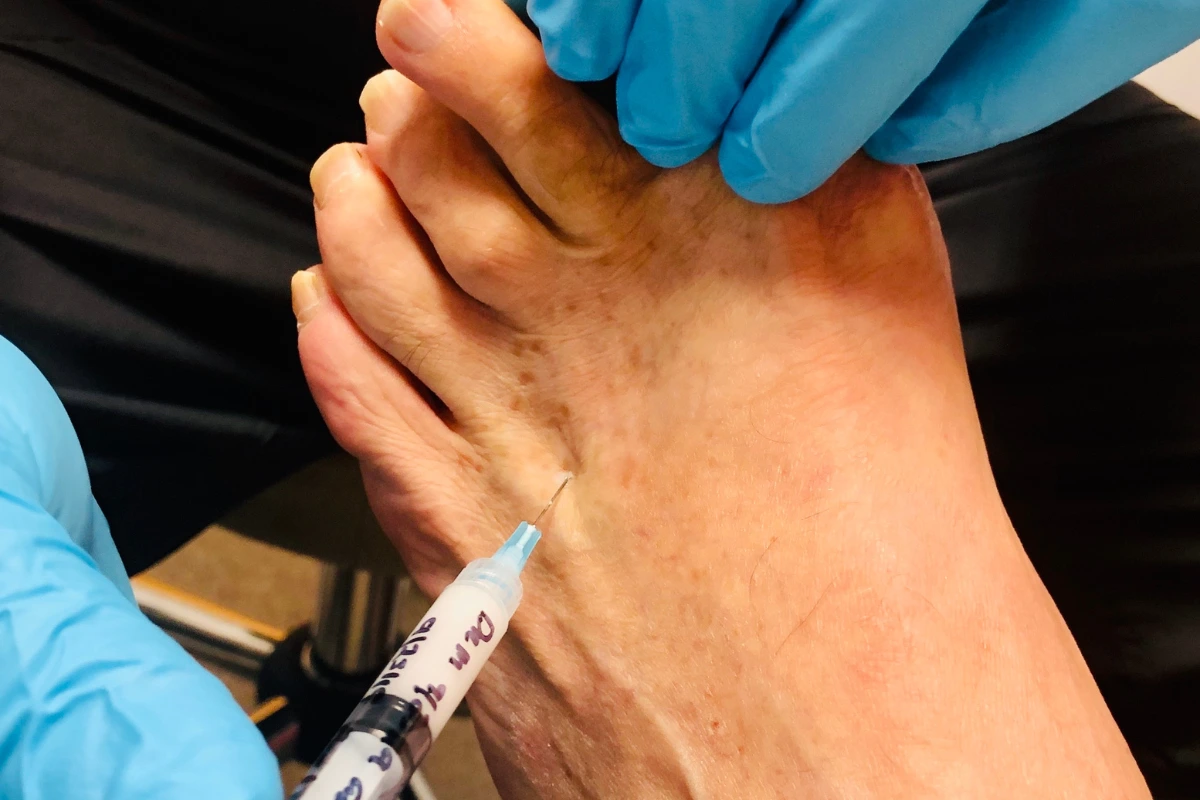
Injection Therapy
When conservative measures don’t provide adequate relief, corticosteroid injections directly into the area around the affected nerve can significantly reduce inflammation and pain. These injections are typically performed in a doctor’s office and may provide relief lasting several months. Corticosteroid injections are a common treatment for Morton’s neuroma and are often considered before exploring surgical options. However, skin discoloration can be a possible side effect of corticosteroid injections and should be considered when discussing treatment options.
Some specialists also offer alcohol injections, which work by essentially “deadening” the nerve to reduce pain signals. This treatment may require multiple sessions but can be effective for patients who want to avoid surgery.
Studies show that conservative treatment approaches relieve pain in approximately 30-50% of patients with morton’s neuroma. Over 80% of individuals with Morton’s neuroma find relief from conservative methods when these approaches are applied consistently and early.
Alternative Therapies for Morton Neuroma
For those seeking additional ways to manage morton’s neuroma symptoms without surgery, several alternative therapies are available that can help reduce pain and improve quality of life.
Extracorporeal Shockwave Therapy
One promising option is extracorporeal shockwave therapy, which uses targeted sound waves to stimulate healing and decrease inflammation around the affected nerve. Many patients experience a noticeable reduction in pain after a series of treatments, making this a valuable tool for those with persistent symptoms.
