Understanding Toenail Fungus
Toenail fungus, or onychomycosis, is a common fungal infection affecting nails, caused by fungi thriving in warm, damp places like swimming pools and sweaty shoes. It leads to nail discoloration, thickening, and brittleness, sometimes causing pain or skin infections if untreated.
Early signs include white, yellow, or brown spots under the nail tip. Treatment options range from oral antifungal medications and topical creams to home remedies like tea tree oil and apple cider vinegar. Over-the-counter products such as creams and sprays may help mild cases.
Choosing the best treatment depends on infection severity. If initial treatments fail, laser therapy or combination approaches might be recommended.
Causes and Risk Factors Of Toenail Fungus
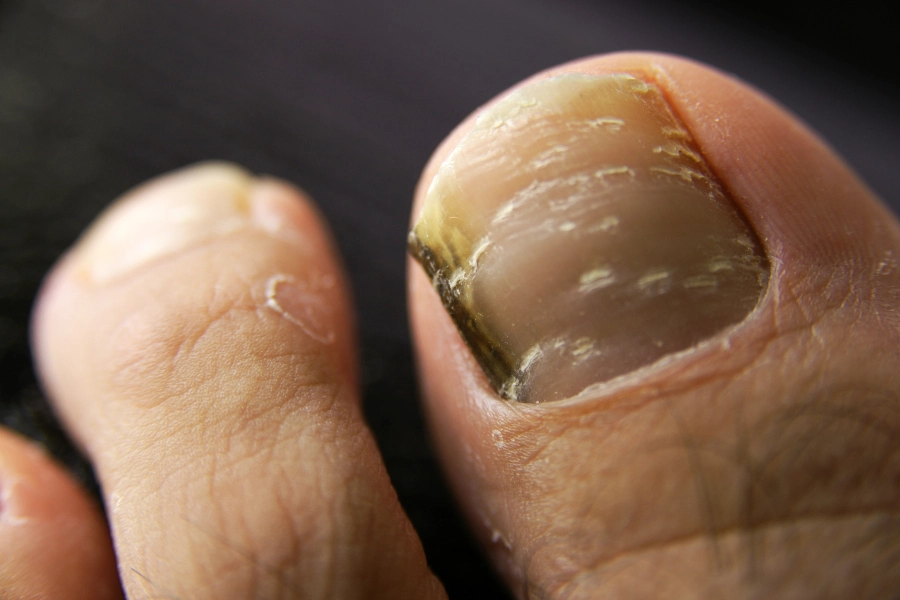
Toenail fungus develops when fungal organisms (dermatophytes, yeasts, or molds) invade the nail. Nail fungi are a common cause of toenail fungal infection, leading to changes in nail appearance and potential health risks. Dermatophytes are responsible for 90% of toenail fungal infections.
They thrive in warm, moist environments, which is why swimming pools, public showers, and damp shoes are common sources. Nail fungi thrive in warm, moist, and dark environments, making it essential to keep feet dry and clean to reduce the risk of infection. You may be more prone to toenail fungus if you have:
Athlete’s foot, a common fungal infection of the skin, can easily spread from the skin to the toenails. Having athlete’s foot increases your vulnerability to toenail fungus, especially in damp environments or when wearing improper footwear, as the two conditions are closely interconnected.
Nail injuries that expose deeper tissue.
Diabetes, circulation problems, or weakened immunity.
Chronic conditions like nail psoriasis or other skin conditions.
A habit of walking barefoot in public locker rooms without shower shoes or flip flops.
Symptoms of Toenail Fungus

Symptoms develop slowly, often starting with minor discoloration and progressing to more severe changes. The first sign of a fungal toenail infection is a small, white, yellow, or brown spot under the tip of the nail. Watch for:
Yellow, brown, or white patches on the affected toenail.
Thickened or distorted shape of the affected toenail.
Nails that become brittle or crumble at the edges.
A foul odor or dull appearance compared to a healthy nail.
Separation of the affected nail from the nail bed.
If you notice these changes, consult a toenail fungus doctor for evaluation before the infection worsens.
How a Podiatrist Diagnoses Nail Fungus
Diagnosis is more than just looking at the nail; the goal is to confirm a toenail fungal infection. A podiatrist may:
Perform a physical exam of the nail’s surface, thickness, and surrounding skin.
Take a sample of the infected nail for microscopic analysis or culture, confirming fungal growth.
Rule out other nail conditions, such as psoriasis or bacterial infections, that mimic fungus.
Accurate diagnosis is critical, since using the wrong treatment wastes time and increases recurrence.
Podiatrist-Recommended Treatments For Toenail Fungus
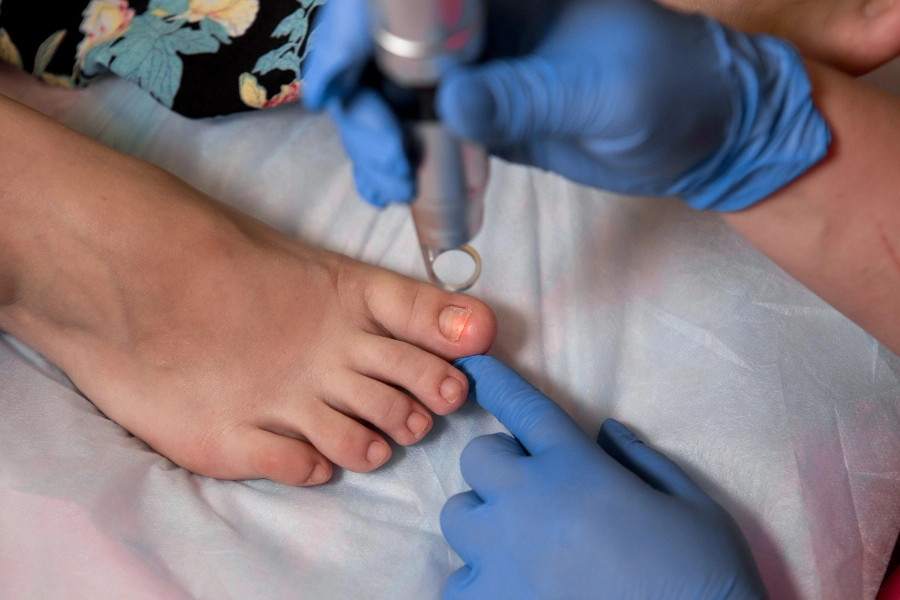
Topical Treatments
Mild infections may respond to topical antifungal medication, such as ciclopirox nail lacquer, efinaconazole, or tavaborole topical solution.
Another topical option for mild to moderate cases is a medicated cream, which is often available over the counter and requires consistent application.
These solutions and creams have antifungal properties that help inhibit or kill the fungi causing the infection.
They penetrate the surface of the nail slowly, so treatment can last 9–12 months. They work best when the nail is thin or after professional nail debridement, which allows better penetration.
Oral Antifungal Medications
For moderate to severe infections, oral treatment is usually recommended; these are prescription drugs for toenail fungus. Drugs like terbinafine, itraconazole, and fluconazole are highly effective, often achieving cure rates above 70 percent.
They work from within the bloodstream, reaching the nail matrix where fungal growth begins. Oral antifungal medications like itraconazole and terbinafine usually take about 12 weeks to clear the fungus.
While oral antifungals are powerful, they may cause mild gastrointestinal symptoms and require monitoring for potential side effects. If these drugs are not effective, a doctor may consider other medications as part of the treatment plan.
Laser Toenail Fungus Treatment
One of the newer options is laser treatment, which uses concentrated light energy to heat and destroy fungal cells. Laser treatments are a modern, non-invasive category of options for toenail fungus, offering an alternative when topical and oral treatments are insufficient. Sessions are quick and painless, with no systemic side effects.
However, multiple visits are often required, and long-term success rates vary. Laser treatment for toenail fungus typically requires multiple sessions spaced weeks apart.
Lasers are best for patients who cannot take oral antifungals or who want to combine them with other therapies for stronger results.
Professional Nail Debridement
A podiatrist can carefully trim or thin diseased nail material. This instantly reduces fungal burden, improves appearance, and enhances the effectiveness of topical medications. Keeping nails trimmed may reduce pressure and pain while treating toenail fungus. While not a cure on its own, debridement is often part of a comprehensive treatment plan.
Combination Therapy
The most effective approach is often a combination therapy. For example:
Oral antifungals with topical solutions.
Debridement with topical application.
Laser therapy is paired with prescription medication.
By attacking fungus from multiple angles, combination therapy achieves the highest success rates and lowers the risk of recurrence.
Home and Natural Remedies

Some patients try home remedies for mild cases. These include tea tree oil, apple cider vinegar foot soaks, or even Vicks VapoRub, which has shown antifungal activity in small studies.
Baking soda is another popular option; it can be used as a foot soak or made into a paste to help manage mild nail fungi by absorbing moisture and supporting antifungal treatment.
A foot soak with ingredients like apple cider vinegar, Listerine, or baking soda is a common home remedy for toenail fungus. Rubbing alcohol can also be used to disinfect toenails and surrounding areas as part of a home hygiene routine to help prevent the spread or recurrence of fungal infections.