Radiofrequency Ablation
Another minimally invasive approach is radiofrequency ablation. This procedure uses controlled heat to disrupt pain signals from the affected nerve, providing relief for many people who have not responded to more traditional treatments. Radiofrequency ablation is typically performed by a foot and ankle surgeon or ankle surgeon and can be an effective way to reduce pain without the need for open surgery.
Physical Therapy and Other Modalities
Physical therapy is also a key component of alternative management. A skilled therapist can help you improve foot and ankle mechanics, strengthen supporting muscles, and teach you strategies to relieve pressure on the nerve through our comprehensive services. Some patients find that acupuncture or massage therapy helps manage symptoms of Morton’s neuroma by promoting relaxation and improving circulation in the foot.
Consult a Specialist
It’s important to consult with a foot and ankle surgeon to determine which alternative therapies are most appropriate for your specific symptoms and medical history. With the right combination of treatments, many people are able to reduce pain and return to their normal activities.
Surgical Treatment
When nonsurgical treatment fails to provide adequate relief after several months, surgical treatment becomes a consideration. Morton’s neuroma surgery has high success rates and can provide definitive relief for people whose symptoms significantly impact their quality of life.
Your foot and ankle surgeon at Evolve Health will recommend surgery only after conservative treatments have been thoroughly tried.
The decision to proceed with Morton’s neuroma surgery depends on the severity of your symptoms, how long you’ve had them, and how much they interfere with your daily activities. For more information or to schedule a consultation, don’t hesitate to get in touch with us for details.
Types of Surgical Procedures
The most common surgical treatment is neuroctomy, which involves removing the affected portion of the nerve tissue. This procedure can be performed through two different approaches: To access the nerve, the surgeon can make an incision on either the top or bottom of the foot over the web space.
Dorsal Approach: The surgeon makes an incision on the top of your foot between the affected toes. This approach allows good visualization of the nerve and surrounding structures while avoiding weight-bearing areas of the foot.
Plantar Approach: The incision is made on the bottom of your foot. While this approach provides more direct access to the nerve, it may result in a longer recovery period since the incision is in a weight-bearing area.
Success Rates and Recovery
Surgical treatment for Morton’s neuroma has excellent success rates, with 70-80% of patients experiencing significant pain relief. Some studies report even higher success rates of 80-95% when patients are properly selected for surgery. Surgery is often considered to be the most reliable form of treatment for Morton’s neuroma, with many studies showing an 80 to 95% success rate.
The recovery period varies depending on the surgical approach used. Most patients can return to normal shoes within 3-4 weeks, though complete healing may take 2-3 months. During the initial recovery period, you’ll need to wear a special post-surgical shoe and limit weight-bearing activities. Patients typically return to normal shoe wear within four weeks after surgery for Morton’s neuroma. You can learn more about recovery timelines and tips for foot surgery in our detailed Bunion Surgery Recovery Time guide.
Potential Complications
Like any surgical procedure, neurectomy carries some risks. The most common complication is permanent numbness in the area between the affected toes. This occurs because removing the nerve eliminates sensation in that area, though most patients find this numbness preferable to the chronic pain they experienced before surgery. Approximately 5 to 20% of patients may have symptoms return after successful surgical treatment and require additional treatment.
Other potential complications include:
Infection at the surgical site
Scar tissue formation that could cause new pain
Incomplete pain relief
Recurrence of symptoms (though this is rare)
Temporary swelling and stiffness
Alternative Surgical Procedures
Some surgeons offer less invasive alternatives to traditional neurectomy:
Radiofrequency Ablation: This technique uses heat to destroy the painful nerve tissue without making large incisions. Recovery time is typically shorter than traditional surgery.
Cryoablation: This procedure uses extreme cold to destroy nerve tissue and may be effective for some patients.
Extracorporeal Shockwave Therapy: While not technically surgery, this treatment uses focused shock waves to reduce pain and inflammation around the nerve.
Most people who undergo surgery for Morton’s neuroma are very satisfied with their results and experience dramatic improvement in their quality of life. However, it’s important to understand that surgery permanently changes the anatomy of your foot, so the decision should be made carefully after thoroughly exploring conservative options.