While these options may improve appearance temporarily, they rarely eliminate the infection fully. OTC products for toenail fungus are usually more effective for mild cases and may take months to work. They are best used alongside medical treatment, not as replacements.
Best Treatment Options for Infected Nail
When it comes to treating an infected nail caused by toenail fungus, the best treatment options depend on how advanced the fungal infection is and your overall health. For many patients, a combination of oral antifungal medication and topical treatments offers the most effective results.
Oral antifungal drugs like terbinafine and itraconazole are commonly prescribed by foot doctors to treat nail fungus from the inside out, targeting the source of the infection and helping to prevent it from spreading to other nails.
Topical treatments, such as ciclopirox nail lacquer and tavaborole topical solution, are applied directly to the affected nail. These antifungal drugs work by attacking the fungus on the surface and within the nail, and are often used alongside oral antifungal medication for a comprehensive approach.
Consistency is key—these treatments may need to be used for several months to fully clear the infection and allow a healthy nail to grow in.
In addition to medication, simple lifestyle changes can make a big difference. Keeping your feet clean and dry, wearing shoes that fit well, and avoiding sharing personal care items like nail clippers or towels can help prevent the spread of toenail fungus.
Consulting a foot doctor ensures you receive the best treatment plan tailored to your specific nail condition, increasing your chances of a successful recovery and reducing the risk of recurrence.
Evolve Health Clinic Recommendations
The Evolve Health clinical overview of toenail fungus treatment emphasizes a well-rounded approach that combines medication with smart lifestyle habits. For those with mild fungal infections, we suggests starting with topical treatments such as antifungal nail polish or medicated cream. These options can help manage symptoms and support the growth of a healthy nail, especially when the infection is caught early.
For more persistent or severe cases, Our Doctors recommend oral antifungal medications or laser treatment, which are more effective at treating toenail fungus that has penetrated deeper into the nail.
They also highlight the importance of preventative steps such as wearing shower shoes or flip-flops in public areas, keeping feet clean and dry, and not sharing nail care tools or nail polish to reduce the risk of reinfection.
By following these evidence-based recommendations and working closely with a healthcare professional, you can create a treatment plan that addresses both the current fungal infection and helps prevent future outbreaks. This comprehensive strategy is key to restoring clear, healthy nails and maintaining long-term foot health.
Prevention Tips
Preventing reinfection is just as important as treatment. Prevention strategies are essential to prevent toenail fungus from recurring. Practical steps include:
Wearing shower shoes in public places like locker rooms can help prevent toenail fungus.
Keeping feet dry and changing socks frequently.
Cleaning nail tools and avoiding shared nail polish.
Trimming nails straight across to prevent trauma.
Choosing breathable footwear and avoiding prolonged damp shoes.
Treating athlete’s foot promptly, as the infection can spread from the skin to the nails and increase the risk of toenail fungus.
Using antifungal powder in shoes can help keep them dry and reduce the risk of toenail fungus.
These habits reduce the risk of new fungal growth once a healthy nail has replaced the old one.
When to See a Doctor for Toenail Fungus
Not all fungal infections require immediate treatment, but you should see a podiatrist if:
The nail becomes painful, thick, or disfigured.
You have diabetes or circulation issues.
Symptoms spread to multiple nails or the skin.
Home remedies and over-the-counter products fail.
Visit Evolve Health Locations to explore tailored treatment options. Our specialists also provide advanced nail care and injury trauma care for complex foot conditions. Recurrence rates for toenail fungus after treatment can be as high as 40 percent, so ongoing care and prevention are crucial.
Conclusion
Toenail fungus may be common, but it doesn’t have to be permanent. With options ranging from topical solutions and oral medications to advanced laser toenail fungus treatment, podiatrists can create effective strategies that match your needs. The key is patience — even the best therapy requires months for a new nail to grow out.
We design personalized treatment plans to restore your nails and prevent reinfection. Book now to take the first step toward healthier feet.
FAQs
How long does toenail fungus treatment take?
Treatment requires patience. Even after the fungus clears, it can take 6–12 months for a new nail to fully grow.
Is laser toenail fungus treatment effective?
Yes, but results vary. Lasers work best when combined with other treatments.
Can I wear nail polish during treatment?
Regular polish may trap moisture. If you use antifungal nail polish, ask your doctor if it is safe during treatment. Antifungal nail polish can take six months or more to show improvement and is less effective than systemic medications.
Do home remedies like tea tree oil or apple cider vinegar work?
They may provide mild improvement, but they rarely cure fungal infections on their own.
When should I see a toenail fungus doctor?
If nails become painful, thick, or unsightly, or if you have diabetes, see a podiatrist for safe and effective care.