Preparation and Recovery
Preparing for morton’s neuroma treatment starts with a comprehensive evaluation by your foot and ankle surgeon. During your initial visit, you’ll discuss your symptoms, medical history, and daily habits, which helps your provider tailor a treatment plan to your needs. A thorough physical exam will help pinpoint the source of your pain and guide the next steps.
If you’re undergoing non-surgical treatments such as corticosteroid injections, your recovery period will typically involve resting the foot, avoiding activities that trigger symptoms, and following your surgeon’s advice on pain management. Wearing shoes with a wide toe box and steering clear of high heels can help relieve pressure on the foot and support healing.
For those who require morton’s neuroma surgery, the recovery period is usually a few weeks. During this time, it’s important to limit weight-bearing on the affected foot, keep the surgical site clean, and follow all instructions from your ankle surgeon regarding wound care and activity restrictions. Gradually, you’ll transition back to wearing shoes—choosing styles with a wide toe box and good support will help prevent recurrence of symptoms and promote a smooth recovery.
Complications and Prevention
While most people recover well from morton’s neuroma, complications can occur if the condition is left untreated or if treatment is delayed. Potential issues include permanent nerve damage, ongoing pain, and the recurrence of symptoms even after treatment. To minimize these risks, it’s essential to follow your treatment plan closely and seek guidance from a foot and ankle surgeon at the first sign of persistent foot pain.
Prevention starts with smart footwear choices. Avoiding high heeled shoes and tight shoes can significantly reduce your risk of developing morton’s neuroma. Instead, opt for shoes with a soft sole and a wide toe box to relieve pressure on the nerve and metatarsal bones. Maintaining a healthy weight and steering clear of repetitive trauma to the foot—such as high-impact sports or prolonged standing—can also help protect your feet.
Regular check-ups with your ankle surgeon or foot and ankle specialist can catch early symptoms before they progress to more serious nerve damage. By staying proactive and making appropriate lifestyle adjustments, you can help prevent complications and keep your feet healthy.
Frequently Asked Questions
Do I need imaging tests to diagnose Morton’s neuroma?
Most cases can be diagnosed based on your symptoms and a physical examination alone. However, if your symptoms are unclear or don’t respond to initial treatment, your doctor may order an MRI or ultrasound to confirm the diagnosis and rule out other conditions that can cause similar forefoot pain.
How long does it take to recover with conservative treatment?
Conservative treatment typically requires 6-12 weeks to show significant improvement, though some people notice relief within a few weeks of making footwear changes and using proper padding. The key is consistency with treatment and avoiding activities that aggravate your symptoms during the healing period.
Can I continue exercising with Morton’s neuroma?
You can usually continue exercising, but you may need to modify your activities temporarily. Low-impact exercises like swimming, cycling, or elliptical training are generally well-tolerated. If you run or play sports that involve jumping, you might need to reduce intensity or take a break until your symptoms improve.
Will orthotics cure my Morton’s neuroma?
Orthotics and metatarsal pads can provide significant relief and may prevent symptoms from worsening, but they typically don’t “cure” the condition completely. They work by reducing pressure on the affected nerve, which allows inflammation to decrease and symptoms to improve. Many people find they can manage their symptoms well long-term with proper orthotics and footwear.
When should I consider surgery for my foot pain?
Surgery becomes an option when conservative treatments haven’t provided adequate relief after 3-6 months of consistent use, and your symptoms significantly interfere with daily activities. Your surgeon will evaluate factors like the severity of your pain, how long you’ve had symptoms, and whether imaging confirms the diagnosis before recommending surgical treatment.
The decision to have surgery should be made carefully, considering that while success rates are high (70-80%), the procedure does result in permanent changes to foot sensation. Most people who choose surgery are very satisfied with their results and experience dramatic improvement in their quality of life.
Conclusion
Morton’s neuroma is a treatable condition that doesn’t have to limit your activities long-term. Whether through conservative management or surgical intervention, effective treatments are available to help you return to pain-free walking and active living. The key is recognizing symptoms early and working with healthcare professionals to develop an appropriate treatment plan.
If you’re experiencing persistent pain in the ball of your foot, especially the sensation of walking on a marble or pebble, don’t wait to seek help. Early treatment often leads to better outcomes and can help you avoid more invasive procedures down the road. With the right approach, you can successfully manage Morton’s neuroma and get back to the activities you enjoy.